The topic of cannabis and asthma is somewhat infamous among patients as well as within the medical community. Many patients are aware of how cannabis can positively impact their lives and many wonder if they can smoke cannabis despite their asthmatic symptoms. You’ll find the answers here, from the benefits cannabis for asthmatics and the do’s and don’ts of cannabis use.
Asthma is a chronic respiratory disease that currently affects up to 339 million people worldwide, causes approximately 1000 deaths per year. Cannabis has been used as a means of treating the symptoms of asthma for millennia, in various medicinal traditions including those of ancient India and China. What do recent scientific studies say?
1. Cannabis has analgesic (pain-relieving) properties
Although pain is not necessarily considered to be a primary symptom of an acute episode of asthma, studies have shown that up to 76% of patients experience chest pain during an attack. Generally, asthma-related pain is characterized by a deep ache or sharp stabbing sensation that develops gradually over the first few hours of the attack, and slowly dissipates as the attack recedes.

While there are no studies that specifically investigate the ability of cannabis to treat asthma-related pain, several studies into the general effect of cannabis on asthma have noted subjective improvements in pain. The known bronchodilatory and analgesic effects of certain cannabinoids suggest that they could be useful in managing asthma-related pain. Cannabinoids can do this both by reducing pressure and constriction in the lungs, and by acting directly at the nociceptors (pain-sensing nerve cells) themselves.
2. Cannabis is bronchodilatory
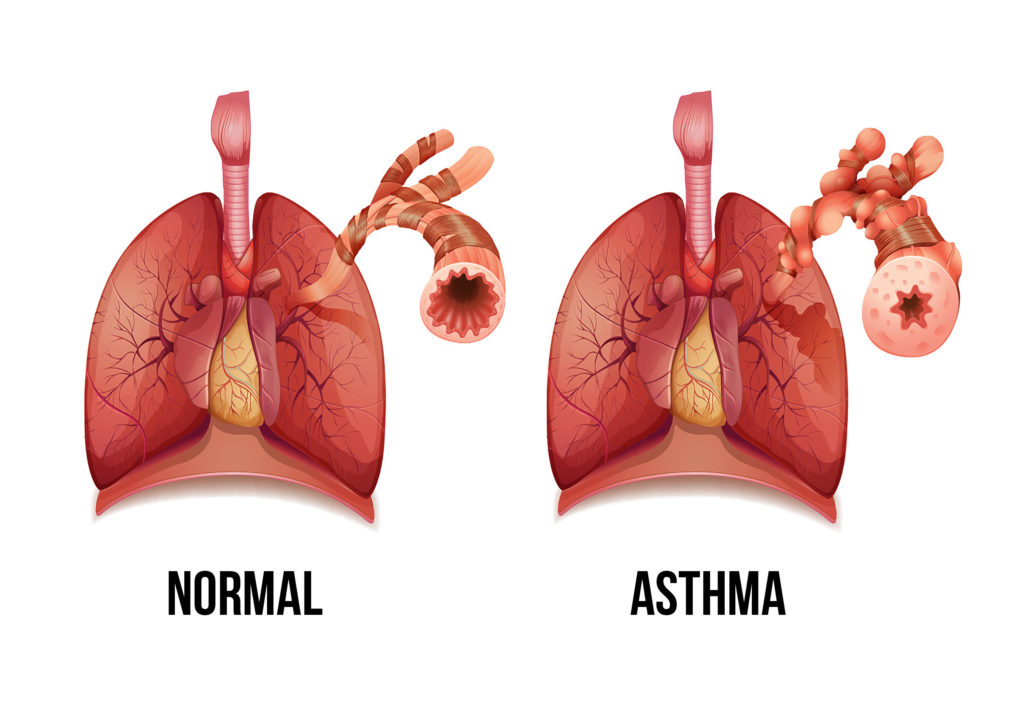
The ability of cannabis to act as a bronchodilator is perhaps its most significant property in terms of the treatment of asthma. During an asthma attack, the bronchioles (the branching network of tubes that carry oxygen to the alveoli) become constricted, causing the rate of oxygen flow to drastically reduce.
Generally, the extent of bronchoconstriction during an attack is determined by peak expiratory flow measurements, which are taken from patients and compared to readings taken in normal circumstances. The difference between the normal rate of airflow and the limited airflow during an attack can thus be determined.
A preclinical study showed that administration of cannabis in various forms can significantly improve bronchoconstriction both during an asthma attack and in normal circumstances (sufferers of severe asthma often have lower-than-average airflow compared to non-asthmatics even when an attack is not occurring).
In the early 1970s, a spate of studies were published investigating the bronchodilatory effects of cannabis for asthmatics. A study in 1973observed that cannabis smoke—unlike that of tobacco—caused a bronchodilatory effect; a 1974 study found that while the bronchodilatory effect of cannabis was weaker than that of isoproterenol, its effects lasted longer, and a 1976 study found that cannabis was as equally effective as salbutamol, although the latter achieved maximal bronchodilation somewhat more rapidly.
As with much of cannabinoid science, there are complicating factors. For example, a 2000 study found that the endogenous cannabinoid anandamide could actually exert a biphasic (two-stage) effect on lung tissue: it strongly inhibits bronchial constriction in the presence of an allergen or irritant (in this case capsaicin) but causes bronchial constriction in normal circumstances such as when no irritant is present. Indeed, some patients administered with THC have reported experiencing bronchial constriction. Thus, further research is needed to determine exactly how cannabinoid treatments should be used across the board.
3. Cannabis is an antispasmodic
It is thought that cannabis can exert a bronchodilatory effect mostly through its ability to reduce inflammation. However, it is also thought that cannabis’ ability to reduce muscular spasms (involuntary contractions) plays a significant role in the management of bronchoconstriction during an asthma attack. The bronchi and bronchioles are composed of smooth muscle, and during an attack, they contract and narrow as well as becoming inflamed.
In a study published in 2014, researchers took bronchial lung tissue from 88 human patients and subjected it to electrical field stimulation to cause the muscle tissue to contract. They then administered THC, the endogenous cannabinoid 2-AG, and various synthetic agonists of CB-receptors type I & II. They found that certain agonists of the CB1-receptor, including THC, reduced muscle contractions in a dose-dependent manner. Furthermore, it was observed that the endogenous cannabinoid 2-AG had no effect.
4. Cannabis is both an expectorant and anti-mucosal
The ability of cannabis to act as an expectorant is somewhat controversial. It has been used as such for thousands of years, and appears in the ancient pharmacopoeia of China and India, but modern research has been sparse and has thus far yielded only ambiguous results.
Countless people throughout the world report an expectorant effect after smoking or vaporizing cannabis. If it were noted only in smokers of cannabis, it could easily be dismissed as a result of the irritation caused by smoke particles. The fact that an effect is experienced even when inhaling vapour suggests that an active substance in cannabis is causing it.
However, most existing research actually points to the propensity of cannabis to cause production of mucus. For example, a study published in 2014 observed increased mucus secretions in habitual cannabis smokers, along with damage to the tissues of the airways. Thus, further research into the expectorant and decongestant effects of cannabis could be advantageous.
These were the top four benefits of cannabis for asthmatics as far as medical research is concerned. Next up are five do’s and don’ts when it comes to using cannabis as asthma patient. We spoke to one asthma patient, Mark, about his experience using cannabis with his medical condition.
Meet the patient: Mark
Mark is a Dutchman and one of the cannabis experts we have the honour of counting in the Sensi Seeds team. He lives in the Netherlands, where the weather can be very humid, and where pollen and various plant matter is known to fly around, even in big cities, and especially in spring.
Mark has suffered from asthma all his life, and has been medicating with cannabis for more than two decades.
In order to give a concrete reference to our readers, here are a few details about how Mark handles his condition, and the severity of his symptoms.
