Opioids are the Latest Plague in the US. Now that the pharmaceutical industry has created an army of addicts, the drug cartels have leaped in to fill the gap. They are flooding America with heroin and fentanyl. We wanted to find out how it was possible for this unprecedented crisis to come about, and why medicinal cannabis offers a glimmer of hope.
The morgue in Dayton, Ohio, is full to bursting. Some days there are lifeless corpses arriving every hour. “We are at full stretch”, confirms the responsible coroner in response to an enquiry by the New York Times..
Along with its neighbours Kentucky, Pennsylvania and West Virginia, the state of Ohio is one of the areas in the country hit hardest by the opioid crisis.
Videos of addicts collapsing in public – in supermarkets, at filling stations, on buses – are circulating on the Internet. The scale of the crisis is such that Donald Trump declared a state of national emergency in the summer of 2017.
The US is drowning in pain.
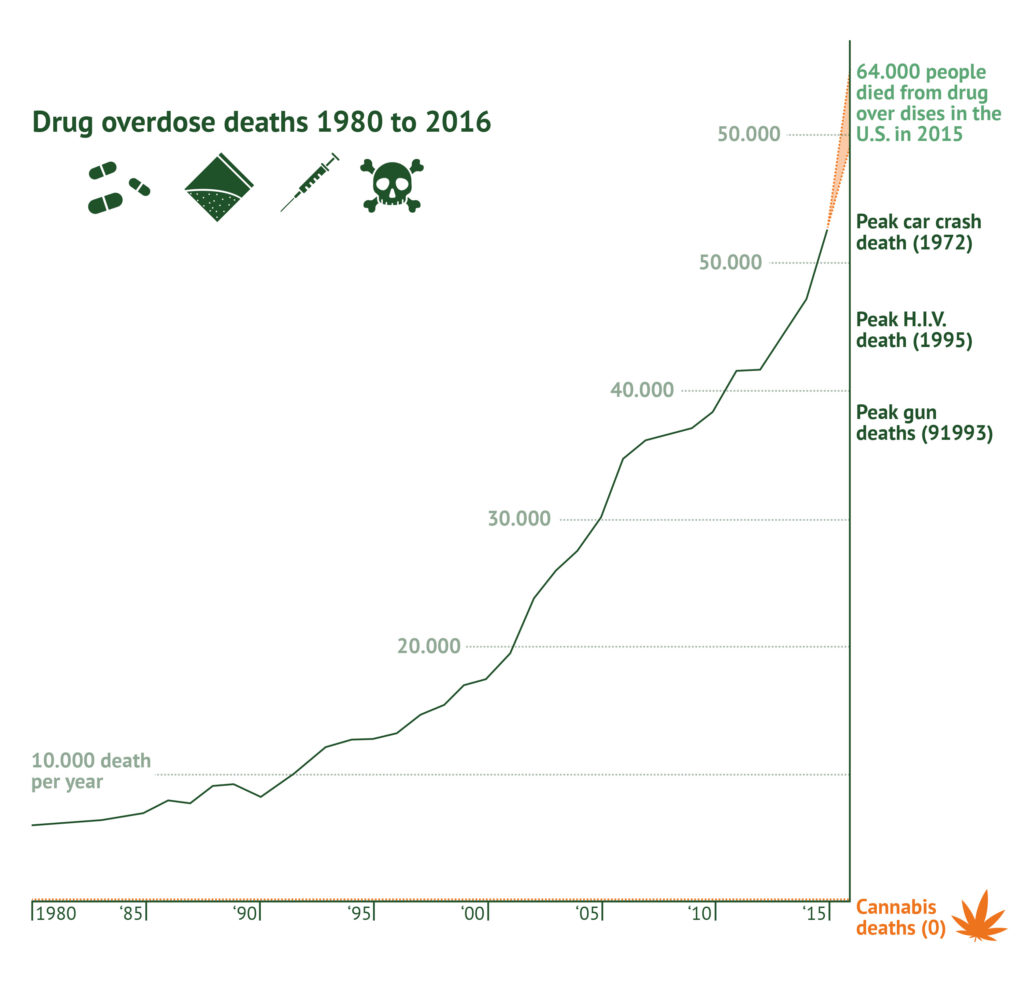
The figures speak for themselves: In 2016, 64,000 people died of an overdose. That is more deaths than at the peak of the AIDS epidemic, and more than the wars in Vietnam, Iraq and Afghanistan combined.
