Post-traumatic stress disorder (PTSD) is a psychological condition that occurs in response to severe or protracted stress, such as experiencing warfare or interpersonal violence (which may be physical, emotional or sexual). Numerous PTSD sufferers self-medicate with cannabis, and several studies indicate potential benefit.
As the name suggests, post-traumatic stress disorder (PTSD) comes as a direct result of experiencing a traumatic event., Symptoms include flashbacks of the traumatic event, avoidance of associated triggers, anxiety, depression, anger and hyper vigilance.
Conventional therapy for PTSD mainly includes psychotherapy, with a focus on cognitive therapy, exposure therapy and eye movement desensitization and reprocessing (EDMR). Depending on the severity of symptoms, some PTSD sufferers are also prescribed anti-depressants and anti-anxiety medications.
Global prevalence of PTSD
The US National Comorbidity Survey Replication estimates the lifetime prevalence of PTSD in the USA to be 6.8%. Within this, the lifetime prevalence of PTSD among American men is 3.6%, and among women, 9.7%.
According to a 2019 study published in the European Journal of Psychotraumatology, it is estimated that around 354 million adults worldwide experience PTSD, with 117 million suffering from comorbid PTSD and major depression. These figures are the result of analyses of those affected by war between 1989 and 2015, and who were still alive in 2015. According to this meta-analysis, around 33% of PTSD sufferers will also be diagnosed with major depression.

Not every individual that experiences a traumatic event will go on to develop PTSD. One study determined that 17% of Iraq veterans would go on to develop PTSD, generalised anxiety disorder or depression. Another study estimates that around 25% of children exposed to trauma will go on to develop PTSD. Another concluded that monozygotic (identical) twins have a greater risk of developing PTSD after combat trauma if their twin also suffers from the disorder, pointing to a genetic predisposition.
PTSD and substance dependence
Research has demonstrated a high incidence of substance abuse among those with PTSD. In one study, women in particular showed higher rates of PTSD and substance abuse comorbidity — between 30% and 59%. For women in this category, PTSD is most commonly caused by repetitive childhood physical and/or sexual assault. For men, comorbidity rates are two to three times lower, and usually stem from combat or violence related trauma.
Another small-scale study including 91 participants attending a community based substance abuse program found that up to 52.8% of participants had some form of PTSD. While 37.4% were considered to be sufferers of PTSD, the remaining 15.4% were found to have “possible PTSD”.
Whether cannabis can be truly seen as a treatment for PTSD remains in question, as affected individuals may seek solace in such substances whether or not they are truly effective medications.
Although there has been significant research into substance use among those suffering from PTSD, studies relating to the effectiveness of cannabis as a treatment are relatively sparse. Up until relatively recently, the consensus among the medical community generally was that PTSD was a contributing factor in cannabis use disorders, and little investigation was undertaken into the brain mechanisms by which such disorders develop.
The role of the endocannabinoid system in PTSD
Understanding of the complexities of the endocannabinoid system has increased in recent years, and the role that it may have to play in regulating the symptoms of PTSD and similar disorders has come into focus. An article published in 2012 noted that stress-tolerant individuals exposed to acute stress in the form of a parabolic flight experiment demonstrated significantly increased endocannabinoid concentration in the plasma. Non-stress-tolerant individuals experienced no increase.
However, these individuals were healthy, and not suffering from any chronic stress condition. PTSD (and other chronic stress) sufferers, on the other hand, showed consistently elevated levels of endocannabinoid concentration compared with non-sufferers, even in ordinary, non-stressful situations. This implies that the endocannabinoid system plays a role in the stress response, but the exact mechanism is still unclear.
Interestingly, in another 2015 article published in Nature Reviews Neuroscience, researchers touched on the role of the endocannabinoid system in several aspects of fear-memory processing. The analysis suggests that “repeated re-exposure to a fear-related stimulus in the absence of the threat increasingly activates endocannabinoid signalling”. The researchers argue that this incessant endocannabinoid signalling may lead to extinction of the fear response.