- Pharmaceutical treatment: Ventolin, 1 puff per day, Flixotide, 1 to 2 puffs per day.
- Cannabis treatment: Daily vaporization of dried cannabis flowers (approx. 2 grams per day).
- Physical activity: Mostly sedentary, with daily, average pace walking.
- Background: From very severe (daily severe difficulties + frequent attacks + regular visits to ER + antibiotic treatments) to manageable (aforementioned treatment + difficulties once to twice per year).
Due to all these years of self-medicating, Mark has accumulated a large amount of empirical knowledge in terms of what works best when it comes to cannabis and asthma. Read his do’s and don’ts below.

Cannabis and asthma: What to do? 5 Do’s
1. Choose vaporizing over smoking
Cannabis has the potential to alleviate symptoms experienced by asthma patients regardless of the method of consumption. However, this does not mean all of these methods are equal in efficiency. It also does not mean that using any of the least asthma-friendly ones is entirely harmless. Key elements to consider are:
- Optimal safety
- Potential for instant relief
- Controllable dosage and efficiency
Smoking cannabis is not recommended, as depending on the severity of your condition, it may escalate an existing asthma-related crisis, or even trigger one. Edibles, on the other hand, because of certain variables such as the time they may take to release their effects, can be used as a long-term treatment, but would not be reliable enough in the case of an attack. This is why for emergency treatments, vaporizing is definitely the best option for cannabis and asthma. Not only is the release of cannabinoids in the body close to optimal, the risks for the lungs are at an absolute minimum.
Of course, smoking cannabis is not harmful to the average, healthy human body. But, as an asthma sufferer, you need to watch out for anything that can irritate or negatively impact your respiratory system.
2. Select the best vaporizer possible
Needless to say, the quality of your vaporizer is of the utmost importance, even if you only use it for recreational purposes. To put it simply, a poorly manufactured or non-adapted vaporizer will not vaporize properly. For instance, combusting the substance used rather than vaporising it makes the entire experience fairly pointless.
And of course, if you are using such a vaporizer in the context of a respiratory disease, it could turn out to be a hindrance rather than a source of relief.
Buying pen-like items can be tempting for portability reasons. However, the smaller the vaporizer, the more chances key elements will underperform or simply be absent.
Based on this statement, home vaporizers have a tendency to provide satisfying performances. However, a number of portable vaporizers can also be of use. At Sensi Seeds, we are quite partial to two creations from our friends at Storz and Bickel, and many of us highly recommend them – including Mark, our patient here.
3. Learn how to vaporize cannabis
Consumers that use cannabis for recreational purposes often only have one objective in mind when they start vaporizing: to inhale some vapour. And surely enough, this sole objective leads most people to acquire, over time, a satisfactory method of vaporizing.
When vaporizing for medical reasons, it is necessary to inhale sufficient vapour without causing more irritation to the airways. For instance, a violent coughing fit can make an attack go from distressing to life-threatening in a short amount of time.
Mark’s ultimate method for vaporizing: Slow and steady wins the race; take small calm ’hits’ from your vaporizer, as if drinking a thick milkshake. Try to get some sort of calm vaping/breathing rhythm going. One hit from the vaporizer through the mouth, followed by three normal breaths (through the nose if possible). A three to five second vapour inhalation seems good enough, close to 10 becomes too much. Hold the vapour for a second or two and calmly exhale.
4. Optimise your vaporizing experience
Once you have found the vaporizer of your dreams, and you have mastered the vaporizing rhythm that suits you best, very little remains in your way. Yet, even the smallest things can become obstacles!
Avoid the most basic consequences vaporizing can have on your respiratory system by always having the necessary elements to counter them:
- Itchy/dry throat: always have a big bottle of water nearby and take sips regularly (do not wait for your throat to itch or until you cough).
- Go easy on your lungs: start vaporizing at a lower temperature such as 180°C (360°F). Work your way up if needed, but do not exceed 220°C (430°F). A flow of air that is too warm is not recommended for your lungs.
- Inhalation of plant matter: ensure your vaporizer’s accessories include mesh filters to prevent bits from travelling to your lungs, especially if you suffer from hay fever, a common sister disease of asthma.
- Regarding hay fever: do not rub your eyes after you have handled cannabis flowers
- Keep your vaping equipment as clean as possible using alcohol and lint-free cloths
5. Customize your vaporizer with a water pipe
Many vaporizers, especially home vaporizers, have the necessary connections allowing them to be hooked to an additional device. Connect a water pipe to your vaporizer, and vaporize through the warm water. This will help you inhale when your lungs are already in a bad shape.
However, ensure that the water does not get too hot as it could have the opposite effect. If you feel like your lungs are filled with mucus, opt for a dry vaporizing session instead. Warm, dry air is good for the lungs.
Cannabis and asthma: What not to do? 5 don’ts
1. Don’t smoke cannabis if you have asthma, let alone tobacco
Smoking tobacco can be extremely harmful to one’s lungs, mostly on a long-term basis. To asthma sufferers, its negative effects can have quite immediate impact.
Depending on the severity of your asthma, it can also be damaging to smoke cannabis. Vaporizing can provide the desired effects of cannabis, with virtually no danger.
2. Don’t use cannabis “dabs” (for medicating)
Dabs are becoming increasingly popular. Medicinal cannabis dabs are also gaining ground, but in the context of asthma, they simply don’t fit the bill. Dabbing does not equate vaporizing, as it can potentially expose your lungs to an overwhelming experience. Besides, the potency of most dabs can be a hazard, especially if you are already in a state of major stress and/or anxiety.
3. Don’t give up on your pharmaceutical treatment
It may be tempting to give up on pharmaceutical drugs altogether, especially when cannabis-induced results exceed expectations. However, existing anecdotal evidence, including this article, is not enough to guarantee safety in all possible asthma-related situations.
Asthma is by nature unpredictable, as it depends on literally hundreds of factors ranging from environmental ones to dietary habits, and even psychological states. Ironically enough, you could even experience a small panic attack following the realisation that your inhaler is not in your pocket, which could in turn trigger an asthma-related issue. Do not underestimate the multiple effects your prescription drugs can have on you, including the placebo effect.
4. Choose the first time you experiment with cannabis wisely
Waiting until your asthma symptoms manifest to try to medicate for the very first time is not recommended.
Instead, make sure to experiment in a peaceful, safe context, and while you are not experiencing any major respiratory issue. You need to acquire sufficient knowledge about your body, and how it responds to various degrees of cannabis intake. This means that you should be ready to counter any issue that could arise due to your lack of experience: possible coughing, inappropriate dosage, etc.
Once you have a clear understanding of how vaporizing can affect your breathing, throat and mouth, you can ease into using it to palliate to symptoms such as short breath, wheezing, tightness in the chest area, for recovering after a severe attack, and even to actually counter a full-blown asthma attack.
5. Don’t prioritise your desire to medicate with cannabis over your life
We understand the thrill of finding a solution to a medical problem that is all-natural, non-invasive, and possibly, overall more efficient. However, in the same way you should never solely rely on an inhaler to keep you healthy and safe, cannabis should not become your lifesaver. Keep your inhalers handy. And if you are experiencing a critical asthma-related issue, don’t try to talk yourself into good health. Try to gauge the situation objectively, and if necessary, call a doctor.
Are you an asthma patient yourself? Mark, the interviewee, and Jay, the interviewer, both are. Tell us about your personal experiences with cannabis and asthma in the comments section below!
- Disclaimer:This article is not a substitute for professional medical advice, diagnosis, or treatment. Always consult with your doctor or other licensed medical professional. Do not delay seeking medical advice or disregard medical advice due to something you have read on this website.












