Cannabis arteritis is an extremely rare and under-studied medical condition that causes blood clotting and thrombosis in peripheral limbs. Until now, modern science has not confirmed it as a true medical condition. We explore the research as we try to understand the link between cannabis and thrombosis.
First described in 1960, the putative condition, cannabis arteritis, is thought to have affected approximately sixty individuals since then. The condition is said to affect long-term, heavy cannabis smokers by causing inflammation of the walls of the peripheral arteries. In extreme cases, the condition has led to amputation of the affected limbs.
Despite evidence suggesting that the condition is related to smoking tobacco, some believe that the effect of cannabis plays a unique role. In 2001, a French study presented ten new cases, all of which had occurred in men of a median age of 23.7 years. These individuals all experienced necrosis of the hands or feet after undergoing subacute distal ischemia, or moderately sudden loss of blood flow to a limb. Despite treatment, four patients ultimately required amputations.

Link between thrombosis and tobacco consumption
Due to the known vasoconstrictor effect of cannabis, the researchers concluded that the patients’ regular consumption played a key role in their condition. These men were all moderate tobacco smokers, so it is impossible to accurately assess the degree to which cannabis use was responsible for blood clotting or thrombosis.
However, although most researchers of cannabis arteritis have only studied patients who also smoke tobacco, another French study from 2011 documented the case of a 36-year-old woman with arteritis. She experienced prolonged exposure to cannabis but not to tobacco. In this case, quitting cannabis use caused symptoms to rapidly improve.
Yet another French study described the case of a 36-year-old man with no history of tobacco use. He developed necrotic lesions on the toes, purportedly due to his long-term use of cannabis. After failing to curtail his consumption, the patient developed ischemia of the left leg, requiring amputation.
Finally, the most recent case study took place in 2017. The man in question was 35 years old and smoked 20 cigarettes a day in conjunction with cannabis. He presented with symptoms of necrotic plaque and was finally diagnosed with Buerger’s disease. Researchers concluded that cannabis is at least a cofactor in this particular case, and that the condition is increasingly prevalent in cannabis users regardless of tobacco use.
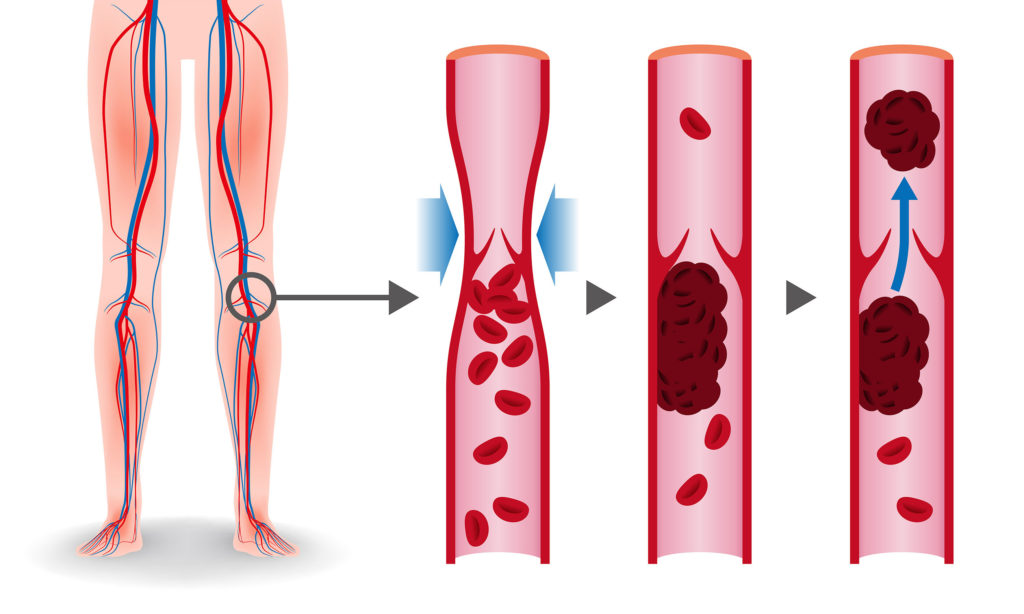
Cannabis and vasoconstriction
Cannabis has long been thought to cause vasoconstriction, in which the walls of a blood vessel (particularly the arteries and arterioles) contract, narrowing the channel and restricting blood flow along it. For over-65’s, one study concluded that the risk of heart attack in the hour after cannabis consumption was five times higher. Even in younger individuals, several cases of heart attack and ischemic stroke (caused by sudden loss of blood flow to the brain) have been attributed to cannabis use.
