Epilepsy refers to a group of conditions characterised by recurrent seizures, which may be convulsive or non-convulsive. Cannabis and cannabis-based therapies have been shown to have beneficial effects on several types of epilepsy, through a variety of biological mechanisms.
Around 60% of all epileptic seizures are convulsive, which means that they are characterised by rapid, involuntary contractions of the muscles that can cause the entire body to shake or jerk uncontrollably. The most common type is the tonic-clonic seizure, which involves a short period of contraction of the limbs followed by their extension, and uncontrollable shaking. A period of unconsciousness can occur before the person turns to normality.
Both convulsive and non-convulsive epileptic seizures are caused by excessive activity in the neurons of the brain; if severe and prolonged, seizures can result in damage to brain tissue, particularly in young children, when the brain is still developing.
Dravet syndrome is one type of severe childhood-onset epilepsy that can cause neurological impairment. It is one of the rarer forms of epilepsy, and patients with Dravet Syndrome face a 15-20% mortality rate. However, there are many variations of epilepsy, and while Dravet Syndrome is an example of the most severe, there are also forms of epilepsy that are mild.
Because of prohibition during the 1970s, cannabis fell off the radar as a medicinal substance until recently. The recreational aspect of cannabis took over public opinion, and despite knowing that cannabis has some remedial properties, it was prohibited for medical use. Now, old research is resurfacing, especially in the case of epilepsy, opening new avenues of medical cannabis as a valid line of treatment.
1. Anticonvulsant benefits of cannabis for epilepsy
The anticonvulsant properties of cannabis have been known to humans for centuries, if not millennia. Cannabinoids were tested for their anticonvulsant properties by researchers as early as 1947.
An early study conducted at the University of Sydney in 1974 demonstrated that delta-9-THC given in high doses had an anticonvulsant effect on mice that were administered chemical and electrical shocks as a means to induce seizures. It was noted that CBD increased the anticonvulsant effect of delta-9-THC, although the researchers did not find that CBD was effective in its own right.
Since then, various studies have found that CBD does, in fact, possess remarkable anticonvulsant properties in its own right, as well as potentiating the effects of delta-9-THC. A 2001 study demonstrated that delta-9-THC and the synthetic delta-9-THC analogue WIN 55,212-2 exerted their effect by agonising the CB1-receptors. CBD exerts its effects via a different means, as it does not agonise the CB1-receptor but instead acts as a weak antagonist.

Due to its effect on the CB1-receptors of the central nervous system, delta-9-THC can actually cause convulsions in rare cases, while CBD does not appear to have this side-effect due to its independent mechanism of action.
The precise mechanism utilised by CBD when working to control convulsions has still not been established, but it is proving highly effective in treating various types of epilepsy including Dravet syndrome in young children, and has gained ground rapidly as a potential treatment due to its lack of psychoactivity.
2. Neuroprotective benefits of cannabis for epilepsy
As research into the endocannabinoid system advances, it is becoming clear that it plays an important role in regulating the duration and frequency of seizures. In fact, there is an entire school of thought that suggests epilepsy is actually caused by a dysfunction of the endocannabinoid system (a condition speculatively known as clinical endocannabinoid deficiency), which could arise due to brain injury, infection or genetic predisposition. This school of thought was founded by cannabis researcher and PhD, Ethan Russo and includes other neurological conditions such as Parkinson’s, Multiple Sclerosis and Dravet Syndrome.
