The current existing literature demonstrates a very clear connection between the endocannabinoid system and liver cirrhosis, all the way through to end-stage liver disease. However, there is no consensus as to whether cannabis use can lead to liver cirrhosis, or whether it’s a potential treatment for the condition.
The liver can be thought of as the human body’s giant detoxifying organ. It plays an important role in the metabolism of drugs, alcohol, medications and toxins arriving from the gastrointestinal tract. Unhealthy lifestyle factors, excessive alcohol or drug consumption or certain hepatic viruses (such as hepatitis) all contribute to the degradation of the liver. The final result of such degradation is liver cirrhosis: the irreversible and extreme scarring of the liver.

There is a lot of controversy surrounding cannabis use and liver cirrhosis. The endocannabinoid system is heavily implicated in liver cirrhosis as modern medicine as confirmed. The distribution of CB1 and CB2 receptors in the liver and their activities are thought to play a major role in the progression of liver disease, fibrosis and cirrhosis. Despite this understanding, there is conflicting evidence about how phytocannabinoids (such as THC and CBD) affect this physiological process and whether they are beneficial or a contributing factor. Let’s investigate.
What is liver cirrhosis, what causes it, and what are the available treatments?
Cirrhosis refers to the late, chronic stage of scarring of liver tissue. In the initial stages, the scarring is called liver fibrosis. It results from persistent, chronic insult to the liver, causing the liver to undergo constant wound healing, and finally leading to permanent scarring. Cirrhosis ensues when scarring of the liver has become so severe that aspects of the liver’s function become compromised. Chronic liver cirrhosis results in disruption of the liver’s structure, and can ultimately lead to liver failure.
Liver disease is responsible for up to 2 million deaths per year, 1 million of which are directly linked with liver cirrhosis complications. Liver cirrhosis is currently the 11th most common cause of death worldwide.
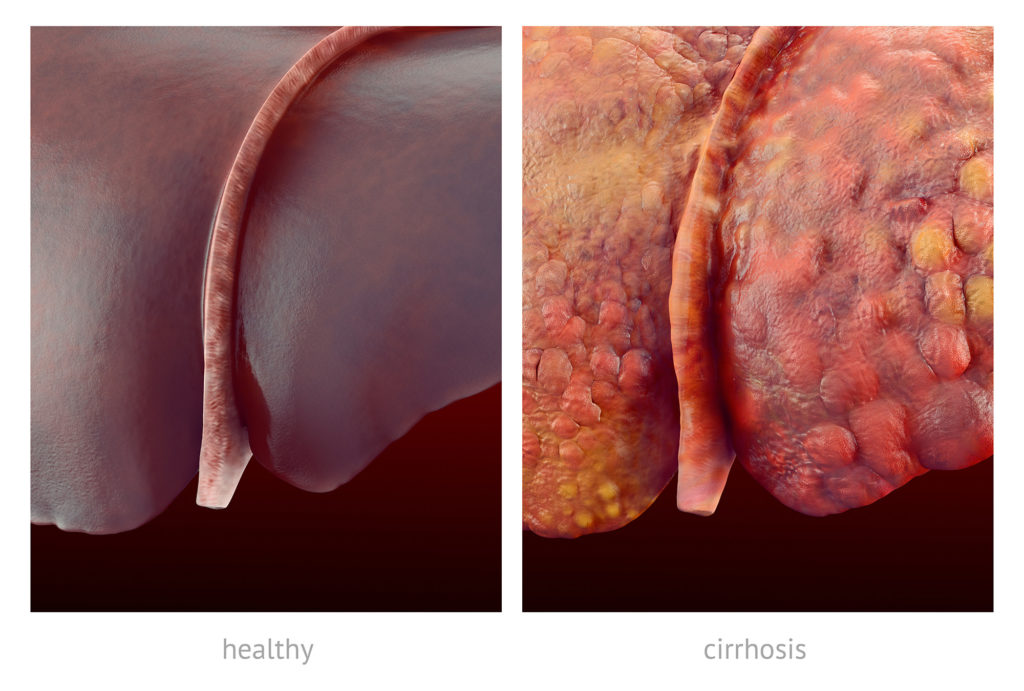
The global most common causes of liver cirrhosis are alcohol abuse and hepatitis C, although other liver conditions can also lead to cirrhosis. One such condition is fatty liver disease, which is most commonly caused by obesity or excessive alcohol consumption.
