Clinical endocannabinoid deficiency (CECD) is a proposed spectrum disorder that has been implicated in a range of illnesses, including fibromyalgia, migraine and irritable bowel syndrome. So far, very little research has been conducted on this speculative disorder, but if it is found to exist, it could be responsible for these very common conditions as well as many related ones.
Clinical endocannabinoid deficiency (CECD) was a term coined only recently, in 2004, by Dr Ethan Russo. Until the field of research expands, this condition remains mostly a theory, but with very solid grounding. Essentially, Ethan Russo bases his theory on the idea that there are many brain disorders which arise out of a neurotransmitter deficiency, and that many other conditions may arise similarly out of a deficiency in endocannabinoids.
As it stands, Russo shows that there is some evidence suggesting that endocannabinoid deficiency is linked with migraines, fibromyalgia and irritable bowel syndrome. In this article, we explore the complex associations between endocannabinoid deficiency and some of these common pathologies. Overall, it is a complex notion that underlying many of these pathologies is possibly endocannabinoid deficiency as a cause, and there is still much research to be done in the area.

Migraine, serotonin and the blood plasma platelets
Migraines are one of the three conditions that feature common clinical and biochemical patterns that may point to underlying CECD. Migraines are thought to be influenced by endocannabinoid function, as areas suspected to be involved with generation of migraines are also affected by cannabinoid activity. Furthermore, the endocannabinoid, anandamide, with its role in pain modulation and serotonin transmission, is believed to positively affect sufferers of the condition.
The biochemistry of migraine is highly complex and poorly understood, but it is known that high levels of serotonin are present during attacks. THC and its endogenous ligand, anandamide, have been shown to inhibit serotonin in high doses (although low doses may increase its production), particularly in the platelets of the blood plasma. The platelets contain the body’s highest reserves of serotonin, which are also present in the enteric nervous system as well as throughout the brain. Serotonin release from the platelets is thought to be crucial to generation of migraines, and migraine is often thought to be a disease of the blood on this basis.
The effect of THC on the release of serotonin and the consequent relief from migraine are what ultimately point towards the possibility of underlying endocannabinoid deficiency. According to the research presented, anandamide deficiency may lead to increased release of serotonin, finally resulting in a migraine. With sufficient anandamide circulating through the blood and brain, serotonin release may be inhibited, therefore alleviating symptoms of migraine.
Fibromyalgia and serotonin deficiency
Fibromyalgia, a pain disorder which is widely considered to be neuropsychiatric in nature, and which modern medicine has very few treatment options. According to a 2014 survey by the National Pain Report, over 30% of fibromyalgia sufferers use medical cannabis as treatment, whether self-medicated or by prescription. Of those who reported having used medicinal cannabis, 62% reported significant improvement after treatment. This kind of self-report does not prove that cannabis is an effective treatment for Fibromyalgia, but indicates the need for randomized controlled trials testing this hypothesis.

In another study which documented the effect of nabilone on fibromyalgia sufferers, subjects experienced significant improvement of symptoms when administered the cannabinoid. Another study demonstrated that quality of life was markedly improved in fibromyalgia sufferers that self-administered oral or smoked cannabis.
The most recent study conducted on this matter took place in 2018. Twenty-six patients were studied and treated with medical cannabis over 10-12 months. Researchers reported a significant improvement in every aspect of their survey for patients, finding that even 50% of those studied stopped taking any other medications for their fibromyalgia symptoms.
Serotonin levels in the platelets are also known to be affected in fibromyalgia, although it is thought that deficiency of serotonin, rather than over-abundance, is responsible for the sufferer’s aberrant perception of pain. This disparity is not fully understood, and is somewhat surprising given the high degree of comorbidity between the diseases,
In one study, up to 63% of primary fibromyalgia sufferers also reported symptoms of migraine, in another, 22.2% of primary migraine sufferers were also found to have fibromyalgia. This disparity may be partly explained by gender differences, as none of the male migraine sufferers reported symptoms of fibromyalgia, and the latter disease is overwhelmingly experienced by women, who comprise 90% of sufferers.