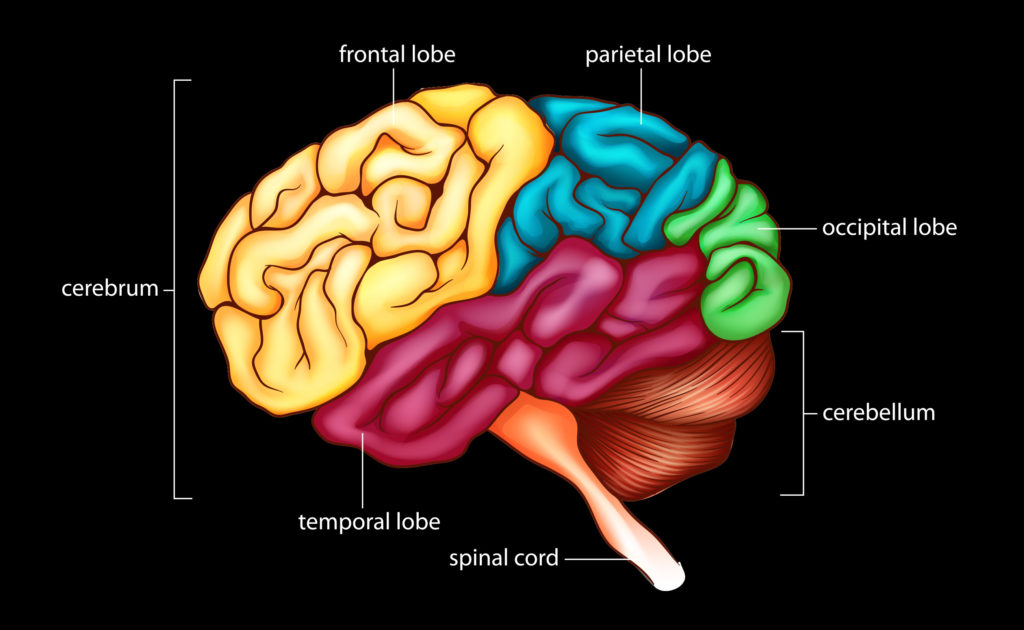
In 2008, a study published in Nature indicated that patients suffering from temporal lobe epilepsy appeared to have dysfunctional endocannabinoid systems. As the name suggests, temporal lobe epilepsy affects the temporal lobe of the brain, and typically produces non-convulsive seizures that involve some degree of sensory (visual, auditory, olfactory or even gustatory) disturbance—although it may also produce tonic-clonic seizures in severe cases.
The common cause of convulsive and non-convulsive seizures is excessive excitation of the neurons in the brain, with the affected region of the brain varying according to the type of epilepsy. In healthy patients, the endogenous cannabinoids anandamide and 2-AG are thought to play a fundamental role in regulating the level of neuronal excitation and thereby reducing the likelihood that a seizure is triggered.
Thus, in patients who possess a dysfunctional endocannabinoid system, cannabis and cannabis-based therapies may target the cause of epilepsy and provide a neuroprotective effect that reduces the severity and frequency of symptoms.
3. Protection against status epilepticus
In extremely severe cases of epilepsy, a condition known as status epilepticus may occur. Status epilepticus may involve continuous seizures, which either last for a duration of over 30 minutes each, or occur at a frequency of more than one seizure per five minutes with no return to full consciousness in between.
If the patient is not provided immediate medical care during an episode of status epilepticus, the prolonged loss of normal brain function may result in brain damage or even death. If adequate medical care is provided, epileptic patients usually survive an episode of status epilepticus without major complications.

However, there is evidence that cannabinoids—specifically CB1-receptor agonists like anandamide, delta-9-THC, and the synthetic analogue WIN 55,212-2—may provide stronger protection against status epilepticus. In a 2006 study published in the Journal of Pharmacology, WIN 55,212-2 demonstrated the ability to totally suppress all seizure activity, including the prolonged episodes associated with status epilepticus.
The study also noted that WIN 55,212-2 significantly outperformed phenytoin and phenobarbital in suppressing status epilepticus.
From this and various related studies conducted over the last decade or so, it has been well-established that agonists of the CB1-receptors are fundamentally important to terminating seizures and preventing the onset of status epilepticus. The research also supports that there is a very strong correlation between the endocannabinoid system and the neuronal excitation that leads to status epilepticus.
For example, a 2007 paper noted that if epileptic neurons were administered CB1-receptor antagonists, it would cause continuous epileptic activity as seen in patients with status epilepticus. If then treated with CB1-receptor agonists, the excessive activity would stop. Conversely, when non-epileptic neurons were treated with CB1-receptor antagonists, the excessive activity resembling status epilepticus did not occur.
