Menopause is the term for the stage of life when a female ceases to menstruate, and permanently loses the ability to have children. During this stage, various physiological and psychological symptoms can occur. Research shows that cannabis might ease some of those symptoms.
Strictly speaking, menopause refers to the point at which a woman has not experienced a menstrual period for 12 months; the years of biological disturbances either side of this point are known as the ‘perimenopause’.
The endocannabinoid system has a fundamental role to play in all aspects of female fertility, from initial fecundity, to implantation of the developing embryo into the endometrium, to delivery of endocannabinoids via breast milk. The endocannabinoid system also has a vital role in the cessation of fertility.
What is menopause?
During perimenopause, women typically begin to experience irregularities to their menstrual cycle, and levels of hormones begin to fluctuate.
During postmenopause (the years after menopause), women experience overall lower levels of reproductive hormones, along with an increased propensity for urinary tract infections, weight gain, and various other health complications.

Symptoms of the perimenopause
During perimenopause, which typically occurs between 45 and 55 years of age, various unpleasant and occasionally debilitating symptoms occur. These symptoms can be roughly divided into three types: vaginal/uterine, other physical, and psychological.
- Vaginal/uterine symptoms include vaginal dryness, pain during intercourse, and atrophic vaginitis (a condition whereby the mucous membranes of the vagina, vulva and related tissues become thinner and lose elasticity).
- Other physical symptoms include night sweats, heart palpitations, dizziness, headaches, stiffness, back pain, breast pain, urinary incontinence, night sweats, insomnia, and hot flashes.
- Psychological symptoms include anxiety, depression, lack of focus, memory problems, mood swings, and loss of libido.

Menopause and the endocannabinoid system
There is a relative abundance of research into the complex role the endocannabinoid system (EC sytem) plays in female fertility in general, including in the onset of menopause. Existing research has demonstrated that various fundamental changes to the endocannabinoid system and related biological systems occur during the menopause transition.
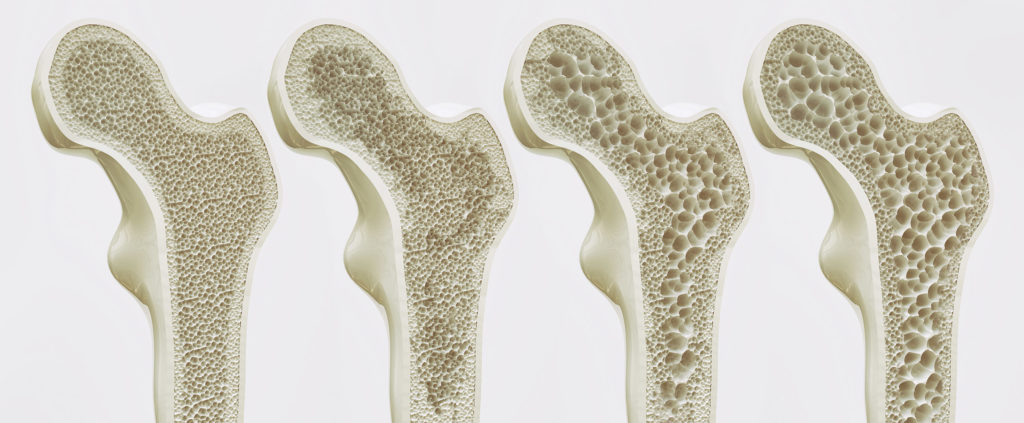
Menopause carries with it an increased risk of osteoporosis, which is itself thought to be related to changes in EC-system function in the skeletal system. A 2011 study found that in the osteoclasts (cells responsible for resorbing bone) of postmenopausal women diagnosed with osteoporosis, an overexpression of CB2-receptors caused osteoclast overactivity, causing bone to be resorbed too quickly.
Menopause also affects the body’s sensitivity to insulin, and may increase insulin resistance (which can in turn lead to the development of Type 2 diabetes mellitus) in some postmenopausal women. Furthermore, a 2013 Canadian study found that in obese postmenopausal women, those that exhibited insulin resistance also demonstrated higher circulating levels of the endocannabinoid 2-AG in the blood, lower levels of anandamide, and elevated levels of CB1-receptor activity compared with subjects who exhibited insulin sensitivity.