IBS and the link between the brain and gut
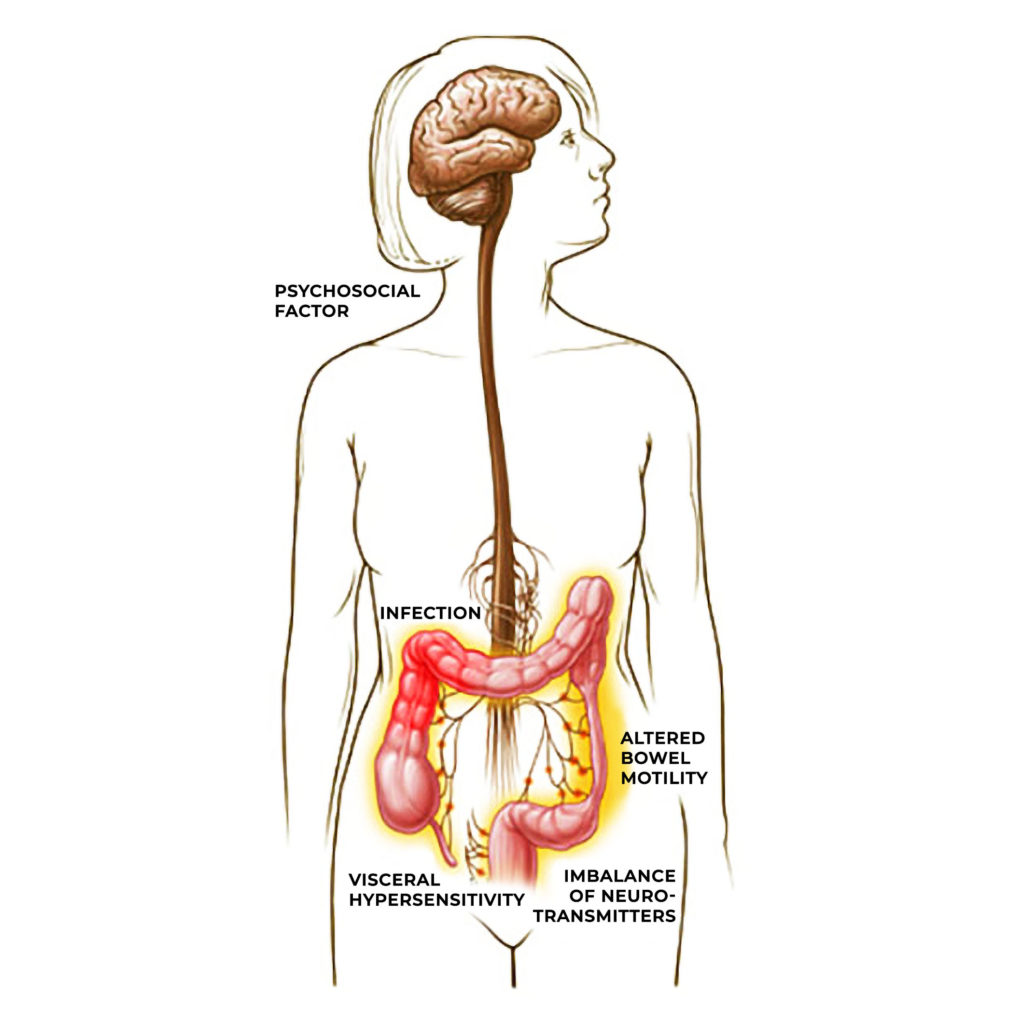
Irritable bowel syndrome (IBS) is a common gastroenteric condition that presents as bloating, abdominal cramps and diarrhoea. It has long been suspected that there is a link between IBS and neuropsychiatric dysfunction, as the condition is often comorbid with psychiatric conditions such as anxiety, depression and PTSD. Acute symptoms often arise in times of mental distress. However, as endocannabinoids are expressed in the enteric nervous system (ENS), as well as the areas of the brain affected by such psychiatric disorders, their effect may be independent.
Serotonin also plays a part in IBS, partially influencing gut motility (the peristaltic actions of the colon, which become “spastic” or uncontrolled during bouts of IBS), sensitivity and secretion of fluid. Interestingly, IBS-D (characterised by diarrhoea) sufferers have been shown to have increased blood serotonin levels, while sufferers of IBS-C (characterised by constipation) experience reduced levels of serotonin.
The effect of serotonin in IBS sufferers suggests a correlation with endocannabinoid deficiency, given that ingestion of cannabinoids affects blood levels of serotonin. With that being said, it is particularly difficult to pinpoint, as in certain cases serotonin levels deficient and in others serotonin levels are excessive.