The $1 million grant from GW Pharmaceuticals for cannabis-epilepsy research
Using cannabis as a form of treatment for epilepsy has been controversial in the past, especially in cases of epilepsy that affect children. However, in the last decades, scientists have taken to researching this controversy to better understand cannabis’ medical application in the case of epilepsy. GW Pharmaceuticals’ $1 million grant to Readings University is one such example.
In Readings University’s research, three compounds were identified as having potential to be used for therapeutic control of seizures. Cannabidiol (CBD), ∆9-tetrahydrocannabivarin (THV) and GWP42006 significantly reduced the number and severity of seizures in rats. Ultimately, researchers are using cannabis to search for compounds that may completely abolish seizures altogether.
Charlotte’s Web and the advent of cannabis for paediatric epilepsy
One of the first human trials on the effects of cannabis for epilepsy patients took place in the 1980s, but was not followed up on until the last decade. Essentially, cannabis was removed from any repertoire as a potential treatment for epilepsy, and in fact, it was frowned upon if it was ever used in this manner. On top of this, there is controversy in applying principles of medical cannabis on a paediatric patient.
Then, in 2009, the Stanley Brothers began to produce a high-CBD strain called Charlotte’s Web. It was created with the specific purpose of treating a paediatric epilepsy patient whose name is Charlotte. Shortly after she was born, she began experiencing frequent and severe seizures. She was diagnosed with Dravet Syndrome. As soon as Charlotte started taking the 30:1 CBD:THC strain, her seizures reduced in severity and frequency almost instantly.
Josh Stanley, one of the creators of Charlotte’s Web, tells CNN:
“The biggest misconception about treating a child, like little Charlotte is most people think that we’re getting her high, most people think she’s getting stoned”
This is one of the biggest hurdles that families and researchers face in the pursuit of understanding cannabis and its medical application for epilepsy. As it stands, the effect of cannabis on epilepsy is one of the most well-researched avenues of medical cannabis. As the research continues, cannabis is increasingly recognized and prescribed as a medicine for certain types of epilepsy, particularly those characterised by seizures.
- Disclaimer:This article is not a substitute for professional medical advice, diagnosis, or treatment. Always consult with your doctor or other licensed medical professional. Do not delay seeking medical advice or disregard medical advice due to something you have read on this website.












ONE HAS FOUND THAT THE PROPRTIONATE AMOUNT OF CANABIS AIDS NOT ONLY EPILEPSY BUT A NUMBER OF OTHER AILMENTS SUCH AS ;CANCER DEMENTIA, HEART AND RESPITORY CONDITIONS AS WELL AS HELPING ONE FOCUS
Hello
I have epilepsy but only when I don’t get enough sleep or really stressed.
All the tests in the world and all the medication cannot help so I was wondering if hemp seeds would help me. I am not a good sleeper and don’t want to take sleeping pills if I can help it.
What do you suggest.
Thanks
Joan
Hi Joan,
Thank you for your comment. We are sorry to hear about your situation. As Sensi Seeds is not a medical agency or practitioner, we cannot give any kind of medical advice other than to consult your registered healthcare professional. This article about the potential benefits of medicinal cannabis might be useful for you to show your healthcare provider if they are not familiar with it.
You may also find it helpful to contact a support group for medicinal cannabis patients. In the UK there is the United Patients Alliance, and throughout much of the rest of the world there is NORML, who should be able to put you in touch with a group in your area (search United Patients Alliance or NORML followed by your area name).
These are our pages on medicinal cannabis and medicinal cannabis strains, which you might also find interesting.
With best wishes,
Scarlet
This is a very nice article. Cbd is truly the next best thing in medical advancement. Why is it very popular? This is primarily because of it’s health benefits and effectiveness it can offer. I’ve watch a lot of video about how CBD works it’s magic in a snap. Marijuana strains can give you different effect.
I’m looking for a strain that promote sleeping (high in CBD). What do you recommend? How do I get seeds that I can grow it myself?
Sincerely,
Sam
Hi Sam,
Strains that encourage physical relaxation and sleepiness are mostly indicas. This page on choosing a medicinal cannabis strain will hopefully be useful to you, and depending on where you live, we may be able to send seeds to you!