This research shows a possible biological marker for diagnosing PTSD, which in most cases, is done through questionnaires. While the study itself does not specifically refer to PTSD, it refers to the psychological phenomenon underpinning PTSD: the repeated fear response in the absence of a threat.
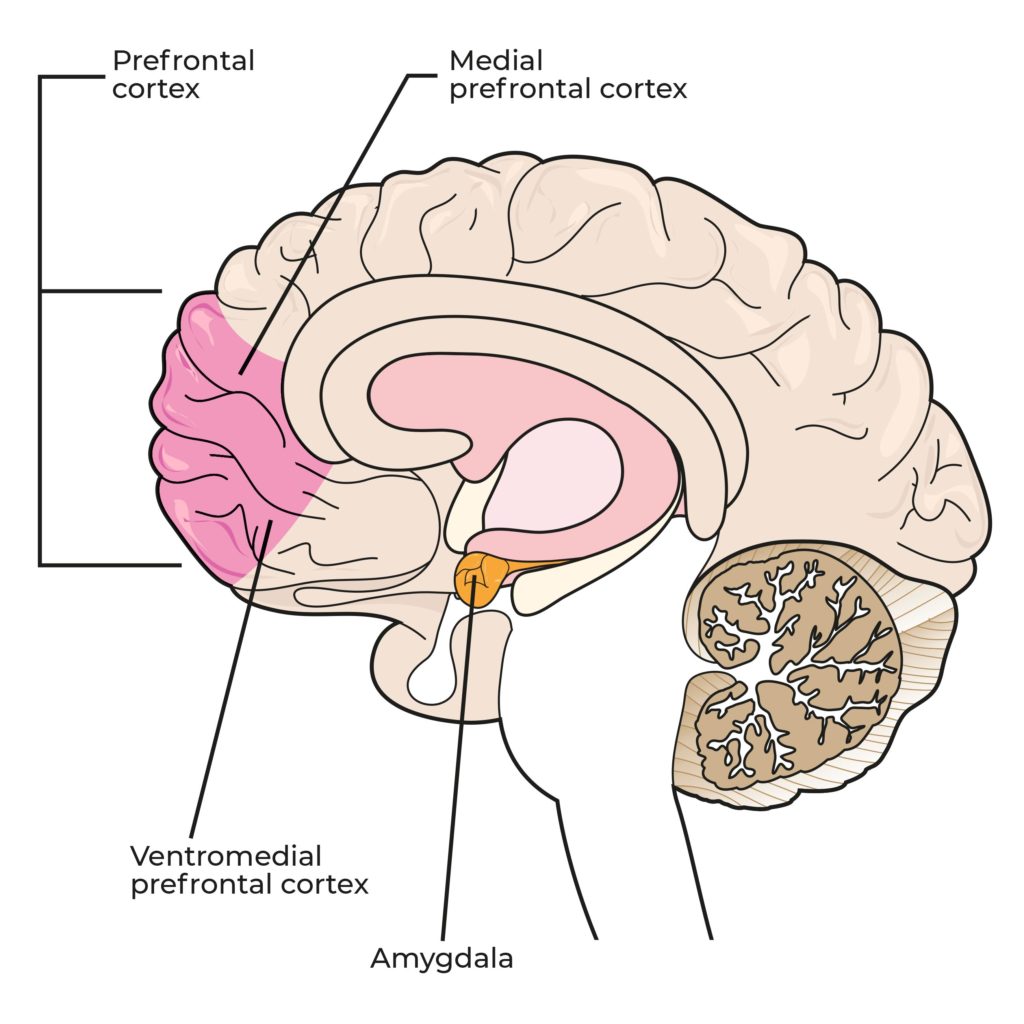
Genetic phenotype of CB receptors could increase predisposition to PTSD
Another 2012 study by Alexander Neumeister supports the findings of the Nature Reviews Neuroscience study mentioned above. The article describes the role of the CB1 receptor in the experience and memory of stressful events. Normal endocannabinoid signalling through the receptor assists in extinction of fear, and impaired signalling is associated with a failure to eradicate memories of trauma. This was also linked to chronic anxiety and depression (in animal subjects).