Cannabinoid receptors in the enteric nervous system
It has been demonstrated that activation of the cannabinoid receptors in the enteric nervous system decreases hypersensitivity of the gut, as well as reducing gut motility and inflammation. Many sufferers of IBS use cannabis to alleviate their symptoms, although some report that symptoms worsened subsequent to commencing use; some even postulate cannabis as a trigger for IBS in certain individuals.
The overlap between instances of these conditions has led to the hypothesis that they are all expressions of the same underlying somatic disorder. Many sufferers of IBS also report symptoms of migraine, and up to 70% of fibromyalgia sufferers also present IBS symptoms. Many have all three, but it is not strictly necessary for all three to be present for an underlying condition such as CECD to be the cause, as many spectrum disorders manifest markedly different symptoms from patient to patient, and other related conditions may be involved.
Is an underlying condition responsible?
The idea that a dysfunctional endocannabinoid system is responsible for this postulated somatic disorder first arose within the last few years. In 2004, when the condition CECD was first proposed, researchers suggested that the high degree of comorbidity, along with the common feature of unusual cannabinoid receptor activity, pointed to an underlying disorder of the endocannabinoid system.
Many known conditions can be attributed to dysfunction of a specific neurotransmitter system: Alzheimer’s is caused by deficiency of the acetylcholine neurotransmitter, and Parkinson’s by age-related dopamine deficiency. It is therefore plausible to assume that deficiency of the cannabinoid neurotransmitters would also cause a specific disorder, or set of related disorders.
The relationship with the serotonin signalling system cannot be ignored when researching the possibility of CECD’s existence. Behavioural studies suggest that the effects of endocannabinoid signalling are mediated by regulation of the serotonin system. For example, THC has been shown to inhibit serotonin release from the platelets in migraine sufferers, as well as increasing synthesis of serotonin in the brain. 2-AG and cannabidiol have demonstrated similar effects. However, the independent effects of cannabinoids on the cannabinoid receptors are thought to be the underlying cause of CECD, despite this possibly fundamental relationship with serotonin signalling.
If the existence of CECD is proven, targeted therapies can be investigated, which would pinpoint the precise nature of the deficiency and determine the appropriate ration and dosage of supplemental exogenous cannabinoids. At present, treatment of these conditions is usually through ingestion of crude cannabis extract, or through smoking, which may involve wildly different cannabinoid ratios between cannabis strains. Due to the dose-dependent effect of many cannabinoids, relief of symptoms may not be adequate with some varieties.
- Disclaimer:This article is not a substitute for professional medical advice, diagnosis, or treatment. Always consult with your doctor or other licensed medical professional. Do not delay seeking medical advice or disregard medical advice due to something you have read on this website.









Muchas gracias. ?Como puedo iniciar sesion?
Hola,
Puede iniciar sesión en su cuenta en la parte superior izquierda de la pantalla, donde dice ‘Iniciar sesión o registrados’.
Espero que esto responda tu pregunta y que sigas disfrutando el blog.
Con los mejores deseos,
Scarlet
the clinical endocannabinoid deficiency is very effective. In my opinion these may help to support people for deficiency.
I have had IBS for years now. At least ever 2 days and won’t stop until I take Imodium. There is no way this can be stress related or anxiety. I would have to be stressed more than half my life which is no way possible. Pot makes my pain much worse and intense, so it’s not part of my health remedy. I still feel your looking at the wrong areas of the body and the brain is more related. There are so many factors of the brain involved. Memory, fibro fog, fatigue, headaches, IBS, etc.
I wish some company would make an effort to look at the hypothalamus. We are suffering and on disability, we need help.
Do you think this would help someone that has Parkinsons and dementia but doesnt have tremors.?
Dear Audrey
Thank you for your comment. Unfortunately, as Sensi Seeds is not a medical practice, we are not able to provide any advice relating to medical situations other than to consult your doctor or other licensed medical professional. This article, written specifically for healthcare providers who may not be aware of the many properties of cannabis, may be useful to you in talking with your doctor. You could also try to contact local medicinal cannabis support groups, if you have not already done so. In the UK, there is the United Patients Alliance (you can find them on Facebook) and in the US and EU there are many branches of NORML (google NORML followed by your area name). We hope this is helpful.
With best wishes,
Scarlet
It’s now 2017 but I was wondering if there are any studies or research projects planned for CEDC. Thank you.