With best wishes,
Scarlet
Been hit with temple lobe epilepsy when 22 . had to give up work last year because seizure’s started to get a lot worse 34 now. Am on 3 different types of medications epilim clobazam and sertralin . lived in newcastle for over 5 years were always had a good supply of good clean cannabis my seizures had completely dissapered but since a move back to London and try to sette back into workwork and not having a regular supply of cannabis they have never in my life been this bad lots of focal and some grand mal seizures. I no for a fact now cannabis is the answer in controlling my seizures. I have tempole lobe epilepsy there are lots of types of epilepsy but cannabis works well for me this type epilepsy the chemical compounds in cannabis have worked well for me. But cannabis that people buy on the streets now is full of crap its not clean and is causing more problems for the NHS that’s why they would legaliz it for medical use . Thanks for reading and good luck
Hi everyone! I am 47 and I have epilepsy. I got it when I was 22. I have been taking Dilantin since I was diagnosed. Which is 25 years now. I want more than anything to be off this medication and have a healthier way to control this ..Who agrees and understand me?
hi i have had tmporal lobe epilepsy since in my teens although only diagnosed in my 30’s. it was difficult living with this whilst never being told what it was. i always had an affinity with smoking pot and always had more seizures when it was unavailable or i was just having a break. im in my 50s now and not had a seizure for over 10 yers but sometimes i do feel an ‘aura’ but if i can remove myself from triggers i seem to be able to avoid going into a seizure. it is scary in some social and work environments wth triggers everywhere and avoiding being overtired. even just being a passenger in a car at night, bright and noisy places etc are difficult. i tend to isolate socially because of this. i am now about to stop using as i am scared to be arrested for having on me when i have to go and get. also, it is making me a criminal to use the medicine that works for me and keeps me seizure free. good luck with your ‘eppiness’
I agree and understand, Maria! I was diagnosed at 47, only a year ago, with temporal lobe epilepsy. The side effects of all the standard medications are concerning. I have been watching a lot of documentaries and reading a lot about CBD oil and I am hoping to find some good, reliable information. Right now I am searching for consistent dosing information but can’t find enough to calm my fears. I hate these standard medications, though, and I am ready to be off them as soon as possible. I hope you find the answers you are looking for.
Well I like what I see. I just have a concern for one of my family members. She is 10 and having very bad seizures. The medicine they have her on isn’t helping they’ve increased her amount to the max. She is on 4 different medicines. She can go to school anymore. Her seizures are lasting around 7-10 minutes everytime. She as around 4 a day. She also has a rare heart condition called brugada disease. Do you have any recommendations.
Hello Brittany,
Thank you for your comment. We are sorry to hear about your relative. As Sensi Seeds is not a licensed medical practitioner, we cannot give medical advice, and must recommend that you consult your doctor or other registered healthcare professional for all medical matters. When you do so, you might find this article which was written specifically for professionals who might not have researched cannabis as a medicine. Depending on what country you are in, you may be able to order our CBD Oil which is sold as a food supplement and has been known to have relaxing properties but I cannot recommend its use as a medicine or make any claims about if it would help with TS or not.
With best wishes,
Scarlet
Hi Brittany,
I would strongly recommend trying cbd oil/paste – It has worked for my Temporal Lobe Epilepsy and has enabled me to reduce my prescribed medication, all of which caused large amounts of terrible side-effects. I have gone from at least a seizure a day to one every three months and they are much less severe.
All my love to you and your daughter.
Good luck and stay strong.
Leo
Hi Leo, Could you please tell me how much and how you took the CBD oil for your temporal lobe epilepsy? And what kind/form you took etc. This is all new to me and I’m trying to find out how it can be best taken. How long do you take it for? Is it for a short amount of time or do you take it for the rest of your life? Specifics would be so helpful do me! Thanks in advance!
Cynthia
It started at 13 or so. My dad already with the condition. They put me on tergretol like dad and off we go.. I found mary-Jane a yr or 2 later and it seem to make the seizure’s turn to moments of deja-vu more than not..2012 I had a seizure driving and police took my license. seeing neurologist again,3 different meds still trying to get it right but no luck.. Pot helps 100% wen available, I quit for 6-12mths and it got alot more severe and frequent so I’ve been smoking since with heaps less problems but not legal in west Australia..plzzz make it legal
was 11 years old when placed on Phenobarbital, along with Dilantin for Temporal Lobe Epilepsy. Decades later, opponents of cannabis often state that cannabis’s euphoric effects are the reason they object to it.