The link between the endocannabinoid system, the menopause transition and the risk of weight gain deserves further investigation. An earlier study, conducted in 2005 in Germany, found that in postmenopausal women, obese subjects exhibited a significant increase in both anandamide and 2-AG compared with non-obese subjects. A corresponding reduction in levels of the endocannabinoid-degrading enzyme FAAH was also observed in obese women.
How genetic variations to the EC system affect menopause
There are also genetic elements controlling the function of the endocannabinoid system at key points in the female reproductive life cycle. Research has demonstrated that individuals in possession of certain single-nucleotide polymorphisms (SNPs) differ in their physical response to menopause, in ways affected by the function of the EC system.
A 2011 study by the same Polish research team found that a different SNP, RS2023239 of the CNR1 gene, may be associated with an increased ‘free androgen index’ in postmenopausal women in possession of it. Increased levels of free androgens (male reproductive hormones such as testosterone) may in turn be associated with an increased risk of cardiovascular disease.
How can cannabis help menopausal women?
1. Osteoporosis
The CB2-receptors of the osteoclasts are fundamentally involved with the development of osteoporosis. It has been shown that SNPs in the CNR2 gene encoding for expression of CB2-receptors are strongly associated with the development of osteoporosis in postmenopausal women.
As well as this, it’s also now known that CB1-receptors also have a role to play in the development of osteoporosis. A 2005 study on mice with inactivated CB1-receptors exhibited increased bone mass and were protected from ovariectomy-induced bone loss. Several studies have also shown that antagonists of the CB2-receptors decrease bone loss; thus, inactivation of the CB-receptors appears to be key to reducing the excessive rate of bone resorption that causes osteoporosis.
2. Weight gain
While limited research into the altered EC-system function in obese postmenopausal women does exist, there are apparently no specific studies into the ability of cannabinoids to control or reverse weight gain in such cases. However, in general terms, it appears that CB-receptor blockers are potentially contributory in weight gain.
Several studies have demonstrated that the synthetic selective inverse agonist of the CB1-receptor, rimonabant, is capable of causing weight loss in humans. But this drug has been withdrawn from the market due to the potential for serious psychiatric side-effects including suicide ideation.
However, prevalence of obesity in cannabis users is much lower than in the general population, an association potentially attributable to a synergistic effect of THC combined with CBD. So, non-synthetic medical cannabis may prove equally (if not more effective) than any synthetic cannabinoid, and presents far fewer potential side-effects.

3. Insomnia
Again, no specific studies into the ability of cannabis to help with insomnia in menopausal women exist. There are, however, several studies attesting to the ability of various cannabinoids and synthetic cannabinoids to help. This includes anandamide and the THC analogue Marinol to speed onset of sleep, improve restfulness of sleep and reduce likelihood of awaking mid-sleep, as outlined in this 2007 review. CBD products may also prove helpful, since research shows it can increase total sleep time.
4. Insulin resistance
There have been several studies into the relationship between the endocannabinoid system, insulin resistance, and the development of diabetes. It appears that blockers of the CB-receptors are key to managing insulin resistance, as CB2-knockout mice exhibit reduced insulin resistance, and CB1-receptor blockers have been repeatedly shown to mediate diet-induced insulin resistance.
5. Pain
Again, countless studies into the ability of cannabis and cannabinoids to manage pain have been published over the decades, with the general consensus appearing to be that CB-receptors agonists are more useful than blockers in the management of pain. Both CB1-receptor agonists such as anandamide and CB2-receptor agonists such as the synthetic AM1241 have been shown to exert an anti-nociceptive effect in cases of chronic pain.
Inflammation often becomes a problem in menopause due to lower levels of estrogen, which can be a reason for pain. Since cannabidiol (CBD) has anti-inflammatory properties, it may prove helpful for inflammatory-related pain during menopause.
6. Anxiety
The precise role of the EC system in mediating anxiety remains somewhat controversial, and appears to be dose-dependent. Low doses of CB-receptor agonists appear to induce a anxiolytic effect, while high doses exert the opposite effect. Furthermore, CB1-receptor inactivation or deletion appears to induce anxiogenic effects.
7. Loss of libido
The CB1-receptor inverse agonist AM251 has been shown to increase sexual motivation, proceptivity and receptivity in female rats, suggesting a possible role for CB1-receptor blockers in the treatment of loss of libido in human females.