My comment isn’t showing
Hello s,
Comments need to be approved by a moderator before they become visible. In the English section of the blog, the comments are checked every weekday in the morning, so it may take a while for your comment to be approved. It is possible that your comment (I don’t see it either!) was not approved because it did not abide by the conditions of use when commenting on the blog. You can read the conditions of use here.
With best wishes,
Scarlet
You seem to have overlooked an important fact. Chronic stimulation of cannabinoid receptors (CB1) by cannabis DECREASES the number of receptors (down regulation) and disruption of CB1 receptor signaling in the brain can result in mood dysregulation, depression, anxiety and stress intolerance. Also, CB1 modulates the rewarding effects of drugs and drug induced reward is associated with dysregulation of CB1 receptors. Both depression and PTSD are associated with down regulation of CB1 receptors
“Cannabis dependence is associated with CB1 downregulation, which begins to reverse surprisingly rapidly upon termination of cannabis use and may continue to increase over time.”
Subjective and behavioural effects of nicotine in humans: some sources of individual variation.
“Regulation of cannabinoid CB1 receptors in the central nervous system by chronic cannabinoids.
Studies over the past decade have determined that CB1 receptors undergo downregulation and desensitization following chronic administration of THC or synthetic cannabinoid agonists. “
“While the numbers were too small to determine if cannabis smoking regulates CB1 expression, published reports indicate that this is the case only in daily smokers”
“Previous data showed the development of tolerance to a variety of pharmacological effects of plant cannabinoids when administered chronically (5 days). This tolerance phenomenon has been related, in particular, to DOWN-REGULATION of brain CB1 cannabinoid receptors. Binding levels of CB1 receptors decreased ranging from approximately 20 up to 60% in all brain areas. ”
Effects of chronic exposure to delta9-tetrahydrocannabinol on cannabinoid receptor binding and mRNA levels in several rat brain regions.
ENDOCANNABINOID INFLUENCE IN DRUG REINFORCEMENT, DEPENDENCE AND ADDICTION-RELATED BEHAVIORS
“We discuss drug-induced alterations in endocannabinoid function that may contribute to various aspects of addiction including dysregulated synaptic plasticity, increased stress responsivity , negative affective states, drug craving and relapse to drug taking.”
2-Arachidonoylglycerol: a possible endogenous cannabinoid receptor ligand in brain
“Endocannabinoid signalling in reward and addiction.
Brain endocannabinoid (eCB) signalling influences the motivation for natural rewards (such as palatable food, sexual activity and social interaction) and modulates the rewarding effects of addictive drugs. Pathological forms of natural and drug-induced reward are associated with dysregulated eCB signalling that may derive from pre-existing genetic factors or from prolonged drug exposure. Impaired eCB signalling contributes to dysregulated synaptic plasticity, increased stress responsivity, negative emotional states and cravings that propel addiction.”
Endocannabinoid signalling in reward and addiction.
Stress intolerance is associated with anxiety and depression
From “New Perspectives in the Studies on Endocannabinoid and Cannabis: Abnormal Behaviors Associate With CB1 Cannabinoid Receptor”
“In conclusion, the present findings show that 9-THC may impair spatial memory, at least in part, by inhibiting glutamate release through the CB1 cannabinoid receptor. Also we suggested that h 9-THC induces abnormal behaviors such as catalepsy-like immobilization and aggressive behavior through the CB1 cannabinoid receptor. “
Hello Silvia,
Thank you for your comment, which I will bring to the attention of the writer of this article, and for taking the time to include links to the sources you have quoted. Unfortunately, as Sensi Seeds has a policy of link-free comments, I have had to remove them before approving this comment. However, I have replaced them with the titles of the research papers that you cite.
With best wishes,
Scarlet
Please tell me there is a way to be tested for CEDC! This was written with me in mind, totally! When I’m out of my “meds” (stopped big-pharma years ago) I can only go a few days before the issues (all above) start kicking in. After 2 weeks without I’m bedridden from the fibro and migraines.
Fibro, migraines, periphial neuropathy, IBS and autoammune rashes. I live in a state that is still illegal to medicate (sad). Whomever wrote this, please help me find the doctors testing for this so I can help get more info to build our case for legalization.