Obviously not one of those individuals grew up on Phenobarbital,Mysoline(synthetic opium) , Tegretol, and all of the other AED’s I have tried throughout my treatment. Currently on Felbamate/Felbatol for intractable multi focal seizures.
Cannabis treatment for seizures should not be decided by those that have not experienced an anti seizure med. If they were so concerned about the “high effects” , then where were those people when I was seeing double, trying to stay awake and learn in elementary school, find my balance, etc., while being prescribed barbiturates as a child.
Signed,
Legally High for Years
Same! Mine is due to a traumatic brain injury at birth. I even had my entire right lobe removed 30 years ago. The seizures came back. I’m on 8 pills a day and still have seizures in my sleep.
Nice informative article. I have a friend whose daughter has epilepsy. We are waiting for Florida to legalize so she can get on a marijuana treatment plan. They legalized Charlotte’s Web as of January 1st but no one can get access to it yet. Florida is so backwards. We have thousands of other patients that can benefit from medical marijuana. We’ve been advocating and praying they legalize it SOON for all illnesses. I know how much it can benefit millions of people, not only people with epilepsy. I have a neuromuscular disease and edibles control my pain to allow me to live a better quality of life.
I have suffered with seizures for over 40 years now and still the Medical Profession have failed to find a drug that will control the seizures. At the moment I take both Phenytoin Sulphate and Phenobarbital tablets twice a day I have had more scans and MRI tests than I can even remember and still I have to constantly take the tablets, If Cannabis resin would control the fits I would be only to willing to try it
My son who has autism and epilepsy was having tonic clonic seizures for 7 years. He is 27. The last time he had a major seizure, he had 3 in one day. This never happened before and his seizures were becoming life threatening. The third seizure, he was turning purple and could not breathe while seizuring. We were at emergency at the hospital. They were pushing the anti seizure meds intravenously and pushing air into is lungs. His breathing was super labored for about 10 minutes when he started breathing again. I knew he could have died.
That’s when I decided to try medical marijuana. We started with a low dose of 0.5 oil on a dropper. He had 2 more seizures after but they were very mild. This was the first time he did not pass out and stop breathing and no injury! He even remembered the mild seizure and told me about it. We increased to 0.7 and a couple of weeks later he had another really mild seizure and we increased it to 1.0 which is a full dropper. This dropper is the same size as an eye dropper. He has been taking 1.0 since and has not had any seizures.
He also started having panic attacks because he was waking up on the street or in an ambulance or hospital with injuries. He had a broken nose and black eyes and cuts and stiches and concussions.
The CBD oil he is on now has saved his life! He is seizure free and is more calm and engaging than before. CBD will not make you high, but it can stop seizures. I would encourage anyone with epilepsy to try cannibis oil.
I guarantee if you found a gram of high CBD strain oil, not rick stein oil though as that’s different, you need the CBDV, imbue a grain of rice size every day for a week and you will find the seizures, 1 reduce in frequency, 2 reduction in their strength, 3 much faster recovery time; memories, emotions and general cognitive function restores much faster.
4, THIS IS THEIMPORTANT INFO: mix the 1g of CBD oil with organic coconut oil say 30ml is a good starting dose. Coconut oil binds perfectly with Cannabinoids and Terpenes when cooked at the correct temperature and time oil you can perform a process called decarboxylation. Cannabis produces phyto-cannabinoids in a carboxylic acid form that are not orally active at least at the CB-1 receptor sites, because they don’t readily pass the blood brain barrier in their polar form.
To enable them to pass the blood brain barrier, they must first be decarboxylated, to remove the COOH carboxyl group of atoms, which exits in the form of H20 and CO2.
Decarboxylation occurs naturally with time and temperature, as a function of drying, but we can shorten the amount of time required considerably, by adding more heat. The more heat, the faster it occurs, within reasonable ranges, and in fact occurs spontaneously when the material is burned or vaporized.