Again, CBD could be helpful here. Estrogen plays a part in promoting blood flow to the human vagina, helping with lubrication. With dwindling estrogen, this can be a problem. CBD is a powerful vasodilator, which could help increase blood flow.
Could cannabis worsen any of the symptoms of menopause?
1. Membrane dryness
Cannabis is certainly associated with xerostomia (dryness of the mouth). It’s also been widely linked in the popular press to vaginal dryness, although it appears that there is in fact no basis for this claim. A 2009 study entitled ‘Cannabis and Sexual Health’ appears to be the basis, but on closer inspection it’s apparent that the association between cannabis use and vaginal dryness was in fact too weak to reach statistical significance. Furthermore, the mechanism underlying vaginal lubrication differs in fundamental ways to salivation.
Indeed, there is evidence that cannabis can in fact enhance sexual arousal, which is more likely to have a beneficial than detrimental effect on the natural processes of vaginal lubrication.
2. Heart palpitations
Some evidence suggests that cannabis can trigger acute cardiovascular events in susceptible individuals. It appears that agonists such as THC are more likely to be implicated in such events, and thus it may be advisable to avoid THC if suffering from heart palpitations. This is especially true if at risk from any pre-existing condition.
In general, it appears that CB-receptor blockers might be useful as supplementary management of menopause-related disorders including osteoporosis, weight gain and loss of libido, whereas agonists such as THC might be useful in the management of pain, anxiety and insomnia.
- Disclaimer:This article is not a substitute for professional medical advice, diagnosis, or treatment. Always consult with your doctor or other licensed medical professional. Do not delay seeking medical advice or disregard medical advice due to something you have read on this website.











I am 63 and have been having hot flashes and night sweats since menopause at 56. That’s 7 years of not enough sleep! I think it’s probably genetic since my mother had terrible hot flashes and night sweats for over 10 years. In the last 6 months I started smoking marijuana and have also tried edibles. I haven’t had reliable success with reduction of night sweats. Some nights I have no hot flashes and some nights I have one after the other. I live in a country where marijuana is illegal. The marijuana I have found here tends to keep me awake instead of helping me sleep. Is this because of the strain of marijuana I have been using? Since it’s illegal I can’t go to a store or Dr. and ask for a strain to help with sleep.
Will cbd oil help more in this case?
Hi Kate,
Thank you for your comment. I am sorry to hear about your situation. It is highly likely, as you suspect, that it is the type of cannabis that you are consuming that is keeping you awake – sativa strains give a more active effect, indica strains are more commonly used to induce sleep and relaxation. This post explains more about the difference between indicas and sativas.
As Sensi Seeds is not a medical agency or practitioner, we cannot give any kind of medical advice other than to consult our registered healthcare professional. This article about the potential benefits of medicinal cannabis might be useful for you to show your healthcare provider if they are not familiar with it.
You may also find it helpful to contact a support group for medicinal cannabis patients. In the UK there is the United Patients Alliance, and throughout much of the rest of the world there is NORML, who should be able to put you in touch with a group in your area (search United Patients Alliance or NORML followed by your area name).
This are our pages on medicinal cannabis and medicinal cannabis strains, which you might also find interesting.
With best wishes,
Scarlet
the Indica strain won’t keep you awake,I smoke that strain regularly ,the sativa strain tends to act like a strong cup of coffee on me .the Indica definitely help’s me w/ sleeping, anxiety & my chronic pain as well as the horrible sweats .I also use CBD lollipops
( 45 mg’s ) hopefully this help’s .
Is there any down fall in using HRTs combined with medicinal for menopause symptoms. Night time hot flashes, heart pounding and waking up after 2-3 hours of sleep. And thats an improvement with HRTs. I need more than 3 hours of sleep and could use a break with nightly hot flashes.
I went through all of the menopausal symptoms, eventually medical tests–I had to have a complete Hysterectomy, including my cervix. 2012. Still have occasional hot flashes, night sweats. In the last 2 years, I am experiencing extreme painful intercourse—so we have stopped completely. Desire still there. I am devastated!
If youre not on hprmone replacement pls DO consider trying bio identicals. Most patches have bio identical estradiol but you also need to have some progesterone to have balance. Progesterone saved my life. You can get it otc in usa. Here in Canada i had to get it cprescribed and compounded at a pharmacy. Or ask for Prometrium pills from your gp or obgyn. No more flashes or dryness.