Hello,
By smoking weed people often mean smoking joints, from what I gather. I can’t smoke those without coughing my lungs out (I suspect that’s related to my asthma). However, I have a Gandalf pipe which I smoke weed from about once a year. Is that really that harmful? I mean, I don’t smoke a lot of it, and my lungs have plenty of time to recover, and I don’t notice anything, but…
Haha! I had to scroll all the way down here on my phone😂 took me like 1,000 swipes, phenomenal post i love the last one. It’s very easy to settle with something especially in a crazy world like we live in today. Life is a journey we should never be settling in anyway most definitely not our health for sure!
I was diagnosed of parkinson disease 5 years ago,i started azilect then mirapex as the disease progressed in frebuary last year,and i started on parkinson disease herbal treatment from Ultimate Life Clinic,few months into the treatment i made a significant recovery,almost all my symptoms are gone,great improvement with my movement and belance,it been a year and life has been so good for me.
amazing post ! Thanks for sharing.
You must feel stupid now after all the young deaths of cannabis vapors. No Smoking > Smoking > Vaping
Hi Barn,
Did you actually read the article? It explains using cannabis and cannabinoids to treat asthma; nowhere does it mention e-liquids, which contain the components believed to be the cause of the tragic deaths you are referring to.
This statement from the CDC details more about exactly which components are thought to be the problem: https://www.cdc.gov/tobacco/basic_information/e-cigarettes/severe-lung-disease.html
and although there is a correlation between e-liquids containing THC and illness, there is no proven causation. Given the warnings from the Centre for Disease Control about home-made e-liquids, it is likely that the problems are caused by tainted or incorrectly made liquids.
It’s a shame that you feel the need to use the deaths of young people to level such criticism towards the writers of a properly researched and responsibly written article that’s been fact-checked by an MD and is intended to help asthma sufferers. I hope you can find the time to re-read the article and gain a deeper understanding of it.
With best wishes,
Scarlet
Good answer scarlet 👍
CBD Oil works great for Asthma! Contrary to popular opinion, cannabis can help asthmatics in many ways. Though perhaps surprising, some research indicates that compounds found in cannabis can contribute to relieving certain acute and life-threatening symptoms of asthma.
Please can I have the name of the cbd oil it’s very important my son has severe asthma and Crohns. He’s 30. Ty so much
Kimberly,
Ambary Gardens out of Colorado makes their oils without pesticides and I have been using them for years. Additionally, Sunsoil out of Vermont is also wonderful. If you’re new to buying these, try to do research on the extraction methods employed by each company and if they’re using pesticides or chemicals.
Hope this helps!
CBD oil has been a game changer for me, after surgery it worked better on my incision pain than any pain med I tried. (and quickly) It’s helped with the panic and anxiety I get when I can’t breathe. Once I take it I can almost immediately feel a difference in my breathing. The airways feel like they open up and the inflammation is gone. The wheezing goes away and I relax. Fda won’t let me post which oil I use but if you message me I’ll tell you. It has more than one seal of approval from the Hemp authority, provides all their 3rd party testing right on the website for the public to see and only has 2-3 ingredients so it’s pure. You have to be careful because they are not all the same. fyi.. I use the full spectrum oil.
Dear Charlene. I just got diagnosed with asthma. In between my regular inhaler I get tightness and pain in my chest, so my doc put me on a rescue inhaler.
I would Love to get the name of the CBD full spectrum oil you use. I uses a CBD balm which sometimes helps.
Look forward to your response.
Hello,my name is Debby,I’ve been trying to educate myself regarding my treatment. I would like to know if possible; the very best CBD to spend my hard earned money on as I have always been hesitant to buy any, not believing it will work for me! Thanks for sharing your knowledge 😎
Hi Charlene. My son is having a very bad athsma flare up. I’d love to know what you use…<3
What brand are you taking? Thanks
I am concerned regarding vaporisation recommendations, I used a Volcano and organic flower, however still found a large tar build up on bags.
I read now that vaporising temps do not effectively destroy the wax cuticle that naturally occurs on plant leaves, this wax is thus vaporised and condenses and settles in the lungs. One only has to look at old vape bags to see the thick sticky tar in them. I found, despite promises, vape made my lung condition worse.
Lot’s of different reactions and claims re. the efficacy of using cannabis to treat or relieve asthma -and my own history with both is lengthy however, over the past 6 years (I’m in my 50’s now) I -underline the letter: I- discovered that while I do in fact have very mild asthma, I also suffer from VCD -which mimics asthma in some ways and is often misdiagnosed as asthma and does not respond to any asthma medications. Vocal Cord Dysfunction is something my Dr.’s never mentioned and seem to know nothing about. What I’ve learned is that it can be stress induced, seems to be tied to early traumatic events and naturally, cannabis is very effective in treating “attacks” so I wonder if some of the miraculous claims about how the Devils Lettuce helps with asthma, are actually people who unknowingly are treating VCD? There’s very little money to be made dealing with a respiratory ailment that big pharma can’t profit from so do your own research and figure out if you really do have asthma…
Hi Hans,
Thanks for your comment and sharing your experience, I’ve never heard of VCD before! I will do some research and perhaps make it the subject of a new blog post.
With best wishes,
Scarlet
What THC Cannabis strain is best on people with asthma, not causing the chest to pull closed or feel tight chested the next day
Hi Nicholas,
Thank you for your comment. As Sensi Seeds is not a medical agency or practitioner, we cannot give any kind of medical advice other than to consult your registered healthcare professional. This article about the potential benefits of medicinal cannabis might be useful for you to show your healthcare provider if they are not familiar with it.
You may also find it helpful to contact a support group for medicinal cannabis patients. In the UK there is the United Patients Alliance, and throughout much of the rest of the world there is NORML, who should be able to put you in touch with a group in your area (search United Patients Alliance or NORML followed by your area name).
These are our pages on medicinal cannabis and medicinal cannabis strains, which you might also find interesting.
With best wishes,
Scarlet
Today I was tired of coughing and using the inhalers and medication. I used CBD oil and checked the internet for information, just in case. I was using CBD for a while for back pain, but suspended it a month ago. That is the exact time I am suffering the asthma attacks. I used today sub-lingual CBD oil and no more coughing!!!!!
I’m interested to know what indica you think is the best for vaporizing for asthma?
Hi Tonya,
I’m afraid I don’t have an answer to this question; both the cannabis plant and the human body are such complex beings, with so many variables from specimen to specimen, that the answer is probably going to be different for everyone. My only recommendation would be to experiment to find out what works best for you.
With best wishes,
Scarlet
Can anyone advise me if one can use a Standard Dose (0,01ml per 0,5ml Medical Alcohol) of Rick Simpson Oil and then add 5-10 drops of that mixture with Saline Solution in a standard Nebulizer to nebulize with?
I do not have Asthma but am experimenting to see if I find a way that is easy to Nebulize and the effects I experince, possibly helping with my Sinus problems.
The drug for asthma from marijuana has been available over 10years now and has bee improved with a beta blocker .The name can be googled and is available by prescription in Jamaica.
Before it was available people drank a small amount of it as a home remedy
Sres/ras como es el consumo para el asma,y la artritis,se toma via oral
podrian informar en español
Saludos cordiales
Any thoughts on vaporizing dry herb versus oils for asthmatics?
Hi L, see my answer on that other asthma-related article you commented on:
Thank you for your question!
Obviously, there are differences between the two, but none that impact my well-being – I am the writer and my asthma is fairly mild. On the other hand, Mark, my interviewee, suffers from much more severe asthma, and he reports that buds are definitely his preference, because anything that’s oil (CBD oil, hash oil, whatever you have handy) will have a tendency to produce heavier/oilier vapour. This can be overwhelming for the lungs, depending on how your specific brand of asthma is treating you. So, as it often is, my best answer is: try and see for yourself? Start with small quantities of oil. And when opting for buds, if you are very prone to hay fever, make sure to use capsules so as not to inadvertently inhale plant material.