The article also noted that existing medications for PTSD have been implemented “opportunistically” when their benefits were discovered, and that such medications had usually been originally designed for other conditions. Often, such drugs are of limited effectiveness and may occasionally cause serious side-effects.
Overall, there is a common thread in academic literature that there is a link between endocannabinoid signalling, fear processing and the development of PTSD. While PTSD relies on a traumatic event to occur (without the trauma, the condition is not PTSD), there may be a genetic predisposition to the condition.
THC and Nabilone as possible treatment options
Neumeister concluded in his research that THC may provide temporary relief of PTSD symptoms, but long-term use could lead to impairment of CB1 receptor signalling. This could cause an increase in the severity of anxiety, irritability and sleep disturbance in PTSD sufferers.
A 2009 study also investigated the efficacy of a synthetic cannabinoid as an adjunctive treatment for PTSD. An adjunctive therapy is one that is prescribed in addition to a primary medication. In this case, the primary medications were antidepressants and hypnotics, and the synthetic cannabinoid used was Nabilone. This study found that 72% of patients experienced cessation or reduction in nightmares, improvement in sleep time and quality, and a reduction of daytime flashbacks.
Although the results of this study are promising, the small sample size of just 47 individuals means that further research must be done to determine the effectiveness of nabilone. As interest in use of cannabinoids as treatment for PTSD is increasing so rapidly, we are likely to see the results of further research in the future.
Other ways that cannabis can alleviate symptoms of PTSD
As current understanding of PTSD goes, there is no pharmacological way to cure PTSD because of the nature of the condition. It is acquired from a trauma, and there is no known pharmacological treatment to “undo” a trauma. This is why treatment typically includes managing symptoms of anxiety, insomnia, depression and flashbacks. While cannabis may not technically cure, or even contribute to a cure for PTSD, it has properties that may help with symptoms.
1. Cannabis may have anxiolytic effects
While the anxiolytic effects of THC have been questioned many times over the years, there is a general consensus among scientific academics that CBD especially has anxiolytic effects. For certain individuals, THC is also able to reduce anxiety symptoms.
One of the major symptoms of PTSD is anxiety, and it is often one of the symptoms that can be managed with medication. A 2011 study on mice concluded that overexpression of CB2-receptors reduced anxiety-like behaviours and caused an increase in gamma-aminobutyric acid (GABA) in the hippocampus and hypothalamus.
In another study (in vivo, on humans), individuals with PTSD were found to have reduced levels of endogenous cannabinoid, anandamide. Consumption of CBD is thought to increase serum levels of anandamide by inhibiting FAAH, the enzyme responsible for anandamide degradation. This is one mechanism of action by which CBD is thought to have anxiolytic and anti-depressant effects.
2. Cannabis is neuroprotective
The neuroscientific understanding of PTSD is still in elementary stages, but scientists are constantly looking for reliable biomarkers for the condition. Naturally, and as mentioned before, endocannabinoid signalling shows promising potential. In this 2018 research, Graziano Pinna discusses the role of neurotransmitters in cases of PTSD, and the possibility of using neurology as a form of PTSD treatment.
Essentially, Pinna suggests that certain chemical processes in the brain that contribute to neuroprotection may play a role in the regulation of cognitive processes and emotional behaviour. While we are only beginning to understand how neurology affects human behaviour and emotion, it is something intuitive to the field of study.
Phytocannabinoids THC and CBD have demonstrated neuroprotective effects countless times in academic research, including the ability to stimulate neurogenesis. While it is not clear exactly how neuroprotection can relieve symptoms of PTSD, a connection has been established.