I wonder something I have been a daily smoker for many years and reciently due to moving and knowing no one have been with out for almost a month a few days ago while working I started getting foot pain and it’s progressed from mild to pretty much constant resembling neuropathy or gout .
im now after testing my sugar and finding it to be normal trying a Apple cider vinegar, vit C , kewi , low acid high alkaline flush. And just replaced poor foot ware for much better footwear.
I have no visible swelling but my nerves are painfully tender and my big toe is sensitive.
Trying this flush for a few days started today so no results yet but wonder if the lack of canabnoids is an issue.
Is there any blood test I could ask my Doctor to test for CEDC?
Thank you so much for all you help
Namaste`
Very interesting reading, I have Crohns disease, fibro, ehlers Danlos syndrome, arthritis, Raynaud’s, hyperthyroidism and have smoked cannabis for a few years now, I find it helps with nausea, helps me to relax more and helps with my sleep. I will continue to take cannabis as long as it keeps working for me, some agree some don’t but each to their own x hugs to all you chronic illness warriors all around the world
I have Fibromyalgia, Ankylosing spondylitis, gastroparesis, Hereditary Hemochromatosis, Chronic Fatigue Syndrome, PTSD, Depression, arthritis in several joints, chronic severe headaches that will go on for a month or more without relief. The more my conditions progress, the more the my body seems to add to the list. With the right strain of cannabis, I can hault the symptoms altogether while under its affects. With the right strain, I am a functional member of society. If I go without it, my body starts going back to the way it was before I started it, I can barely function. I am too nauseous for water to remain in my stomach. My pain level is unbearable. Before it, and without it, I literally don’t have the energy to sit, I have to remain laying down. Some aren’t right and only lessen my agony.
I have never used cannabis, but I do find it interesting that there is possibly another system in our body and that a plant exist that directly relates to that. God did create us, the heavens and the Earth. I do know that if you listen to your bodies cravings if may help. My niece craved butter and bacon fat when she was little. She has seizures, one of the dietary recommendations was to increase her fat intake. The comment I read about salt, made me think of my mom, who has muscle aches. I think if medical society focused more on foods and plants and balance of systems, we would be better off. I think we could be on to something with the Endocannibanoid system. Hope more research can be done and less restrictions can be given on a plant that may do more good than harm. I am sure, as always, it may be a fine line but we need openess to be able to address it.
Eating food high in salt and fat also trigger our bodies to produce our own endocannabinoids. What I would like to know is what would be better for our systems? Smoking actual weed, or just eating a bag of potato chips. Which method would produce the most beneficial amount of endocannabinoids in our bodies?
Excellent article on the subject, but I noticed one significant lack. Cramping and constantly spastic muscles are also serious symptoms of fibromyalgia which are relieved with cannabinoid replacement therapy. When diagnosed in 1996, I was fortunate to be loaned the first edition of this book: Fibromyalgia and Chronic Myofascial Pain: A Survival Manual (2nd Edition) Devin Starlanyl & Mary Ellen Copeland. The biochemical mechanics occurring with FMS/CPS are well known, the “neuropsychiatric” description is promoted by certain interests offering compounds such as Lyrica for treatment, referring to “overactive” nerves in their advertising.
You make an important point about cannabinoid content determining therapeutic benefits. Prohibition restricts access to the enormous variety of cannabis cultivars, many of which offer enormous therapeutic benefits for chronic conditions which “mainstream medicine” fails to offer significant relief. Imagine the progress which could have been made with cannabis in the past 40 years alone, if not for federal prohibition.
As a chronic migraineur for 25+ years, I found this article interesting. One point in your article that confused me though is the statement, “The biochemistry of migraine is highly complex and poorly understood, but it known that high levels of serotonin are present during attacks.” In all the literature that I have ever read regarding migraine and serotonin levels, it states just the opposite; that migraines are correlated with LOW levels of serotonin, even during attacks. In an article from the American Headache Society on the subject of serotonin and headache, this is stated, “Migraine and in particular, chronic headache sufferers, tend to have low levels of serotonin, and their serotonin level goes even lower during a headache.”
(http://www.achenet.org/resources/serotonin_and_headache/)
Can you please clarify this discrepancy? Thank you.
Hello Seshata I have a situation that is for me very troubling. I’m a medical mmj patient and I smoke and vape. However I’d prefer to consume edibles. After several months trying every dispensary edible known to man (have not tried transdermal) the edibles have absolutely no effect on me. Regardless of quantity and method of preparation/extraction. Is it possible that I’m endocannabinoid deficient and therefore that’s the reason I cannot absorb oral thc?