Good luck!
Jay & Mark.
Any thoughts on vaping dry herb versus vaping oil?
Hi L,
Thank you for your question!
Obviously, there are differences between the two, but none that impact my well-being – I am the writer and my asthma is fairly mild. On the other hand, Mark, my interviewee, suffers from much more severe asthma, and he reports that buds are definitely his preference, because anything that’s oil (CBD oil, hash oil, whatever you have handy) will have a tendency to produce heavier/oilier vapour. This can be overwhelming for the lungs, depending on how your specific brand of asthma is treating you. So, as it often is, my best answer is: try and see for yourself? Start with small quantities of oil. And when opting for buds, if you are very prone to hay fever, make sure to use capsules so as not to inadvertently inhale plant material.
Good luck!
Jay & Mark.
I know the article stated that edibles are not effective as a rescue medication for asthma but I’ve heard that they are effective as a daily preventative medication. Does anyone know if this is correct? Also is it only the THC that acts as a bronchodilator or are other cannabinoids effective for that as well? And how do you decide on doses for that?
I read through every comment and was amazed at the volume of asthma suffers. I too suffer from asthma and have great relief with CBD oil. The first night I used the oil I woke up to clear my lungs with coughing. It was like I took an expectorant. Then with only a few drops before bed I have had control of my breathing. The only time I have issues is when I forget to take the CBD. I wish you all the best of luck and relief.
I smoked yesterday night. didn’t have a lot of water and today I used my inhaler. I swear because of how it affected my lungs I got high from some of the weed being in my lungs. I know this sounds different or wrong but I have a lot of liquid in my lungs for my condition and I wonder if that has any relevanceyea
I ha e asthma and I have a constant cough that is very annoying!! I was wondering if cbd oil would help! Would appreciate a response, thanks!!
Hi Chris,
Thank you for your comment. We are sorry to hear about your situation. As Sensi Seeds is not a medical agency or practitioner, we cannot give any kind of medical advice other than to consult our registered healthcare professional. This article about the potential benefits of medicinal cannabis might be useful for you to show your healthcare provider if they are not familiar with it.
You may also find it helpful to contact a support group for medicinal cannabis patients. In the UK there is the United Patients Alliance, and throughout much of the rest of the world there is NORML, who should be able to put you in touch with a group in your area (search United Patients Alliance or NORML followed by your area name).
This are our pages on medicinal cannabis and medicinal cannabis strains, which you might also find interesting.
With best wishes,
Scarlet
Thannkyou for this article! I have been smoking for about 10 years. It has been harsh to my lungs but I did it anyway. Now I hope its not too late to undo the damage I’ve done to my lungs. I just never had access to what I needed in order to enjoy the cannabis safely. I felt like I was the only one with this problem. I know alot of stoners with asthma but none of them had problems smoking the way I did. I guess my asthma is just way more severe and I hate it. But Im happy to be a little more informed about ot. Thanks again!?
I am 14 years old and medicinally smoke cannabis due to my asthma, I use a plug-in vaporizer and it works GREAT. I found this post very helpful especially for the people that do not know the positive effects on inducing cannabis.
Thank you!
I have lived with asthma most of my life and for other medical reasons I can not use inhaled steroids.
Cannabis through vaping through an IceBorn helps increase my lung function by at least 200 on my peak flow meter.
I most appreciate Lemon Skunk.
Hey ,i understand that spliff joints are bad for astmha but if i use weed joints its can help to my asthma or only the vape
Hi Yagel,
As the article says, even smoking cannabis without any tobacco is definitely not recommended for asthma sufferers – do your lungs a favour and invest in a vaporiser! There are links to recommended ones in the article.
With best wishes,
Scarlet
Please post sources and or medical qualifications… Without a medical background I don’t know whether or not to believe you!
Hi Tom,
Thanks for your comment. The author of this article does not have medical qualifications, but is an experienced and diligent researcher and writer specialising in the field of cannabis. Sources are linked to throughout the article; the links are in green.
With best wishes,
Scarlet
Taking CBD oil has helped me a lot, I feel like I don’t need the Inhaler anymore
The most important thing is to take this as an Oil And it doesn’t get you high!!!
Asthma sufferers cannot afford smoke or vape use
Simply take the oil in a tea spoon
I have had asthma my entire life but I am new to the cannabis treatment and I was wondering if a vape pen would work as well as the vaporizors recomended?
CBD oil is helping me recover WAY faster after a workout and it keeps you lean.
What should I do for the anti asthma properties? Vape? smoke? Edible? what strain?
Hi Jinkies,
You may want to read this article for some advice: https://sensiseeds.com/en/blog/cannabis-asthma-dos-donts-patient/
Thank you for your message.
I have environmental Asthma. I don’t always have it act up. I suffer PTSD and Fibromyalgia. When the weather goes below 70°F especially when below 30°F in NY weather. I’m a medical Cannabis patient and has been since the 90’s (I’m California Native implanted in NY years later) The cold weather acts up my asthma a lot. NY only allows for vaporization of cannabis oil extract, drops, and edibles. I’m an old school Cannabis user. I gave up smoking for vaporizing as I get much better medical use out of it. My concern is when I use Ventolin. I generally wait an hour before I vape 3 good rips from a vape pen to a full lung and exhale, I don’t hold it in as long. This lasts a good 3 hours. I would never take ventolin and then vape right after. that would increase the heart rate unnaturally.
That is from my own experience. My Cannabis Doctor told me that there’s no conflict or interaction with my inhaler. He suggested it’s wise to wait an hour after use of ventolin before taking cannabis. I hope this helps those who are curious. Always be safe and ask your Cannabis Doctor. Never rely on Internet for medical questions.
Thanks everyone for suggestions, but please, when you mention your experience tell us in what form you used cannabis products…smoked it, used nebulizer, took orall. Please complete your sentences… and thanks, keep it up.
I’ve had asthma all my life and my experience with smoking weed has been good for my asthma ….now I’m using CBD oil and it’s really working for me…I feel more relaxed and my breathing is great….I think that MJ should be legalized because it safer than achohol and your not going to overdose or die from it …just think about it there is not one case in history where someone has overdosed from smoking weed…the feds don’t want it to become legal because then they would not be able to charge you with a crime it’s not because they care about you or me..I understand drugs like meth,cocaine,heroin,pills,and many other dangerous Drugs being illegal,but pot is no where close to being a dangerous drug it’s a herb for goodness sakes it’s all natural nothing man made like all this crap the pharmacy company push down our throats on television day after day..if you listen close to all them television commercials about this drug or that drug the side effects on 90% of the crap is not good for you….here are some of the side effects of weed …000000 there are no side effects you might eat yourself to sleep but your not going to die or have a heart attack ..or a stroke …your liver is not going to eat up from all them man made drugs and that’s what I have for now
hello I have had asthma all my life as i was born with it, but to the point- i am just curios i play a lot of sports and i mean a lot and i am looking to go pro with baseball so i am just wondering, does smoking weed decrease my lung capacity/will it make things worse? I enjoy smoking but If it is making my asthma worse i wanna quit. help?
Dear Josh,
Thank you for your comment. We are sorry to hear about your situation. Unfortunately, as Sensi Seeds is not a medical practice, we are not able to provide any advice relating to medical situations other than to consult your doctor or other licensed medical professional. This article, written specifically for healthcare providers who may not be aware of the many properties of cannabis, may be useful to you in talking with your doctor. You could also try to contact local medicinal cannabis support groups, if you have not already done so. In the UK, there is the United Patients Alliance (you can find them on Facebook) and in the US and EU there are many branches of NORML (google NORML followed by your area name). We hope this is helpful.