In a French study of 48 young adults that had experienced ischemic stroke, 21% were found to exhibit multifocal intracranial stenosis, or multiple narrowings within the cranial arteries. Of the 21%, all were cannabis users, and although not all displayed symptoms, the majority were affected. Of all the demonstrated causes, which included cardioembolism and artherosclerosis, this pattern of stenosis was most common. Researchers therefore concluded that cannabis use could be a key contributor to ischemic stroke in young adults.
Problems with establishing causal links
While there may indeed be a link between cannabis use and vasoconstriction, the sample size in this particular study was too small to draw valid conclusions on the relationship with ischemic stroke. Furthermore, most consumers of cannabis in France also consume tobacco, and tobacco is also known to be a vasoconstrictor.
Therefore, further research must be done before assuming a causal link. Indeed, the vast majority of research into cannabis arteritis has been done in France, where laws are strict and political opinion mostly disapproving, and the possibility of bias seems very high.
There are many great similarities between cannabis arteritis, thromboangiitis obliterans (Buerger’s disease) and the progressive blood clotting in the peripheral arteries associated with tobacco use. These similarities lead many to believe that the conditions are not in fact separate, but that the effect of cannabis is synergistic at most. Confirmed cases of cannabis arteritis that are not associated with tobacco use are insufficient to establish a true relationship.
Could contaminants be to blame?
Yet another possibility is that the high incidence of this condition in France is due to a contaminant in widespread use, rather than cannabis itself.
In fact, arsenic has been proposed as a possible contaminant. This is because in high-phosphorus soils, cannabis has been shown to exhibit higher uptake through the root system. Plus, water supplies polluted by arsenic have been implicated in cases of “black-foot” necrosis. The fact that the majority of cannabis consumed in France is hashish, which is often mixed with very harmful additives, strengthens the possibility that contaminants play a part in cannabis arteritis.
Complex relationship between cardiovascular and endocannabinoid system
Contaminants do not propose the only complexity in this matter. There is evidence that contradicts many of the underlying principles of cannabis arteritis. Several studies have shown that THC, anandamide and abnormal CBD cause vasodilation rather than vasoconstriction, by causing the smooth muscle of the artery walls to relax.

Atypical cannabinoids may also induce vasodilation. Vasodilators assist in reducing blood pressure and increasing the flow of blood to the peripheral tissues. Certain cannabinoids often also exhibit significant anti-inflammatory effects.
In fact, there is evidence to suggest that certain cannabinoids may have anticoagulant (anti-blood clotting) properties, This came to light after a study conducted at the University of Dallas in 2017, where researchers found that cannabis may reduce blood pressure and enhance blood and oxygen flow. This would usually imply that the risk of thrombosis-like diseases would be reduced.
The highly complex interactions between the endocannabinoid and cardiovascular systems require intensive research before firm conclusions can be drawn. Cannabinoids may differ in the degree to which they affect vascular function according to dosage, as well as the concentration in which they are present. A cannabinoid may also exert a vasoconstrictive or blood clotting effect in certain parts of the body and a neutral or vasodilatory effect in others. For example, it is thought that in rats, THC causes a vasoconstrictive effect in the renal arteries and a vasodilatory effect in the hindquarters.
While there is some evidence linking the effect of certain cannabinoids with vasoconstriction of the arteries, the status of cannabis arteritis as a condition in its own right is highly questionable. Further research may establish a definite link, but as it stands, there are not enough patients who have used cannabis exclusively (without tobacco).
For that reason, research into the matter is difficult and the results are compromised. Until further research presents itself in the absence of tobacco use, our understanding of the condition is limited.
- Disclaimer:This article is not a substitute for professional medical advice, diagnosis, or treatment. Always consult with your doctor or other licensed medical professional. Do not delay seeking medical advice or disregard medical advice due to something you have read on this website.











I have blood clots (P.E ) in my lungs Dr. Said I have a lot is it bad to smoke a joint here n there, will I die. I mean I’ve smoked for 25 yrs plus. An now I fund myself more frustrated n short temper 🙃 but if I hit a joint or 2 . I feel better . Plus I got this after covid diagnosis. How bad is it.
i’ve had portal vein thrombosis due to an infection on my bellybutton as a baby, and have never smoked weed or anything, but if i were to take an edible would it have the same effects as smoking?