Until now, there are no known cures for liver cirrhosis. The condition is characterised by scarring, which is typically irreversible irrespective of where it happens on the body. Just like any other scarring, advanced liver scarring is considered irreversible, although removing the causative factor can slow down the progression of the disease.
Because of the worldwide prevalence of liver cirrhosis, it is a highly researched condition. More recently, the endocannabinoid system has been under close scrutiny as a potential treatment target. This is because cirrhosed livers display different behaviour with respect to endogenous cannabinoids and cannabinoid receptors when compared to normal livers. Herein drives the major controversy about whether cannabis is a causative factor for liver cirrhosis or whether it is a potential treatment opportunity.
The endocannabinoid system and liver cirrhosis
Quite a considerable amount of experimental studies and clinical observations have noted altered activity of endocannabinoids and cannabinoid receptors during liver cirrhosis. It has been found that the endocannabinoid system (EC) is highly active in cirrhosed livers, with extremely high cannabinoid receptor expression during the progression of the disease. However, cannabinoid receptor expression is very low or completely absent in normal, healthy livers.
In a 2011 study published in the British Journal of Pharmacology, researchers demonstrated that both CB1 and CB2 receptors are up-regulated in samples of cirrhotic liver. The researchers found that CB1 receptor activation (agonism) intensifies fibrogenesis (creation of scar tissue), while CB2 receptor activation inhibits the progression towards fibrosis. During the same study, the researchers also demonstrated that the CB2 receptor is integral in the regenerative process after acute liver injury.
These findings seem to be supported by other academic literature. In rodent models, CB1 and CB2 receptors were deleted entirely from cirrhosed liver cells to assess the effects of complete deletion. Appropriately, deletion of the CB1 receptor demonstrated a marked improvement of liver fibrosis and deletion of the CB2 receptor increased inflammatory scores, increased collagen deposition and liver fat.
These findings were again supported by another study by Julien et al. in 2005. The team showed that activation of the CB2 receptor resulted in antifibrogenic activity, supporting the importance of the CB2 receptor in the regeneration process following liver fibrosis.
Aside from cannabinoid receptors, endogenous cannabinoids also have an important mechanistic function in liver cirrhosis. Endogenous cannabinoids such as AEA and 2-AG naturally contribute to the behaviour of CB1 and CB2 receptors. In this way, they may instigate some of the antifibrogenic and profibrogenic activities of the receptors themselves.
AEA has been demonstrated to reduce fibrogenesis in liver cirrhosis. Conversely, 2-AG potentially mediates fibrogenesis completely independently, without interaction with CB receptors. However, at higher doses, 2-AG induces cell death of hepatic stellate cells (HSCs), and might therefore inhibit fibrogenesis. Heightened HSC activity is thought to promote fibrogenesis and fibrosis.
The aforementioned research demonstrates that the endocannabinoid system is implicated in just about every stage of cirrhosis pathology. This includes potential complications of cirrhosis, such as hepatic encephalopathy. This is a neuropsychiatric condition specifically caused by damage to the liver’s function. Modern research is beginning to show that exogenous cannabinoids such as THC and CBD interact with the endocannabinoid system in such a way as to treat symptoms of hepatic encephalopathy. However, this will be discussed in greater detail later on in this article.
Cannabis and the progression of liver cirrhosis
The research surrounding cannabis’ potential to increase the risk of liver cirrhosis has been varied and controversial. For the most part, results are completely conflicting.
At the beginning of 2019, Dr Igor Koturbash and other researchers at the University of Arkansas tested for the hepatotoxic dose of CBD. The models were rodents, to which CBD was administered first in an acute toxicity phase and secondly in a sub-acute toxicity phase. In the first phase, mice were administered a single dose of up to 2460 mg/kg of CBD. During the sub-acute phase, mice were administered lower doses (up to 615 mg/kg) over 10 days. Interestingly, in the sub-acute phase of testing, 75% of mice died or were dying within 72-96 hours. The result was profound liver hepatotoxicity.