With best wishes,
Scarlet
I have suffered with asthma all my life and I am 20 and still do but not as bad as I used to when I was a little kid so one day I was curious about smoking weed so the first time in my sophomore year of high school. I took 5 garvs with my friend and then all of sudden I panic because I really thought I was having an asthma attack so I went to the er that same day! It wasn’t fun at all but I am really want to see if vaporizer will work for me as an asthma patient. Or even ediables.
Thanks for this! I’ve been battling with sports-induced asthma for several years now, and I’ve found that edibles helps. I’ve been making my own at home with Charlotte’s Web or Girl Scout Cookies, alternating depending on what I’m in the mood for. I’ve been toying around with the idea of using a vaporizer, but after reading your article I’ll give it a shot.
I did some research and decided to use cannabis habitually to see if it would help my asthma situation. At the time I was going through one albuteral inhaler every two weeks. (Crazy!) I hated the side effects of jitters and such. After one week of use I noticed a tremendous difference. After a month I no longer had to worry if I had an inhaler in my pocket. I threw it out. 2 years later I quit to get a better job, and here comes the asthma again.. My inhalers don’t work that well. I don’t even get attacks when I use cannabis regularly. Asthma should be a Debilitating Condition for medical use. But, it’s not where I live so I’m not eligible.
I would voluntarily partake in any study if it helps improve my lung capacity, i use 2 x asthavent inhalers monthly and i am on Nuelin tabs if i don’d take my tabs i cant breathe the day, yes i am obese, just mention walking and i cant breathe, i am so desperate this is getting worse and my quality of life and any assistance will be well appreciated at this stage. Tears in my eyes as i type. I just cannot anylonger
I have went from cigarettes to smoking marijuana and when I switched over from smoking cigarettes to marijuana I stop having asthma attacks for about 5 years and then recently the past year or so I’ve started having asthma attack and upper back pain I smoke maybe a half a blunt a day now when I used to consume maybe 2 to 3 blunts a day so I have cut back over in the morning time I have a skin tag like three or four in the morning have to consume my albuterol inhaler but I just want to know what is going on with the fat the upper back pain and if I turn to Vapor which vapor pen would be best for me or do I need to choose a bong thank you
I am a life long Asthmatic, with many attacks and 2 arrests, in my 20’s. My disease has been well controlled in recent years with Singulair, Symbicort and Reactine. I rarely use my Ventolin. The last few months have been hell, with major forest fires here in AB, Canola blooming and both following snow mold. I am so looking forward to Harvest! I have been vaping pot, with great success. I recall the first time I tried this. I was alarmed to the point of being scared. I had never before, IN MY LIFE, experienced full lung expansion. I have been tempted to drop my meds because I feel so fine. I will not do this. As you say, Asthma is very unpredictable. I can run and walk up to 10K’s.
I would like to share that I have a husband who suffers with Extreme Restless Leg Syndrome. Over a 5 year period, he was placed on no less than 30 medications. These meds were the likes of Clonazepam, Seroquel etc. They were designed to knock him out. The result was a man, wandering around and now stoned. He developed a paradoxical effect to all these meds. He was placed on a Parkinson’s med, by a Neurologist that proved to be ineffective. I gave him 1 CBD capsule and his legs quit jumping. He is controlled on 3 pills a day and is off the Parkinson’s med. Lastly, I am a Palliative RN. I have seen some pretty amazing things, in helping with pain and nausea. Thanks
Hi their, I am an asthmatic patient and I have had asthma ever since I was little, I used ventolin inhamer, the tablet and also seretide diskus, growing up. I only started smoking marijuana 2 years ago and I noticed changes in my asthma condition
1. Less asthma attacks, smoking weed made me feel calm, and unirritated because we all know irritation, to much cold or to much heat can cause an attack. My asthma isn’t too strong but it became stronger ever since I stopped smoking for a while, I found out that when I have an attack. It takes longer for it for it go relief me, I mean not using any drugs. Please am not saying smoking weed as an asthma patient is bad. Am just saying in a long run it can cause some problems but I can’t see the future for myself yet. But what I will advice is for asthma patients to not smoke cigarettes, because the smell makes me uneasy, uncomfortable. I advice that you smoke weed, maybe a joint or two, 2 to 3 times in a week. Let me just end this with to much of everything is bad. Just control your marijuana intake very well and don’t compare yourself to other people smoking cigarettes. Weed helped me with my asthma and I got too dependent on it, like the doctor said don’t be too dependent on it and forget your medical drugs. But now I hardly smoke weed but I like to smoke it. But I don’t want to put my self in the position of doing it to much. I hope you understand me
Hello I have asthma and i have all ways been told that if I smoke I will suffer with my asthma well like the kid who would never believe there parent’s i went out a smoked a cigarette and vaped e-juice and I suffer completely even when I stopped and I had to take steroids on top of steroids and breathing treatments everyday every 2 hours and now I’m better but I was reading thru articles and i seen that using cannabis could improve my asthma symptoms so I went out and smoked two joints and that day and the day after I felt fine my lungs felt clear I cough be cause my lungs felt so clear it was weird but I felt good and my breathing was good and i didn’t take any medication for those two days but the third day I had to take my medication but I notice a difference when I use cannabis and my daily medication and I feel better using cannabis as a my go to if I have a asthma attack or for my daily medication I feel that cannabis should be available for people with asthma
I was having asthma in my past and got into even more worse conditions. Then i started using cannbis CBD Oil products that really helped me in every circumstances. I was using CBD Oil which are made from hemp plant containing less than 1% THC. Soon above 2-3 months I was feeling normal and my breathing was also normal.
Cbd oil is made from hemp. You can get it without any thc in it and it is legal in all 50 states because it is made with the part of the plant that does not have any mind altering effect like the medicinal Marijanna.
You take it orally and it does help the lungs with out needing to inhale it.
Hi Steph, question as I’ve suffered from Asthma off and on for many years and particularly this year has been awful.
I just got some Pure CBD oil to put on my gums or swallow. You said its ok using it without the small amount of THC can still work for Asthma?
I love reading all the posts! Hope indeed 🙂
I am a 68 year old female. I began using cannabis because of asthma related COPD and systemic Epstein-Barr Virus infection. I have never enjoyed smoking it, but prefer to ingest RSO, and some edibles. I grow strains that are high in THC and calming. THC seems to quickly open the bronchial passages. But so far, I only ingest it at night about an hour before bed. It seems to open my breathing, greatly reduced inflammation, and I sleep comfortably all night.
The asthma I have developed is mostly environmental..chemical pneumonitis from years of being exposed to cleaning agents in hospitals and closed units in adult care communities. If I am exposed to chemical smells…perfumes, detergents, cleaning chemicals, I use a mild inhaler from a pharmacy outside the U.S.–insurance no longer covers this particular inhaler as it works and is very affordable for the consumer.
My first lung function test showed a 30% lung capacity. The Respiratory specialists sent me home to die. After only 6 months of the herbs–again from outside the U.S….and moderate cannabis ingestion, my new base line is 49% lung capacity! Quite a significant difference. Don’t know if this is relevant to the topic discussed here, but wanted share my experience with living.
Type you purchase? Where? Cost? I was just diagnosed with Severe Asthma and they are testing to find out what type of Immune system problem I am having. It’s like a never ending asthma attack some days.
I’ve been a marijuana smoker for like 20 years. And while in my area of the world we don’t use bongs and stuff, but rather roll joints with some tobacco in it, I remember my surprise back then when smoking a joint (even with tobacco in it) actually relieved bad cases of my asthma. I was young enough to not give a damn about it and internet was not that developed back then either, so it was just an occasional observation.