I am looking for the best strain to buy for menopausal symptoms hot flashes and so on helppppp
I’m back! last week i purchased some cookies with each cookie having 10mg CBDs to 2.5 mg THC….i ate one at 5:30 pm and another at 10:30 pm….for the first time since 1992 i slept without being awakened by hot flashes/night sweats….i did wake up a few times with usual turnings….but no hot flashes, for over 12 hours!!!!!
i don’t eat the cookies in the daytime, as i figure i can deal with the flashes, but i just want to sleep at night…..this has worked for 4 nights now….a fifth night, i didn’t eat the first one until 8, and then the second one at 11 or so….that somehow didn’t work as well….i think i need a lot of hours to get this fully in my system…it puts me a bit of a crimp in my style as i don’t want to drive stoned…and even that tiny bit of thc gets me a bit stoned….which i don’t mind as long as i am home….i’m getting used to that aspect as well, because i am such a lightweight….but hurrah hurrah! the only bummer, is it is so expensive. a pack of 10, 10mg cbd cookies or chocolates cost $45-50. at 2 a day, that’s $10 a night…..Yowsers!
Hello Magicis,
Thank you for your comments, and for updating us! It’s very good to hear that you are having such positive effects. It is also very likely that not eating the cookies til 20:00 does not work as well, since when cannabinoids are consumed in this way, they can take up to two hours to start working; sometimes even longer, depending on what else and how recently you have eaten, and what your metabolism is like. There is some more information in this blog post on smoking vs eating cannabis as to how long the effects can take to begin, and how long they may last.
It may be a good idea to keep a food/cookie journal for a few weeks, to chart what you have eaten and when – not just the cookies, but everything – so that you can work out how to get the maximum effects for your money. I look forward to your next update!
With best wishes,
Scarlet
i have had hot flashes and night sweats since 1992, so no solid sleep for this girl! are there no studies or info on how thc or cbds might affect night sweats….i can deal with the ones in the daytime, but i would really like to sleep for more than 2 hours at a time….can’t take estrogen because of family history….
Im in year 7 of menopause, never slept for years!!!! I am only 37years old and due to the fact I was waiting till my 30’s to have children this diagnosis of pof not only caused physical but also emotional damage… after being pushed to the end of my rope and feeling hopless and helpless my friend came over with a gram of medical marijuana. With a lil reluctance I smoked a small amount and within 15mins was able to get up and actually function including eating and cleaning my house..That night b4 bed I again smoked a small amount and lord behold I slept woke up once during the night a lil warm, but not soaked and shaking every few hrs as normal.. The doctors around here are anti mary jane so the chances of getting a script is none!! But I would highly reccomend it to anyone who may have the option (;x cheers!!
I have also been smoking green to help me through the menopause. It helps my mood swings,night sweats,insomnia, I am a much better person when I have had a smoke. I only need a couple at night. It has been a medicinal help.
I am a 58 year old women and I started to smoke pot in the late 60`s (my first time ) 69 and steady smoking since 1973 or 74 , and it has helped me more than anything , prozact was not for me it turn me upside down , but pot helped with anxiety depression the mood swings . I`ve done gone thru menopause and if it weren`t for pot I would not have any friends , family or social life cause I was a disaster , a complete mess I would not give up my license for pot for all the money in the world. valume made me crazy to. so I love herb even if it never was legal I would still find it on my own . and that’s that.!
I completely agree w/ you ! I am 58 & I smoked pot when i was a teenager. then i didn’t smoke when i was around 19 / 20 yr’s old & also stopped taking any type of medication’s ( asprin etc.) as i was going to be having kids & I wanted my body clean .When my kids were older , i started smoking again ,I can say that when i went thru menopause & even before that w/ the chronic pain I experienced , from water skiing
( barefooting ) injuries & my back surgery I was put on heavy pain med’s & xanax, i hated the way i felt on both of those not to mention the dependency to them .I am off the xanax & the heavy dosage of pain med’s now & I smoke regularly & use the CBD lollipops instead. Not only do i sleep better & am so much more relaxed , no anxiety, but i don’t experience the awful pain anymore & i feel so much better .I would NEVER stop smoking or using the lollipops EVER !!