It’s important to remember that these are considered the levels of hepatotoxicity of CBD, and does not suggest that all CBD consumption is hepatotoxic. The media’s response to this research was that “CBD could cause liver damage”, but in fact, researchers were simply looking for which maximum dose may lead to liver toxicity. Essentially, researchers concluded that CBD interacts with the same metabolic pathway as many other substances and drugs, and this may contribute to its hepatotoxicity. Finally, the researchers suggested a standard by which dosage could be calculated for each person to mitigate any chance of hepatotoxicity.
In 2005, French researchers investigated the effect of cannabis smoking on the progression of fibrosis in chronic hepatitis C patients. The researchers included a total of 270 patients and included in their analysis other factors such as excessive alcohol intake, tobacco smoking, age at the time of liver biopsy, and steatosis. The researchers concluded that severe fibrosis was predicted by daily cannabis use, independent of the other factors. They advised that patients with chronic hepatitis C should refrain from using cannabis regularly.
These findings were supported by another 2008 study including 204 patients with hepatitis C. The study was conducted at the University of San Francisco and used baseline data from a prospective, community-based cohort study. The primary predictor was cannabis use and the results were calculated using a fibrosis score on biopsy. The team also concluded that daily cannabis use was strongly associated with moderate to severe fibrosis for patients already diagnosed with hepatitis C.
In 2013, at McGill University in Quebec, Canada, a team of researchers revealed results contradictory to those mentioned above. In this study, the team evaluated 690 individuals who were diagnosed with HIV and hepatitis C coinfection who did not have significant fibrosis or end-stage liver disease. This was the baseline. At the baseline, 53% had smoked marijuana in the last 6 months, and were consuming an average of 7 joints per week, while 40% were daily users.
Researchers found that each additional 10 joints per week slightly increased the risk of progression towards end-stage liver disease or cirrhosis. However, they also found that when the exposure to cannabis was lagged to 6-12 months before the HIV/hepatitis C diagnosis, cannabis was no longer associated with progression of fibrosis or cirrhosis. Similarly, they found that whatever higher risk of cirrhosis was associated with cannabis use was attenuated after exposure to cannabis was lagged.
The researchers credit the findings of other studies to a possible reverse causation mechanism due to self-medication with cannabis. They found no associated risk between cannabis use and progression of liver fibrosis or cirrhosis.
Hepatic encephalopathy and phytocannabinoids
Chronic liver disease can lead to hepatic encephalopathy, a decline in brain function. The liver’s most important role is to take contaminated blood from the gastrointestinal tract and detoxify it, along with metabolising drugs and other toxic materials that enter via the gastrointestinal tract. If its function becomes too heavily impaired, toxins begin to accumulate in the body, including in the brain.
There is not an overwhelming amount of data available about the endocannabinoid’s role in hepatic encephalopathy. It is nonetheless reliable and promising for further investigation of treatments.
In a 2006 study, researchers observed elevated levels of endogenous cannabinoid, 2-AG, in the brains of mice with fulminant hepatic failure. The team of researchers used this as a biomarker that the endocannabinoid system was responding to liver dysfunction. The mice were treated with exogenous 2-AG and another CB1 receptor antagonist, SR141716A and their neurological scores improved. Their scores improved again when treated with CB2 receptor agonist, HU308. The researchers concluded that modulation of the endocannabinoid system by exogenous cannabinoids, either as CB1 antagonists or CB2 agonists, shows potential for future treatments.
In another study, researchers reported that stimulation of AMPK (a cerebral enzyme and major intracellular energy sensor) is a response to liver failure. This enzyme is regulated by the endocannabinoid system. Administration of THC to hepatic encephalopathy induced mice augmented AMPK levels and restored normal brain function. This is because in hepatic failure (as discussed earlier in the article), the CB2 receptor is strongly stimulated and responsive.
There also exists a body of research relating to the endocannabinoid system’s role in hepatic vasodilation and other circulatory changes during cirrhosis. These matters are equally pertinent for the growing body of research surrounding the endocannabinoid system and its response during cirrhosis.