Times changed I stopped smoking joints as I no longer found that enjoyable, still my asthma persisted. I tried all kinds of alternative cures and eventually laid my sight on them vaporizers and THC oils as I certainly have no intention to die from organ malfunction few years from now because of all them corticosteroids I have had. After some research I narrowed my selection for my first vaporizer to Dr. Dabber products (still debating on which one or maybe something else will pop in the meantime). They have been reviewed in blogs and seem to be of good quality and not brutally priced (sorry, I won’t lock 500 Euro in my first vaporizer just to try if it works for me at all).
The other issue however seem to be the oils. I did not quite see anything about them in this post, except they are not that potent because of water content. Quite frankly as someone 40 with fresh baby, who drives and needs to work 9-5 and who does not enjoy the effects of marijuana anymore, vaping buds is not an option. Do you have any suggestions on how to select THC oil for medical purposes while keeping my wits with me?
Thanks.
Yes tobacco will bronchodilate you, they put bronchodilators in tobacco so you get a nicotine hit more deeply/strongly, thus making it as addictive as possible, and so that when you have f’==d your lungs up with tobacco, its tobacco that “comes to the rescue” when your chest is tight. The bronchodilators in tobacco help to mask the damage tobacco is doing so you don’t try to give up too soon ( ie – before you die from lung disease).
I wish I could put the tobacco companies into the same box that I will be in soon.
Has anyone tried a plain ordinary nebulizer to vaporize Cannabis Sativa Seed Oil? I added 1/2 of the seed oil, to 1/2 silver solution for dilusion of the oil. The vapor comes out of the mask beautifully, but I don’t know if this an effective and safe way to use the Cannabis Sativa Seed Oil. A nebulizer is a very effective way for me because I have a compromised gut system from Crohns.
Hello to everyone concerned. I am the leading asthma/Marijauna Guru in the World. No one has more info on this subject than me. Currently I am in battle with State of Florida and a sheriff named Grady Judd. These lawmakers need to be held accountable for their actions and I am in the process of organizing against their campaigns. Hopefully attorney John Morgan will be of great assistance if he is elected Gov in 2018. If I had my way I would make them pay restitution to every person arrested for possession. That is my goal ! For anyone who wishes to speak to me personally about asthma and cannabis I can be reached at my email address above. Cerely, Richard Jeffreey Wilkes Sr.
What about kids?
Could you please tell me how to get it legal in South Carolina??? help help help Where can I go to help an organization that is trying to obtain legal marijuana in South Carolina?????
Hi Richard Jeffreey,
I don’t seem to see your email address! Would like to contact you indeed.
Best regards,
Shady
I don’t see your email address
I would like to continue use, but am fearful as a fairly new asthmatic patient and constantly inflamed. Please, let me know how we can speak. I’ve got lots of questions. Thanks, happy thanksgiving!
I smoked yesterday night. didn’t have a lot of water and today I used my inhaler. I swear because of how it affected my lungs I got high from some of the weed being in my lungs. I know this sounds different or wrong but I have a lot of liquid in my lungs for my condition and I wonder if that has any relevance?
Hi Jay/Mark, thank you for sharing your experiences – your article is very informative, but I’ve just realised that this is not going to be a simple process – I feel at a bit of a loss as where to start?
My mother (87 years old) has had asthma all her life. She uses her nebulizer twice a day and has an asthma pump. She is on osteoporosis meds, Warfirin, suffers with extremely painful knees at night…. I just want to help her to be able to breathe and relieve the pain….
I don’t know if you can advise me on what I should try with her? If not would you know of anyone that could advise me?
Kind Regards
Janet
Dear Janet,
Thank you for your comment. We are sorry to hear about your situation. Unfortunately, as Sensi Seeds is not a medical practice, we are not able to provide any advice relating to medical situations other than to consult your doctor or other licensed medical professional. This article, written specifically for healthcare providers who may not be aware of the many properties of cannabis, may be useful to you in talking with your doctor. You could also try to contact local medicinal cannabis support groups, if you have not already done so. In the UK, there is the United Patients Alliance (you can find them on Facebook) and in the US and EU there are many branches of NORML (google NORML followed by your area name). We hope this is helpful.
With best wishes,
Scarlet
I have had asthma my whole life using all kinds of inhalers many times a day and have done alot of treatments with corticoids and nothing really works long term. i recently moved to california and started to smoke a strain of marijuana very high in CBD and less than 2% of THC. well well well my inhaler usage went down from 3 times a day to next to none. and i have been trying to find out why that has been happening and the only thing i changed in my diet, supplements or anything was the introduction of CBD at night to relax after work.
Is the weeds also effective for asthmatic patient if they smoke????is it safe for them????please give me more some info about this, i really really need it for my mom current condition
I have asthma and used a water soluble CBD product from dutch Natural Healing in a nebulizer 3 months ago. Got 30% more capacity in 2 weeks. My doctor is flabbergasted 🙂 My life has changed. Be sure to use a water soluble product. Oil or vape liquids won’t have the same effect. Tried them all. Good luck!
Hi, which product is it and how often did you use the nebulizer? Thanks
I am going to start with an organic Cbd/thc oil 20:1 ratio as I do not want to be high
I have lyme, lots of pain and asthma.. I can’t smoke anything so will the oil get to my lungs and work as an anti inflammatory there too like it should for my joint pain from lyme?
Dear Mary
Thank you for your comment. We are sorry to hear about your situation. Unfortunately, as Sensi Seeds is not a medical practice, we are not able to provide any advice relating to medical situations other than to consult your doctor or other licensed medical professional. This article, written specifically for healthcare providers who may not be aware of the many properties of cannabis, may be useful to you in talking with your doctor. You could also try to contact local medicinal cannabis support groups, if you have not already done so. In the UK, there is the United Patients Alliance (you can find them on Facebook) and in the US, Canada and EU there are many branches of NORML (google NORML followed by your area name). We hope this is helpful.
With best wishes,
Scarlet
CBD oils are doing miracles in me. I am using the best CBD oil in the market from this new company in the USA. Completely legal and no THC. Highly recommended. It has helped me with inflammations issues.
What is the brand of CBD oil that you are using?
That’s strang because I was told by a medical professional that you need both CBD and THC for it to work. Even if it’s only a tiny bit. Something to do with metabolizing.
We bought some cbd oil and I was afraid to try it because I have Afib, but I am having so many problems with my asthma, I have decided to try it. I just put some drops under my tongue. I sure hope it helps.
As a asthma sufferer for 27 years. It wasn’t until I started smoking marijuana that my asthma goes away. I’m allergic to things such as pets, pollen, cold weather. Every time I’m around those things my asthma flares up but one day I was at a friends house who happen to have 2 dogs and I felt like I was suffocating about to pass out. My friend gave me a little mj rolled up and the asthma went away right away.
Another scenario when I moved to Los Angeles I lost my albuterol inhaler. With no insurance I just had to give marijuana a another chance. Rolled it up on raw paper and it hasn’t been back since.
So I do strongly believe Marijuana is a great substitute for inhalers.
I can tell you definitively that THC acts as a bronchiodialator. I have had several asthma episodes in the past. While visiting CO in the winter, I caught the flu and developed pressure and soreness in my chest, shortness of breath, wheezing, and an unproductive cough. With the simple intention of enjoying an edible for fun, I ate 1/2 a gummy. A couple hours later I noticed 80% or so reduction in my symptoms. This can’t be placebo effect because I wasn’t expecting this effect.
Can someone send me the info of how to get started and what I’ll need. Ive had asthma all my life and need assistance when trying cannabis. Is there a pill form and machine to use? Is there a guide?