Unlike in the past, the current drug epidemic is not an inner-city problem. Mainly the suburbs and rural areas have been hit. Places that have never really recovered from the 2008/09 economic crisis.
And unlike in the era of crack, it is the white people of the country that are affected. Millions of them are addicted to painkillers containing opioids, heroin and fentanyl.
Cannabis offers hope, but cannot provide a cure for the opioid epidemic
First the good news: Multiple studies and patient stories refer to the pain-relieving qualities of THC and CBD. As part of a current study, the University of New Mexico is researching whether patients with chronic pain could reduce their opioid consumption by using cannabis. The initial results are encouraging.
In terms of the effect of cannabinoids on opiate addiction, there are some interesting pointers from animal experiments. In one study, CBD blocked the reward effect of morphine. In another study, CBD reduced rats’ behaviour in seeking heroin. The delayed positive effect could still be observed two weeks later, which might help prevent relapses.
A research initiative at UCLA also gives grounds for hope. According to Jeff Chen, who is heading up the research, there are indications that cannabis might help people, to give up pills and heroin: “Where there is an element of chronic pain, cannabis can address the chronic pain element. We also know that opioid addicts have a lot of neurological inflammation, which we believe drives the addiction cycle. Initial studies indicate that cannabinoids reduce inflammation in the brain.”
Five years ago, a widely cited study showed that states with a medicinal cannabis programme report up to 25% fewer opioid-related deaths than those with no programme. The research was conducted between 1999 and 2010. But if we look at 2010 to 2017, the results look rather different. States with medicinal cannabis report 23% more deaths. This is according to a new study from June 2019.
Chelsea Shover, co-author of the study and researcher at Stanford University, does not believe that cannabis can prevent deaths from opioid overdoses. The physician Professor Chinazo Cunningham agrees: “Cannabis is certainly no miracle weapon. It is not a cure for the opioid epidemic.”

It would be naive to believe that cannabis is a solution for the opioid crisis. But that’s not to say that it does not have a part to play in pain relief, as shown in the studies above and anecdotal evidence.
Cunningham agrees. She is keen to drive the research forward. But as long as cannabis is prohibited at the federal level, her hands are tied. The US government shows no signs of relaxing the ban on cannabis – much to the delight of the pharmaceutical industry, which is held mainly responsible for the crisis. Is there any truth in this accusation?
$$$$$$$$$$$$$ It is Bonus Time in the Neighbourhood!
The 50s were a time of new beginnings. Nothing seemed impossible in the land of endless opportunity. While the first VW Beetles were being constructed in Germany, Americans were already driving big cars to go shopping. Nowhere was this feeling of opportunity more obvious than in New York. Manhattan went through an unprecedented construction boom, the towers in Midtown reached for the sky again.
Reaching for the sky was what the three Sackler brothers Arthur, Mortimer and Raymond also wanted to do. In 1952, they purchased the small pharmaceutical company Purdue Frederick, which became the cornerstone for their later wealth. The first years were difficult; it was not easy to make much money with laxatives and earwax removers. What looked more promising was the painkiller business.

In 1996, the family company, now renamed Purdue Pharma, launched OxyContin, a strong painkiller, based on oxycodone, an opioid. Oxycodone was already being used in other painkillers, but not in its pure form, and not in such a high concentration. They brought to market not just 10 mg pills but also some with 80 and 160 mg of oxycodone, which Barry Meier, in his book “Pain Killer: A Wonder‘ Drug´s Trail of Addiction and Death, described as follows: “In terms of narcotic firepower, OxyContin was a nuclear weapon.”
The FDA (Food and Drug Administration) had classified OxyContin as a Class II substance, for which by definition there is a high risk of abuse and addiction. Nevertheless, Purdue marketed its pills as a cure for all types of pain. The press release for its launch claimed: “The fear of addiction is overstated.” A patented mechanism that ensures that the active ingredient is released only slowly (“Contin” stands for continuous release), was intended to prevent abuse.
In 1996, Purdue started a large-scale advertising campaign to convince doctors, wholesalers and consumers of the benefits of the new magic pills. The campaign shows a happy grandmother who has her back pain under control thanks to OxyContin and can at last play with her grandchildren again.