Also @ Karhy B do you medicate with edibles?
A erva é cura para algumas doenças e só por isso deveria ser legalizada-: -)
Marijuana is the only thing that HAS controlled my pain related to migraine’s and fibromyalgia. I’m on no pain meds other than Excedrin migraine, as needed. And this is after suffering for about 30 years, going through conventional doctor’s and treatments. Cannabis should be available to everyone, to keep it illegal or unavailable, is doing a disservice to everyone. I have 2 personal friends that were cured of inoperable, terminal brain cancer, thanks to what most know as “Rick Simpson Oil.”
please let me know if cannabidiol oil can help with my carcinoid tumor.
Without knowing more about your specific case I can’t comment.
I have to agree on this article and thank god science is relating the connection….I suffer from migraines,IBS and stress pain and fybromalsia….cannabis helps all three…there are even days I can wake up without one bowl attack, when its usually so sensitive..to swallow instead of spiting out the stuff in my mouth in the morning would set it off.
This material is not original, and is not properly referenced or attributed. A hidden link inside the text is inadequate. Please rectify.
I’m sorry, but what on earth are you talking about? I have provided no less than 20 sources for my arguments in this article. And whatever you believe about the adequacy of links within the text (which are “hidden” how exactly?), that is the way we link to sources in articles on the Sensi blog.
Very helpful article thank you!
I was just reading that serotonin is used to regenerate nerve cells in the spinal cord and brain. If cannabis is capable of this it would definitely help a wide variety of conditions and injuries. As a Multiple Sclerosis sufferer who also has Fibromyalgia and Migraines I’ve been seriously researching cannabis and the implications of it’s prohibition on the rise in autoimmune disorders. There is definitely a correlation with the removal of cannabis from society and the rise in neurological/psychiatric diseases. Great article!
http://www.nih.gov/news/health/dec2014/ninds-03.htm
A lot of factitious somatoform disorders being mentioned here
Seshata,
Was wondering if there have been any studies pertaining to this deficiency and drug addiction, in the way the receptors work. From my own experience with addiction of one of my son’s, it seems that when he is sober he does not feel comfortable in his own skin.
That is an interesting question and not one that I have had the chance to research in detail. I am planning to publish and update to this article soon; if I discover anything relevant I shall include it. Make sure to check back in a month or so!
Regards,
Seshata
Seriously now we are saying there is a deficiency of pot in people? This is taking advantage of people with severe pain many disorders like Fibromyalgia. Pot may help some but this takes it a bit far! And you wonder why we are not taken serious by the doctors!
No, that’s not what this article is saying. This article is saying that the endocannabinoid system appears to be dysfunctional in certain individuals suffering from a range of diseases that have a high rate of co-morbidity (ie they often occur simultaneously in patients). The endocannabinoid system is the system of protein receptors and their endogenous ligands (compounds that bind to the receptors and are produced by the body) that is found in humans and most other animal species. Compounds in cannabis closely resemble some of these endogenous ligands, such as anandamide and 2-AG – so closely, in fact, that they do a very good job of binding to the cannabinoid receptors. In individuals whose endogenous ligands are not produced in sufficient quantities, and who experience the above-mentioned illnesses as a result, treatment with exogenous cannabinoids (ie, those from cannabis) may help to restore the inherent imbalance and improve the symptoms of the disease.
Please, if there’s anything else you don’t understand, don’t hesitate to ask more questions.
Charlene: Actually ALL mammals produce their own cannabinoids. Cannabinoids are found in breast milk because it helps to calm the baby as well as make them hungrier so they will drink more, and allow them to gain the necessary weight they need to gain to grow and develop. We have CB receptors in the brain and in the genitalia. It has been proven that when we don’t produce enough of our own cannabinoids, we must turn to plant cannabinoids. Marijuana actually lessens pains felt by the user and has been proven in many lab tests. While YOU personally may not agree with the methodology, many users of marijuana suffer from many different issues, depression, anxiety, physical pains and the usage of marijuana allows them to feel like most people do on their good days. The timber industry is the reason for the criminalization of hemp. You should really do some research before making blanket statements as you have done.
You are a moron.
This could explain strokes are related to cannabis, people with migraines/RCVS are self medicating because they have an endocannabinoid deficiency. Otherwise we should be hearing deaths everyday from dabs, and see it in marinol and sativex studies since its concentrated cannabinoids.