Dear Shelby,
Thank you for your comment. We are sorry to hear about your situation. Unfortunately, as Sensi Seeds is not a medical practice, we are not able to provide any advice relating to medical situations other than to consult your doctor or other licensed medical professional. This article, written specifically for healthcare providers who may not be aware of the many properties of cannabis, may be useful to you in talking with your doctor. You could also try to contact local medicinal cannabis support groups, if you have not already done so. In the UK, there is the United Patients Alliance (you can find them on Facebook) and in the US and EU there are many branches of NORML (google NORML followed by your area name). We hope this is helpful.
With best wishes,
Scarlet
I suggest using the oil and just putting it in your mouth twice a day or vaping it…if you read the other comments here it’s been helping a lot of people! Hope that helps!
CBD Oil works great for Asthma!!
Hi all,
Every time I have a strong wiff of pot I go into a full blown Asthma attack. I’m curious if anyone similar has tried the canniabs inhalers. Really would like off the steroid inhalers.
Yeah Scott, my neighbour/s smoke and in the past few months I have noticed an immediate attack once Instart smelling the stuff. It is a different strain to what I’ve smelled before so it could be that.
Lol, so I am not the only one that is affected by smells! Just strong smells it seems to get my asthma started and then I have to control it. I have a friend that smokes pot so every time I am at his place lol my asthma is a mess. I’ve had asthma all my life so used to it but I’d love to get off the meds it really turned me into a couch potato. I used to be really active when I was younger asthma wasn’t as bad but the older I got the worse it got.
I am old geezer from Colorado and the jury is still out for me. I remember back in the 70’s the first time I smoked pot it was a revelation. I could breathe. The first time really blew me away as that was not even on the radar. So I smoked through high school and 2-3 years after. I have chronic asthma and lung volume was in the 70’s when I was in my twenties. Then I really did not use marijuana until the past three years or so. I have read where THC is a good dialator but I really cannot say I get the effect I had back in the 70’s. Now I have severe COPD and sometimes I actually think it suppresses my breathing and I do not oxygenate as well. I have tried a variety of strains and mixed strains, sativa, indica, CBD oils, THC oils, scripts, home grown, vaporizers, nebulized, oral, through the skin, etc. All have a similar effect.
One thing CBD does very well is take the edge off anxiety and fright. For that, it is truly a blessing.
Greg…I’d love to know if you ever do find a Strain that you can vape that works well for your COPD. Do come back and let us know if this happens, and which strain works for you. Thanks for your testimony. 🙂
I’ve had asthma my whole life, I started smoking around 15. Sounds bad I know, but I used to have around 6-10 asthma attacks a year, spending up to 3 weeks in the hospital at a time… ever since I started smoking, I haven’t had another asthma attack since.
To be honest, I’m going to start vaping smoking the bong doesn’t do much help, a lot of people’s comments have persuaded me to give it a shot, though!
I am asthmatic since 25 years just tried the hash for the 5th times… donno what to say. Im using it with cygarette but till now nothing changed. Ur opinion guys
i think hashish is realy good for asthmatic patients.The only problem with it is how most people abuse the use of the herb.
countries in the world must take a second look at the herb and regulate it uses, since it has been helpful for some of us with asthma since childhood. The use of medical drugs does not help but rather leaves the problem reoccurring
Medical scientist that have researched into the effectiveness of cannabis should help us
I am coming off and asthma attack in the last 24hrs. I can assure you that i use a vape as well and it helps break up the mucus and as a result I dont have the panic attack that comes from not breathing. I still have to use some medications but not as much and would certainly be admitted to a hospital w/o it.
My airways are so inflamed now that I can’t even smoke but I have been making my own oil and it seems to be helping. I would love to be considered for a study if there were to be one.
I am asthmatic since 1994 am now 55yrs . How do I go about vaping and what substances do I use and how do I administer the mixture having no tube here.????
I used to smoke years ago and when I would smoke hashish, My asthma would be cleared right up I could run a mile. Will I quit in 2002 for my job. Now I’m ready to start again . I’m laying here in bed breathing like a madman. Steroid pump taken and now 2 puffs of my pump. I’m ready to try something again I just not sure if I can handle the buzz anymore. I would also like to try for all my aches and pains, I work Construction for 25 years my body is beat up. Tendonite’s in my right arm fullblown pain at this point. Again on pills. Tired of taking pills. Need some thing Natural. I was told to look it up here since this was the way for me to go…
I have severe asthma and was hospitalized and put on insane amounts of steroids to help clear up my lungs. The steroids only made me feel worse and I didn’t feel like my lungs felt any better. I started smoking marijuana and not only did I feel the best I had in months but my lungs have never been more clear. I definitely suggest medical marijuana to anyone with asthma because it has been proven to open up the bronchial tubes and help breathing.
Thanks i have a problem whit my asthma and my vaping..
Ive used cannabis for ten years and am an asthmatic from birth. It like anything else has side effects, despite being good at what it does. If these side effects dont inhibit your life but the actual use of the herb increases your Quality of life then perhaps cannabis and you are compatible. Do your research, love your body. It’s only natural.
Very nice to here from a real asthma patient about his experience. This is some very valueable informations for lots of people. Thanks for that, I’ll send this article to couple of clients. Thanks!
I have used cannabis for a long time to treat my asthma. Strain is extremely important. But I do use a sm g pen to vape bubble hash as my new inhaler. It works perfect! Even as it heats up,it allows for the sm claim hits you mentioned to start the process. I have a nebulizer that I’m supposed to be on 2x/d… advair 2x/d and Ventolin every 4hrs,and my asthma is triggered by nearly anything under the sun. Lol. Since I started to use my pen, I still use my advair. But I’m down to never using my neb and maybe needing my rescue inhaler once every 2-3days. I consume roughly about 1gm BH every 2wks. ?
What kind of strain do you recommend?
Wow thank for posting this information my asthma is extremely bad and I have zero idea about weed but if it will help me then I wouldn’t mind trying it.
Every thing is cool except I have had asthma all my life and I use dabs daily for my medicine. not only do I have asthma but spinal cord damage. Dabs require less vapor to provide effects. The temperature issue you raised makes 0 sence no offense but the terpenes and cannabinoids found in flower or hash are the same which means they vape at the same temperature. The issues raised should have been butane and solvents being harmful to asthma patients also using non solvent forms and how terpene such as pinene are bronchodilator.
Hello Kevin,
Thanks for your comment. However, there is no mention of temperature in regards to dabs. We do not recommend dabs for asthma patients as their potency/high levels of THC can in some cases, not only overwhelm, but can also trigger the opposite reaction (difficulties breathing).
We assume whoever has experimented enough with cannabis and wishes to dab for their asthma, will do so regardless. This article is meant to be completely safe to the patient who wishes to medicate for the first time.
I have been smoking weed for years but started dabbing a little under a year ago. I have since been diagnosed with asthma and to be quite honest dabs are what put em in a position where my lungs were working at 22% capacity. I LOVE dabs, but as far as asthma goes not everyone is going to be able to use them unfortunately. Not without steroids to counteract the damage. Like you guys said that doesn’t keep me from dabbing though. I do not recommend. I’m here to find healthier ways to smoke so I am still able to smoke!
As a cronic user of cannabis and an asthma sufferer, I can assure you the dabs will catch up with you. Its hard to type this is I love extracts but it just doesnt agree with the asthma long term.
Thank you for this information. Although I don’t smoke it, but really, for the sake of this generation, we have been fighting against drug trafficking. Fighting against a drug that many scientist already proved they can cure several sickness.