Doctors’ surgeries were supplied with nearly 35,000 starter coupons that could be exchanged for free pills. Their own reps were persuaded by the big money. Literally. The subject of an email was: “$$$$$$$$$$$$$ It is Bonus Time in the Neighbourhood!” Meanwhile, Purdue financed thousands of training courses, conferences and associations.
Who doesn’t have any yet, who wants more?
The well-oiled marketing machine hit the bullseye. Initial scepticism gave way to enthusiasm. Some doctors started prescribing the colourful pills like Smarties. Their patients were happy and came back for more. This reflects a tragic weakness of the US health system: it is designed to do what patients want and not necessarily what is good for them.
Very soon after its launch on the market, the first OxyContin pills showed up on the black market. It also quickly became known how to release the whole of the active ingredient at once. You simply ground up the pills. Users started to sniff and to inject “oxys”. But for many, just taking them orally led straight to addiction.
In 2007, Purdue Pharma pleaded guilty to misleading the public about OxyContin’s risk of addiction. The company was sued for 634 million dollars. A drop in the ocean, compared to the 35 billion dollars that the Sacklers apparently earned with their blockbuster drug. What happened next?
Purdue invested more money than ever in its lobbying efforts. Between 2006 and 2015, the pharmaceutical industry spent nearly 900 million dollars on lobbying – eight times as much as the gun lobby over the same period.
America’s appetite for opioids was far from being satisfied. The sales figures shot up. And the merry-go-round just kept on turning. In 2012, doctors issued 259 million prescriptions for medicines containing opioids – enough to hand every adult in the country a bottle of pills! This was the peak of the prescription frenzy.
Pills first, then heroin
Once the US CDC (Center for Disease Control and Prevention) had issued new guidelines in 2016 for the prescription of opioids, the number of prescriptions began to fall.

Now, what happens in any market where demand exceeds supply? Prices rise. That in turn got the Mexican drug cartels interested. They flooded America with cheap heroin.
In doing so, the so-called “Xalisco Boys” acted in much the same manner as the Purdue marketing men before them. Based on publicly available statistics, they targeted their product on poor areas with low education, where more than average accidents at work were recorded. They distributed free samples there when they launched in the market.
The strategy worked: around a million Americans now regularly consume heroin. Around 80% of the new users started out on their addiction with legal painkillers.
Heroin is made from the milky sap of the opium poppy that is hard to grow in Mexico. To be able to handle the huge demand, the cartels began to mix fentanyl with the heroin. Fentanyl is a completely synthetic opioid, that is fairly easy to obtain on the Chinese black market.
Danny, a long-term heroin user from Philadelphia remembers when the new drug first appeared on the market: “People did not know what they were dealing with… As soon as the dealers saw that people were dropping like flies, they thought: “We’re doing something wrong”. Now they mix it better.” Unfortunately, we can only partly agree with Danny.
Almost all the users who ended up in the morgue in Dayton died from a fentanyl overdose. There is no end in sight. Experts assume that the number of deaths from drugs will continue to climb.
Land of endless opportunities
It was Patrick Radden Keefe of the New Yorker who exposed Purdue Pharma’s unscrupulous business dealings. Under the name “Mundipharma”, the Purdue owners are now active mainly in countries such as China, Mexico and Brazil. Keith Humphrey, a psychiatrist at Stanford University, warns about the globalisation of the opioid crisis.
The Sacklers are leading a double life. In public, they present themselves as good guys and use their blood money to finance world renowned museums, galleries and universities. But in the meantime, wide opposition is growing. In the summer of 2019, the Louvre Museum and the London Library declared that they would not accept donations from the Sackler family. Other renowned art institutions, including the Tate in London and the Guggenheim in New York, had already stated they would not accept any philanthropy from the Sacklers.
The protest movement is led by Nan Goldin. The world-famous photographer herself became an addict through taking OxyContin. After a painful withdrawal, she has kicked the drug habit. And declared war on the Sacklers. On Twitter and Instagram she demands that the family invest a part of their fortune in addiction treatment and prevention programmes.
Purdue Pharma is now also in the crossfire of the American authorities. Numerous states and municipalities accuse the company of downplaying the risks and marketing OxyContin too aggressively. They are claiming compensation amounting to 10 to 12 billion dollars. Having reached a settlement with the claimants, Purdue Pharma filed for bankruptcy in September 2019.