What we know and what we don’t know about cannabis and cirrhosis
The existing research shows a clear connection between the endocannabinoid system and liver cirrhosis. At the very least, research confirms that the endocannabinoid system acts like a recovery response team for a person with a degenerating liver. When the condition becomes severe, such as with liver cirrhosis or hepatic encephalopathy, the endocannabinoid system is a promising target for treatment.
However, when it comes to treatment with cannabis (and whether or not it’s actually a contributor to an already existing liver condition) remains somewhat controversial. High amounts of cannabis use likely will lead to more liver fibrosis in those with existing liver disease. Further investigation is needed to better understand the role of cannabis as a medicine in some forms of liver disease.
- Disclaimer:This article is not a substitute for professional medical advice, diagnosis, or treatment. Always consult with your doctor or other licensed medical professional. Do not delay seeking medical advice or disregard medical advice due to something you have read on this website.












I was diagnosed with hep c in 1987 was told I had it for a long time I had a blood transfusion in 1970 I have stage 4 cirrhosis am thinking of smoking pot I haven’t in 11 yrs and before 25 why do I want to start well to relax can’t drink since 1987 and ant take pain pills or to much meds I need something to relax am 70 yrs wiser
I had MT gallbladder removed because I had issues and now they telling me I have fatty liver cerrosis drank socially smoked weed from 17 to 30 yrs old or more and it is what it is God has plans for me just sucks to have it in the back of my mind all the time don’t drink don’t smoke 6 yrs sober THC or not
God knows I have Hepatitis B and C but when I smoke marijuana oooh I feel good and I don’t care God has got my back
Good afternoon Malcolmakes,
Thanks for your support,
I’m glad cannabis makes you feel better, it’s such a remarkable plant!
You might also enjoy our article on How Does Cannabis Affect Eating Disorders Such as Anorexia and Bulimia?
Thanks again, and have a great evening!
Mark
My brother was diagnosed in the later part of June with having Hepat cellular carcinoma, cirrhosis, and Hepatitis C. He also suffered with 2 hernias. He was hospitalized for 8 days and they sent him on his way with no hope. No surgery, no chemotherapy, no radiation. They gave him a large prescription for Oxycodeine. I immediately jumped into action as a friend of mine suggested to get him on RSO and CBDs. He has been consuming this for 2 months now and looks to be getting better. The medical community refuses to look into the possibilities of this as being the cure yet many people have become cancer free. He will need some new scans to know for sure but they will not perform any until they are damn well ready. They suck. If nothing else, this man will have a much better quality of life with out the Oxycodein they prescribed. That medicine is junk. He was very confused and could not even function. In the beginning, they removed 3 liters of fluid from his abdomen. He has not needed that procedure since using the RSO and CBDs. Fluid collection in the abdomen is common with cirrhosis and continues to come back even after having it removed. So if using this would cause cirrhosis, why isn’t my brother worse.
Hi I read your story with much interest as i have hepatocellular carcinoma, have had hep C and have cirrhosis,
Fortunately I do not have advanced stage Cirrhosis and have had 1 tumor successfully ablated with microwave and another treated with doxorubicin recently and due a scan in 5weeks time to reassess.
I have just learned that RSO can and has cured cancers and fortunately for us in NZ medicinal marijuana has just become legal and although it can be got on prescription it’s extremely expensive and its actually cheaper to get better quality illegally
I am about to start my first dose on Friday two days from now and being a former pot smoker from way back I’m excited
So thank you for your inspiring message and tell me how is your brother getting along these days as its been 4 years since your post here. looking forward so much to hearing back from you.
Hello, I know its a few days that maybe you are using it, but are you seeing any difference? Because I have my father with the same diagnosis, only that he is at Esld. Please if you can give any info
I agree with Miguel. What was the point of doing the study if they threw it off with alcohol? I also do not believe there is enough evidence. My opinion is that it’s unlikely to cause the body harm especially when we have marijuana receptors in our body. Marijuana is a natural cure.
I think it messed my liver up.. smoking weed.
They did not run the tests on human with JUST cannabis? Why did they always have alcohol as part of the equation? This research tells me nothing.