Hi.
In most causes and cases,where distortion of neurotransmitters-especially seretonin,is involved-there is present a fungal and/or mold overload/infection.
The mycelium (vegetative filaments) of the fungus/mold,have taken over,grown alongside the nerve “threads”,stopping and messing with the normal flow of signals.
Causing auto immune disorders,drying of the joints,penetrating the stomach wall, and mucous membranes,etc.
The phosphor in the cannabis crystal glands,renew the cells-as this is there fuel.
Howdy! This post couldn’t be written any better! Reading through this article reminds me of my previous roommate!
He always kept talking about this. I’ll send this article to him.
Pretty sure he’s going to have a good read. I appreciate you
for sharing!
@Debbie: CBD is cannabidiol, which is a plant cannabinoid found in cannabis. THC is the other main component, tetrahydrocannabinol, which, when paired with CBD produces the psychotropic effect or high. There are also other cannabinoids, such as CBN, and terpenoids which are not cannabinoids but have some anti-inflammatory effects. You have to have both for not only the high but for many of the treatments in this article. CBD alone won’t do the job, you have to have whole plant cannabinoids in a plant form, either smokeable or vaporizeable or edible. You can even make tinctures. Unfortunately politicians in a number of states (Utah, Wisconsin, Missouri, etc) have enacted CBD-only legislation and are trying to pass it off as “medical marijuana”, which it is not. They intend to extract the CBD and throw away the THC (which, incidentally, is marketed in tablet form as Marinol). The only honestly-passed medical marijuana bills are for “charlotte’s web” strain which is high in CBD and low in THC. The politicians won’t admit this came from a dispensary in Colorado! Then there are the 22 states which have passed real medical marijuana bills, in which the whole plant and edibles are sold.
Not true about Marinol. It is a synthetic product.
Where do I sign up for this hemp vap pen thing your speaking of?
This information just dropped into my lap! Legal in all 50 states 32000 people enrolled for free until 3/31/2014 CBD /Hemp Salve and Hemp oil Vap pen more products to come. No medical claims guys. Check it out for me I have IBS , back issues etc tried and feel relaxed and better. Just sharing with y’all
Kathy D. can you tell us more about going to court. My son is executive Producer on a new movie http://www.thescienceofweed.com and i am curious to know more about your statement. also, for everyone, the first documentary he made is free and can help you talk with Doctors and family members and you can watch it for free at http://www.marijuanamovie.org
What are CBD’s?
Lyrica is helping me with fibromyalagia. I wonder if there is any relationship between lyrica and some form of marijuana. So far I haven’t found it.
Also, chronic depression can result from being in pain almost all the time, and I wonder about the link between EXCESS serotonin and the above conditions. However I did find that when I started taking Lyrica, I could stop taking Zoloft (a Serotonin re-uptake inhibitor) and still not suffer from depression. I had taken Zoloft for about 20 years.
http://www.ncbi.nlm.nih.gov/pubmed/18404144
Clinical endocannabinoid deficiency (C… [Neuro Endocrinol Lett. 2008] – PubMed – NCBI
I would like to read more articles like.this related to back pain & illneses and conditions to backrelated pain, I have horrible back problems & I know this miracle serum/ plant could help myself among many others who have similar problems
legalization is necessary in all aspects with response to social and healthy life.
no any more doubts…..
Kathy D. I agree 100%-although it would be even better if our government would stop trying to legislate morality-and telling adults what to do-and let us choose for ourselves. The drug war has been fought for 40 years-and we are further behind than ever-it will never be won, and it is not being fought for our benefit. As usual the government does what will benefit them, not the people who elected them and pay their salaries.
Excellent article! This has been my hypothesis for about 2 years–but being a PhD in Ethics and Social Justice vs. Medicine made my argument fall on many deaf ears…it’s good to see some validation coming forward. The key is in listening to patients and understanding how cannabis effects their symptoms–if our medical profession would stop and listen to cannabis patients the knowledge gained could lead research in many new and interesting areas!! http://www.CPNInstitute.Org
I suffer from Crohn’s, RA, Fibro, and Migraines….and major depression. If we could just get the medical community and government together to understand just a small part of the pain that we go through on a daily basis. All we want is pain relief without all of the side effects of narcotics destroying our organs.