Hey Mattie,
Thanks for your question!
The effects from consuming an edible can be quite different to smoking a joint. Edibles tend to focus more on physical effects that can result in a full-blown “couch-lock”. Another major difference lies in the onset and duration of the high. It can several hours for a brownie to kick in and the effect will last much longer than the effects of smoking or vaping.
Please check out the following articles on our blog which I think you may find of use. How Do Edibles Affect You? Edibles High Explained, How Does Cannabis Affect the Digestive System? and What is the endocannabinoid system and how does it work? A beginner’s guide
Thanks again, and I hope you continue to enjoy the blog!
With best wishes,
Mark
No it’s more intensified and you don’t need very much especially if you have never amen them before be careful don’t exceed 10mg THC of the edible because it won’t hit you right away it takes up to 2 hours to get most of the affect to start working and it keeps getting stronger and stronger as time goes by just sit back and relax and don’t be stupid like so many other people who keep eating more and more because they didn’t feel it coming on right away and by the time they’ve cosnsumed about 100 mg of THC it’s too late they either have a really bad trip or some people end up in hospital with something wrong or a stroke or Heart Attack So yes it can be dangerous also but if you do right for Chronic Pain don’t consume more than 10 MG at a time
The problem is to mix with cigarettes’ its totally dangerous
Can you smoke a bowl a day while having a blood clot in your lower calf muscle. While taking blood thinners.
Hi Sherri,
Thank you for your comment. We are sorry to hear about your situation. As Sensi Seeds is not a medical agency or practitioner, we cannot give any kind of medical advice other than to consult your registered healthcare professional.
You may also find it helpful to contact a support group for medicinal cannabis patients. In the UK there is the United Patients Alliance, and throughout much of the rest of the world there is NORML, who should be able to put you in touch with a group in your area (search United Patients Alliance or NORML followed by your area name).
With best wishes,
Scarlet
i smoke hash, the settlement that covers the leaves of marijuana leaves. heat it a bit befopre mixing it with a wills cigg. and smoke it in a chillum/pipe. what are the effects of the charas/hash on blood, can it confuse the nervous system or the brain from destroying platelets?
Hi Bishop,
I’m afraid I am unable to answer this question as it’s outside of our area of expertise. Sometimes our other readers will be able to offer their opinions though. Sorry I can’t help you further, and I hope you continue to enjoy the blog.
With best wishes,
Scarlet
The study on rats reveals both a vasoconstriction in the kidneys as well as dilatation in the quarters suggestive that even if it is used for vaso relaxation of the arteries, it may not be an exclusive response desired in the management of a medical condition but that there is likely a vasoconstriction response in some other part of the body creating a condition of potential harm. Plus it is addictive and impairs brain function.
I smoke weed without tobacco, I also have dvt caused by spiked hash. I have trouble with my lungs as clots have lodged there, for awhile I had a gf who smoked joints with tobacco, If I took a hit I felt really bad immediately but if I smoked a clean pipe after I felt better again.
I am 80 and have smoked cannabis for arthritis pain since it was legalized in California. In February I developed blood clots in my leg, that were removed by surgery. My doctor thought it was caused by COVID but I tested negative. I have never smoked tobacco.
Good afternoon Barbara,
Thank you so much for sharing your experiences!
It is definitely my hope that at the very least, this article can serve as a kind of online gathering point for others so that they can compare experiences and possible solutions, and not feel so alone!
Thanks again, and I hope you continue to enjoy the blog.
With best wishes,
Mark
I also have slot of blood clots in my leg and they are very painful why did they do surgery on yours did they remove the blood clots I Pray you are out Of Pain God Bless You
Hi
I am 47, have been eating a cannibus biscuit once a week for the last three years. Two years ago I developed a blood clot in my left leg. I have never smoked, i was going to gym three times a week and was very fit.
I stayed in hospital for a week having tests to find the cause but nothing could be found. I stayed on warfarin for six months which cleared the clots. It’s been two years but I feel that I am slightly out of breath again, I have been to my doctor and I have started warfarin again as a precaution. I have now decided to stop the once a week edible as I believe that this could be causing the clots. I have been searching the net to find out if there is any connection between marijuana intake and clots. Any info will be welcome.
I jus found out i got blood clot in my leg.. gotta get surgery to remove it.. how long was the surgery and healing process
In the same rat study thats showed vasoconstriction also showed vasorelaxation in pre constricted arteries. Most likely the irratation is from the smoke since dabs are mych syronger and not associatdd with cardia events