To John Flynn… Have you been tested for Hepatitis C ?? Ihave had hep c for 30 years before I was even diagnosed , My liver is now 100% useless to the point I had to have a stint straight through it . No cancer , yet . Judging by your age I assume you were in Vietnam , and I have heard from a lot of vets who got Hep C from all of the vacinations , especially the air injected type . It seem that a lot of blood was transfered between individuals . If that is the case with you , the VA should not only be responsible for your treetment but may be liable for a lot of different problems . They are hard to fight but there are a lot of attornys who specialize in VA problems .Most of them will take your case for for no charge .. I hope this may help in some way .Most important of all is to Fight Fight Fight and NEVER GIVE UP
I’d like to know if this was a controlled study.
As in they only smoked marijuana and did not drink any alcohol, take prescription drugs, aspirin. Or anything else that can severely damage the liver.
I was diagnosed with Cirrhosis of the liver, the doctor also mentioned liver cancer. I was told that I had 2 weeks to two months to live. That was December of 2012.
“Relevant info” My Mother died Jan 2 2012 I went into a self induced state of drunken decency. I was also percribed by doctors and abused by myself, Oxycontin for pain and Xanax for my depression. I was also a Marine stationed in camp LeJune where I was told that I more than likely digested some toxins from the water.
Cirrhosis: Initially my symptoms were extreme. Swelling, ( Ascites and Edema) they removed 14 jars full of black bile (Looked like Guinness ) I was jaundice. I suffered through Detoxification DT’s (Sorry about spelling). To date I haven’t seen a Doctor since I left the Hospital in 2012, almost 3 years ago I am 57, I am 6 ft and 245 lbs. I quit drinking and I have been avoiding any prescriptions drugs including Tylenol. I drink a lot of water. I am getting better, however, I have suffered mentally and have some dementia I suffer joint pain I believe Ascites, or could it just be just weight gain? and from Neuropathy. Thats a killer.
To my question: I cant afford Medical care. I’m hoping that the V.A. will help. I have a claim pending. Is there any advice besides “See a Doctor” you can offer. I’m a little frightened.
My best
Sincerely
John Flynn
Hey John hope everything is going well with you, my father is 60 years old n is suffering from chirossis n stage 2 liver cancer . Any advice ? Should he be on cannaboils? Thanks best to you..
14 minutes ago
Hello my mom went into a hepatic coma 2 yrs ago..for 10 days..she wasnt expected to survive..shes not a drinker never was …as she aged she developed. Chronic pain. with arthritis..after antiinflamatories etc. Her liver finally failed without Canadian Dr.s taking notice..apparently shed had this primary liver cirosis since my brothers birth when she was 33…but my dad was rcmp so we were transfered from small town to isolated small town with Dr.s that never even offered for her to be put on a transplant list! Now its too late…we adminerstered high doses of liquids of milk thistle..and it has kept her alive…the issue is this..of course dr.s took her off everything..told her suffer through the pain..or die..nice options right! So she started taking nips of alcohol at night just to ease the pain…this of couse is causing ammonia spikes…I want her to stop the boose and try cannabis for the pain and help her sleep…and Im looking for info on the least damaging method to the liver…I am assuming inhalation would be less likely to cause trouble as its not being digested..but Im not sure? Can anyone help me find information…or tell me thidr exp..I dont want to kill my mom..and I want to help her last bit of time here to be worth being here?