This caught my attention!! I have every one of those problems and the pain chart for fibromyalgia was very spot on!! Please everyone help us fight for legalization/decriminalize and medicinal use!!! God Bless!!
Sounds plausible to me. I have all three, plus PTSD, arthritis, neuropathy, diabetes, and several other diagnoses that just seem to go along with rest. I notice that smoking helps about 80 to 85% of the time, there are those times that even cannabis doesn’t work.
I know of several persons who suffer from IBS, regular headaches, joints & muscle pain. These are all worse or initiated by times of increased stress, anxiety, depression. This article is very interesting, these could all be one illness, namely CECD.
Been looking for someone that is on the same page as me. Thanks!
Face book has a couple of good sites on there hemp Australia hemp Sunshine Coast
Have a look they have CBd charts n info on what’s going on with hemp study’s and findings
I hope you find what ur looking for.
Kindest regards
Jane
Several conditions may present themselves as IBS, including coeliac disease, fructose malabsorption,[5] mild infections, parasitic infections like giardiasis,several inflammatory bowel diseases, bile acid malabsorption, functional chronic constipation, small intestinal bacterial overgrowth, and chronic functional abdominal pain….–
Thank you for writing this article!
I proved to the court my long list of health issues is completely related to my having a dysfunctional endocannabinoid system. I have Celiac, 2 types of Arthritis, IBS, hypokalemia, a constant state of fever, and more. Without cannabis I am bed ridden and need medication that makes everything worse and turns me into a non-functioning person. With the miracle of cannabis I can live a normal life and all my health issues become so minor as long as I eat right I have no problems. Without it I will die and nearly have everytime I have had to quit. The court watched me, it took over 2 years but the hell and damage to my body is something I am still healing from. Cannabis must be available nationwide. There are so many people like me. Please encourage your lawmakers to reverse cannabis prohibition. Educate Everyone. Lives depend on it.
Nicely done Seshata,
In my view this explanation seem to key into one of the reasons it helps halt cancer growth and heal on so many levels. Are the studies based on ingesting or vapour?
I used raw cannabis after suffering from chronic thromboses hemorrhoids (internal and external) for 7 years. I have had multiple operations, tried many home remedies and finally got fed up and ate raw cannabis (3/4 oz w/juice) and my golf ball sized tumor shrank to nothing, only taking three days to heal. Since it is still illegal I did not get anymore and after a month it came back to its golf ball size and pain. I’m 22 and a healthy person. These symptoms (fluid, colon spasms and others) is what I experience. It’s not cancer and my doctor wants to send me to another state hospital. Why can’t my doctors locate the issue? They are not looking at the right system in my body, the endocannabinoid system. I would drive to CO and get enough oil to heal, if I had the resources.
My husband and I take UltraCell, a superior product in that it is a full spectrum hemp oil, using the entire hemp plant, and it is grown in USDA approved organic soil, so no harmful growing products are in the plant. (Hemp picks up all elements in the soil so if the hemp is not grown in organic soil it will pick up all the in the soil..
Full Spectrum means that all the other elements in the hemp plant are taken from the plant. Most producers only take the CBD from it. It is a more expensive process to take all of the nutrients from the hemp plant like Zilis does. (That’s the name in Swaheeli for Multiply Nutrition. (There’s a long story about how the name was chosen.)
The dosage is consistent. Most people take 1 gram per day, with half of that in the morning and half in the evening. Hemp has been proven to help diseases of the bowel and brain, especially. But it is helpful for any condition because it goes to the endocannabinoid system in your body and goes to the receptors needing the most help.
please send or post anything you find about the cannabinoid system and Schizophrenia. I have studied all I can and I know it can be used as an anti-psychotic with those properties in CBD. thank you.
I heard about these oral ingested oils at blue moon hemp. Com called CBD comes in different flavors not expensive that’ll help you with what you’re describing you are going through.
Do a little research on schizophrenia and vitamin d deficiency. I was very surprised on how much and how severely a simple vitamin deficiency could effect not just the body but the mind. Best of luck to you.
Beta caryophyllene found in black pepper and cloves is a cannabinoid worthy of further investigation.
Treats anxiety depression and psychosis without side effects, particularly effective when combined with probiotics.
Ethan Russos grand unified theory (GUT) of clinical endocannabinoid deficiency (CED) is interesting and may be helpful in your situation.
This is very interesting stuff, please let me know when you have more information/articles I would like to follow this story.