There is another mechanism at play however, which suggests that we need to control the decarboxylation temperatures carefully.
When we heat cannabis to convert the THCA and CBDA into THC and CBD, we are also converting THC to CBN at a faster rate. At about 70% decarboxylation, we actually start converting THC to CBN at a faster rate than we are converting THCA to THC, so as you can see by the following graph, after about 70% decarboxylation, the levels of THC actually start to fall sharply.
That of course means that the CBN also begins to rise and the medication is becoming more sedative.
You can tailor-make the exact oil to suit your epilepsy; source 1g of 50/50 THC/CBD ratio oil.
Put 20ml of heated coconut oil into a Pyrex bowl, also a thermometer you can put in the oven to monitor the exact temps.
Leave the solution in the oven for 2 hours at 138°C
Before Decarbing
THCa = 4.8%
Δ9-THC = 0.9%
CBDa = 9.9%
CBD = 0.6%
CBN = <0.1%
After Decarbing
THCa = <0.1%
Δ9-THC = 4.8%
CBDa = <0.1%
CBD = 9.1%
CBN = 0.2%
So, as you can see most of the CBDa was converted into CBD. And the THCa became THC then creates CBN.
I hope this is helpful, you can carry around the bottle of oil and just put a couple of drops under you tongue when required. I had a friend who was averaging 8-12 seizures a week and was prescribed midazolam in a pre-made 1ml syringe squirted in side of his mouth, which would knock him out cold within minutes for avg. 8hr each dose.
Within 2 weeks he was down to 2-4 seizures a week and by the 4th week of treatment he went 4 weeks with only 3 minor seizures.
Good luck and research what I have shared with you, it will change your life for the better.
Has there been any research into the apparent anti epileptic properties of THCA? A lot of anecdotal evidence is suggesting that raw THCA tinctures and extracts are more effective than CBD and THC but there doesn’t appear to be any peer reviewed investigation into this.
Please keep me informed………….Thank You
I lost my job to a seizure!
Marijuana could control my seizures but its illegal. Federal law takes precedence over state law Thus, medical marijuana is a trap. I researched the law about this issue. Naturally, I am elated about any cure for seizures, but I wouldn't get any medical treatment in prison.
F*** the government. I have to endure this fucking bullshit because of their prohibition laws. If not for this police state, I could buy the cure for my seizures. I'm not taking any risks on going to jail. Maybe when I was young and naiive. I've seen the government turn other harmless citizens into criminals. I'm not going to be their next prison bitch. These days, instead of trying to function at the expense of risking my freedom, I'm considering anarchy!
Got guns? I think that's the cure. Revolution.
Then I can grow my own medicine and to hell with the crappy side effects of pheno. Not that phenobarbital is as effective anyway.
I live in tuscany , Italy . The local law allows the use of cannabis for medical purpose , but it is not easy . I know many wich are in need of alternative of drugs . This region (Tuscany) consumes more than 50% of drugs more than the rest of the peninsula , the way of mental disease . I would like to ask if Bedrocan or Sativex work like Aldol or Seroquel or Risperdal . Does the cannabis can be used the same way of typical neuroleptics ? Sure our revolution is great , long live cannabis !
I have tried to get a Dr to sign my papers it is like haveing a flea fart knocking over a wall. It is great that papers are able to to get you to be legally allowed to smoke cannabis for medicinal reasons,but try and get a dr to sign the papers it is almost impossable. I have Epilespy that they have tried to control and it is impossable to get it under control. I feel like a lab rat with all the drugs they have tried on me. Also after takeing so many pills since I was 14 I ended up when I was 37 haveing to have emergency surgery. There was ulcers all the way down my esphogus and the reason for my emergency was a hole in my stomache that after so many yrs of takeing pills had burnt the hole in my stomache. When are they going to learn that chemicals aren't always the answer. I need to use the pot because when i use that i don't have as many seizures at all. Come drs sign the papers.
I feel so bad for you my mother also had the same i found a dr in michigan that gave her marinol it worked wonders for her i wish u all the best
Hello, I have such disease, as epilepsy. Doctors argue that this disease at me because of the marihuana use. But I precisely know that it not so. Where truth?