my mom almost died in the absolute worst way…for months I was taking her to the emerg for severe swelling…they sent us home…then one day coming home from picking up rx’s I got an anfry call from my brother asking if Id talked to my mom that morning..I said no..Im actually on my ay there now..why..he had called an ambulance he thought she had had a stroke…Id been with her the eve before…she seemed sleepy..but Id thought she was tired as she thought she had hurt her back..and was in bed…she was rushed to emerg where she got worse..no one was even testing her blood levels..I demanded a test..they didnt preform it for another 8 hours…now my mom was telling me she had just fed the horse over there some hay…and why did my daughter have blood on her neck? ( she didnt) knowone was listening to me…when I arrived the next morning…I spoke to her one last time before she slipped into a coma they expected her to die from….she would never even remember we were there…she was in a coma for 10 days…we did shifts around the clock..I found out they have a new iv drug that can scrub amonia levels from the blood in 12 hrs..its being fast tracked through the usa…any drug like this that has life saving benifits can be brought in with canada forms under these circumstances…it would have saved her yrs of rehab..she still cant walk unassisted…we began milk thistle extract liquid while she was in coma though her feed tube…then gave it to her 4 times daily while we did shifts….she went through a surgury to remove a blood clot from her ankle caused by the coma…then 2 bouts of c diff…we got her out as soon as we could…leaving her in hospital while recovering would have killed her as her imune system was gone..she was in total blood failure…we kept hopefull I kept researching….she went to hawaii last year…her twin grandaughters are now 6..they at least will remember her…my daughter is becoming an actress Im tring to get into production my screenplay…she has alot to see yet..and Im tring to do everything in my power to keep her here with us…I know high doses of lactulose help bind ammonia and remove it from the body…and liquid milk thistle is the only thing known to man to help regenerate liver cells..its a rx in germany..where genevas liver confrence is held where are the top minds are working on new techniques..like the new iv drug..that scrubs ammonia from the blood…she really needs that therapy…and its not available unless shes dieing…define dieing..shes dieing daily! I dont know if this is any help to any of you but Ill gladdly tell you our story..and what has helped us.Iam looking into cannibis as a pain killer that she can take that wont kill her quicker..and give her back quality of life.I did help my friend aunt..she began apparently behaving the same way…but because of knowing my moms symptoms she called me they adminersted lactulose before going to hospital… And fluids and lasic furosimide and got her onto milk thistle..they avoided a coma…and her liver levels continue to improve..which dr.s are saying is impossible.
0 Edit Reply
John I don’t know what state you are in,but you mentioned VA. Yor post is a year old and maybe you know this now. The A took on the task of curing Hep C with Harvoni. Turns out many baby boomer period Veterans, especially those that served in the 3rd ( San Diego command) and 7th Fleet (Yokosuka, Japan command). This has made the VA accept and treat many more cirrhosis patients and have come to give Veterans significantly better attention to liver disease.
Additionally the secretary, of the VA appointed by Trump, has approved an initiative to not deny benefits or take them away from Vets in a state where it is legalized and they and they are a cardholder. He believes Vets have given enough and if something relieves their pain and symptoms then they should not loose their benefits. CAVEATS: You must be enrolled in the state medical m,marijuana registry. The VA Doctors CANNOT prescribe Marijuana, but they can discuss with the Vet alternative treatments even if it Marijuana.
There is no reason to have someone with Non alcoholic Cirrhosis developed from Hep C becoming addicted to anti-anxiety drugs, opiods, etc. if THC or CBD helps them.
i smoke and will till i die it helps me to deal with dumasses who look down there nose and think there better cause they dont smoke give them a f ing cookie thank you
Just wanted to say when you get older you will be more concerned for your health. I recommend that you try to Vape when you can. I know you love a joint. Oh man I do too. But I have severe Emphysema and I so wish I could smoke a fatty
I guess I will try on my death bed
Linda, I had childhood emphysema which was horrific, and I still have asthma 60+ years down the road…
The single thing that shifted my overall lung health was when my 1st OMD prescribed Cordyceps as a single herb in addition to ‘Pe Min Kan Wan’, the Chinese Patent Medicine he recommended for chronic allergies. He cautioned me on the latter that “They took a long time to develop. They will take awhile to heal. Take 3-3x/day or up o 4-4x/day as symptoms require.” AMAZING results!
Within less than a week of starting the Cordyceps capsules (1-4x/day) I noticed I was using my albuterol inhaler less than before. Over time my regular use of it diminished by about 25%. Now it’s about half what it was in 1995 before I began ingesting Cordyceps regularly. Even better, it’s an adaptogen and kidney tonic so has helped in numerous other regards. In the Orient it is also used to treat Hepatitis. I think it’s helped my liver stay healthier in addition to lungs, kidneys, etc.
good luck reducing your symptoms!
If you’re going to call someone a dumb-ass then at least spell the word “dumb” correctly ffs
I think you may find this interesting..
http://www.ncbi.nlm.nih.gov/pubmed/23811492
Marijuana Smoking Does Not Accelerate Progression of Liver Disease in HIV-Hepatitis C Coinfection: A Longitudinal Cohort Analysis.