3. Cannabis may help treat insomnia and relieve nightmares
As mentioned earlier in this article, many PTSD sufferers experience treatment-resistant nightmares. In the study referred to earlier, patients experiencing nightmares demonstrated a positive response to Nabilone, a synthetic cannabinoid.
How THC and CBD may reduce nightmares has not been established, but the general understanding is that THC decreases sleep latency. By doing so, it may help PTSD suffers to achieve sleep and to remain in a more-or-less dreamless slumber. By decreasing sleep latency, REM sleep is either bypassed or shortened too much to induce nightmares.
There is still a lot to understand about PTSD as a condition, and even more about how cannabis can be used as a treatment. There is controversy surrounding cannabis as a treatment for PTSD because it is not a treatment per se, but an adjunctive therapy to reduce symptoms. It poses the potential for abuse or addiction, especially because PTSD sufferers are more likely to develop substance abuse disorders.
However, despite the ongoing controversy surrounding the effectiveness of medical cannabis as a treatment for PTSD, the Medical Cannabis Advisory Board recommends keeping PTSD on the list of qualifiers allowing prospective cannabis users to take prescriptions.
- Disclaimer:This article is not a substitute for professional medical advice, diagnosis, or treatment. Always consult with your doctor or other licensed medical professional. Do not delay seeking medical advice or disregard medical advice due to something you have read on this website.












The article states that THC alone (or synthetic THC Nabilone) only provides temporary relief due to build up blocking the CB1 receptor. However, if you use whole plant products, the other cannabinoids, especially CBD, naturally counteract this effect and balance out. Whole plant use can provide sustained, long-term relief. The bottom line is that the endocannabinoid system regulates and balances out many bodily systems, and you need this plant to keep it healthy and functioning properly.
i am 50 a survivor of child sexual assault adult s assault dv and in 2013 my daughter age 26 and g daughter 6 died in a car crash. i have 2 boys 16 and 11 years i am single parent and i smoke pot to stay sane enough not to quit and i do not drink alcohol
Ruderalis Indica works for me as a stress reducer and sleep inducer. Easy to grow and cheap.
I have a mental illness and hash is bifar the best treetment the pills they give me have such bad side effects they make me worse but ive had to stop cose i cant afford it any more
Seshata the article you have written about PTSD it’s really very informative, surely it will help sufferings to know about PTSD. Domestic violence, substance abuse and unemployment, suggested to some military doctors, combat commanders and researchers that conventional treatments aren’t always enough. We need something unique & spiritual like Trivedi Effect to prevent PTSD.
i love to this product man
I’ve had extream PTSD for 10 years and the only thing that help me with angsiety, irritability, sleep and anger is bush pot. My wife even encourages me. After a smoke I, my personality changes back to normal – the person I used to be before the accident. I’m a mature professional (No I don’t smoke or condone smoking weed at work) adult and pot does defiantly helps me and my family.
The only thing holding this back,, is the do gooders. Who thing they know everything cause they have a degree or what not. But really (from experience) they don’t know much at all. People are spose to help each other…whoops that was wounder land. No people just like seeing people suffer to make them selves feel great about them selfs, (YES ITS MOST OF Us 99.98%) And if people of thoughs types, only build them selfs up over disadvantage people. The human race is defiantly backwards……………………when you think about it,,, this has been mostly humans way of exsistance. So much for getting better with age. Or we could just over populate the world. That way no ONE really,,,,,really,,,truly gives a shit…..!
Posttraumatic stress disorder is classified as an anxiety disorder; the characteristic symptoms are not present before exposure to the violently traumatic event. Typically the individual with PTSD persistently avoids all thoughts, emotions and discussion of the stressor event and may experience amnesia for it. However, the event is commonly relived by the individual through intrusive, recurrent recollections, flashbacks and nightmares.^”
intresting info & good work Seshata please keep me posted with anything more you descover on your journey
regards
Richard