While we may welcome Nan Goldin’s campaign against the Sacklers, it would be an oversimplification to blame the pharmaceutical industry alone for this problem. America’s opioid crisis is first and foremost a social crisis. A lack of prospects and boredom are the perfect conditions for addiction to flourish.
What people need are jobs that offer the chance of a decent life. That includes access to a functioning health care system. In rural areas, the medical and therapeutic treatment which addicts desperately need, is in shambles. Speech therapy and alternative treatments, such as cannabis therapy, barely exist.
- Disclaimer:This article is not a substitute for professional medical advice, diagnosis, or treatment. Always consult with your doctor or other licensed medical professional. Do not delay seeking medical advice or disregard medical advice due to something you have read on this website.











This is all very interesting and probably known for years and years but no one dare let the medicinal benefits get out because of all that pharmaceutical and booze sin tax cash. I wonder how many people had to die before they finally said “ok we better let them release this info” and legalize it already……. Just sayin…….
2nd day on cbd’s. have quit from taking opiates at least twice in the now about ten years I have been using. a HUGE reason I don’t quit bcuz when I go w/out opiate I cannot work due to the HORRIBLE withdrawal symptoms. but I am sick of being a slave to it… took a chance on my maryj smoker hubby’s suggestion on taking cbd. it works! my job involves a lot of reading. I’m physically here but still hard to concentrate (yes I’m at work now). I’ll make up my time by working off the clock after hours here and there this week. I figure if I can get rid of the withdraw stuff I can finally do what I’ve wanted to do since I’ve known that the opiates were using me and not me using opiates. I’ve done things I’ve NEVER thought I’d do before all in an effort to help me score. I would never wish that jail to anybody; the jail within your own body! We’ll see but so far the withdrawal symptoms (cold/hot sweats, irritability, anger, anxiety, depressed) are in check. I started experiencing having to go to the bathroom which kind of brought me joy because I felt like “this stuff is working, the opiate crap is leaving my body”. So if the worst is I have gross shits and some cold/sweats here and there, compared to what I’ve experienced in my past attempts to stop… Shit, Ill take it! rust me, I can take 15-20 of the 10mg pills daily! EASY! I love opiates, how they take pain away, how they make me feel better… but it was taking over my life. That was the relationship I’ve cared about for the last 10 years over my beautiful family. I have vacations I can’t remember because I’d also use Xanax just because and those things make me very forgetful–I didn’t even know how bad I was forgetting things. I just didn’t realize how I’d gotten out of control. I can never get time back… but I have something to look forward to. The other day I cried, It felt good to cry because at least I was feeling something, I haven’t had any feelings for so long… just a numb, high junkee. Forget that, never again!!!
Great posts! i really thank for your all information you write about opiate drugs. It`s really helped me! Thanks for sharing it.
Would any of the synthetic thc like jwh compounds help alleviate opiate withdrawals. Havent found anything on that. Doubting it would ecspecially it having its own dependancy but just a week of synthetic thc shouldnt cause addiction worse than opiates can. Im an opiate addict and i also smoked jwh for 9months straight and had no withdrawals. I dont think jwh is safe but maybe if your carefull iy could help you through the worst..
After 10+ years of opiate use 4 months ago I opt out from using them with my Doctors blessing. Now I use cannabis oil in my coffee and edibles and smoke a little. Even my daughter has notice a change for the better. I feel better and get a lot more done.
I’m an struggling addict of opiate pain killers now for 12 years and would love to find a strain of marjiauna that gives the same feeling as an opiate.
Really interesting article,I have been a heroin user/methadone addict for the past 20 years,The past 18 months i have been clean of street drugs and have reduced methadone by 55%,I made the decision to stop, but armed myself with a grow tent to help with the bumpy ride,I have tried before but always failed,this time with cannabis i feel much stronger/determined and confident.The “Hobby” side of the grow has also been very important in keeping my mind off the shit,I wish i could talk to more understanding professionals about this,Cannabis is also having amazing effects on my diabetes for the better as well as giving some pain release to my feet which suffer due to complications from nerve damage from diabetes.
Cannabis is really helpful in curing various diseases.The two main components from the cannabis plant that are of medical interest are THC and CBD. Doctors prescribe medical cannabis to treat diseases like Muscle spasms caused by multiple sclerosis, Nausea from cancer chemotherapy, Poor appetite and weight loss caused by chronic illness, such as HIV, or nerve pain, Seizure disorders