Its an herb/plant/living, like lavender, chamomile, rosemary, thyme, oak, ivy, tulsi, tea, coffe, elder, rose, hydrangea, datura, oliander, etc; not a drug. Sure some plants you don’t want to use or consume, they will make you sick and/or kill you; like some of the later mentioned. Oliander, BAD TO CONSUME/DO NOT CONSUME, yet is completely decriminalized and an insane amount of people use it for ornamental horticulture and plant everywhere even though its a usually non-native plant, and a poisonous plant, to all{us,animals,(minus humming birds and bees)} All parts of Cannabis are usable/consumable. Not all people can consume all things, that’ fine they shouldn’t. Making it ILLEGAL to grow,consume,share,use should be an outrage to the entire Earth, Because there have been humans sentenced to Death, imprisoned for over 50 years, fined, families have been broken apart, and more. 3000+ years of medicinal usage as well O_O! Until we can see it that way, not even close to change. It became a horrific scary “DRUG” in the 1920’s. Decriminalization gives us the power to heal ourselves(LEGALLY), Legalization allows wealthy people to give us our medicine legally.
I had asthma since the age of 4-5. Breathing machine treatments, steroidal inhalers, other inhalers, that circular purple powder inhaler, everyday. . . . I started smoking herb as a teen and have had to use an inhaler maybe 3 times, I’m 26 now, and i believe I only had to use the inhaler those 3 times because I smoke tobacco and had no herb to open my lungs. I still have my inhalers around, hidden, somewhere. I give thanks for CREATION and the herbal medicine! With respect thanks Yah’ll
Marijuana, really…????? I doubt….
Everybody is entitled to their own opinion! In my case marijuana and asthma is not a good mix! I can’t stand the smell of it when my asthma flares up. It makes me cough worse and I feel like if you’re an asthmatic consult a doctor and get the proper equipment needed for this particular disease.
Use a vaporizer, get a Volcano if you can afford one and vape AC/DC or Charlottes Web. If you don’t like the smell of it take the smell out with a water cure it gets rid of all the dirt, bugs and chlorophyll. Its usually the chlorophyll that makes you cough when it hasn’t been cured properly. Take small sips of the concoction so that your lungs have a chance to acclimate, if your lucky you’ll get some relief and if your unlucky you haven’t lost anything by trying.
No…don’t ‘smoke’ it…use a vaporizer and bubblers/bongs to cool the Marijuana vapor.
I have had asthma from a very young age, I have been using cannabis for a number of years now and have found that it does improve breathing when an attack flares up. Howvevr it only lasts for a while , in the past where i did not have my inhaler to releive the weezing i have used cannabis as an substitute and worked well
I think if something helps you feel better u should be able to use it
I have asthma, had it all my life, and I have been using cannabis for almost twenty years. For 19 of those years I have been smoking it. And with asthma the side effects were nasty. I was always coughing, using my asthma pump or nebulizer medicine. I would wake up coughing and spit up horrid yellow and black flem…yum.
It got so bad that I knew that if I didn’t find another way I would have to stop, or risk serious medical complications. So, I decided to try vaping….
And the results are beyond anything I could have expected. I began a year to vape a year ago after I got the Ascent. My body immediately began to repair my lungs and after three weeks I noticed I was using my pump less. Not going to bore you more but in the end it has been about eight months since I have had to use any asthma medicine.
And all I do is vape at least once a day. I notice my breathing is better after. My chest feels less constricted. I feel bad cannabis works more effectively.
Please I’m an asthma patient and I need the vape instrument buh I can’t get so here in my country can u help me to get one, cause I dnt want to smoke
To build a simple vaporizer: Use a clear glass jar (maybe a liter size) with screw lid for chamber- it goes upside down on top of the base which is usually a plastic or wooden container and maybe a liter or two capacity. Turn base upside down and attach lid for glass jar with screws or bolts to its bottom (now top; include rubber seal between if desired). Jar should be simple enough to attach or detach by screwing onto lid. You need a 100w light bulb- incandescent and as small as you can find. Mount its fixture near center of lid. Create hole in lid and through base to allow power cord to pass out of chamber and into base- this hole also allows air to enter the chamber. Base needs two more holes near bottom; one for power cord to pass and air to enter, and one a tight fit for hose (flexible and maybe 1 cm diameter) to exit. Make another hole the same size in lid and base, to allow 1 or 2 cm of hose to enter the chamber, but not too near heat from bulb.
Detach jar and create a small ‘crown’ of aluminum foil to sit snugly on top of light bulb (a pointy light bulb works best for this reason). Place material to vaporize in the foil. Carefully attach jar. Plug vaporizer into current- please be careful. After a while, vaporization begins. Inhaling vapor through hose should draw air into base and then chamber. Allow bulb and hot jar to cool a few minutes before detaching lid. Worked for me, but build and use at your risk.
I am currently experiencing the same thing! I have a nebulizer machine next to my bed. I wake up on the middle of the night every night having to use it. On steroids daily and still having attacks. I have severe asthma and use cannabis daily but I feel the smoke from dry herb exacerbates it. I’ve been looking into gettin a vape and using more oils. Has this helped for you?
What do you vape? CBD or MJ – if MJ then what strain, Indica, Sativa, % of each? How much and how often?
How can i use marejuana to treat my asthma, to smoke is the best way or is there any other way to use it.
How can i use marejuana in the best way to treat my asthma. To smoke it is best or is there any preparation to use it.
I have asthma returned now, since I’ve stopped smoking now for a year do to being on job searches and need to keep clean urine for drug tests. I now also have acquired COPD and sleep apnea as well. I need medical marijuana legalized here in my Midwest state USA.
Can’t wait for it to be legalized in nc america
An organic asthma remedy ever accepted. The benefits of cannabis as displayed here sound pretty amazing. Great alternative to allopathic approach.
I’m a 34 year old asthmatic, I have suffered since about 13 or 14 years old ( about the same time I started smoking tobacco and other herbs)
When smoking cannabis, until recently I’d always mixed with tobacco like most people here in the U.K. That always caused me issues with my asthma and I would suck through inhalers in a matter of a week or so.
Recently I changed to smoking blunts (pure weed joints) and found that with 1-2 single skin joints plus a couple hours excercise a day my asthma felt a lot more manageable. I barely used my rescue inhaler at all and cut my steroid inhaler down to one puff a day as opposed to the recommended 4.
A couple months ago I bought a Volcano. As vaping is meant to be the healthier way to consume cannabis. Currently I’m a little disheartened as my lungs seems to be worse then when I was smoking blunts. The taste is great, no heavy smoke to suck into your lungs yet my respiratory system feels like I’m smoking a twenty pack a day.
I’m hoping that this is just a transition period and maybe my lungs will adjust after they’ve rid themselves of the dirty toxins that have accumulated, but I’m not sure right now. Will have to give it another month or so. On the plus side I have come of all medication for the moment but am struggling a little at nighttimes.
On the subject of edibles however, I have always found that the day after consuming them I cough up lots of gunk from my lungs, like it actually has a cleansing effect. Not sure this is common but it definitely has an effect on me 🙂
I have ashma and I would like to know more about this
I ALSO HAVE ASTHMA. i have been using cbd with VG in a sub ohm vapor tank. I put 5 drops in the coil and inhale it, holding it for 5 to 10 sec. I cough up all kind of slim and nose runs. Hard coughs. relax and it seems to dry out my lungs where I can breath. Last about 12 hrs. repeat if necessary To me it is better then inhalers and symbecort.
I HAVE COPD. I WOULD LOVE TO BE IN A RESEARCH STUDY FOR THIS.
is there a doctor in Georgia that will put you on cannabis oil for asthma
I’m a bad asthmatic on oxygen bottles n died 5 times etc etc I started smoking Marijuana n was in hospital less however my method of having it is no better for my lungs what would be good options for a poor guy
Wade, the way I prefer to take cannabis is via a $2.59 stick of good quality, unsalted butter. Once made, I use it like any other butter and LOVE the taste of it. You can find lots of how-to’s on the Internet. It takes a while to make it…about 6-8 hours. But 99% of that time its just simmering on the stove. Read how to deoxycarbolate yer herb, a very important first step. Good luck. Please share your experience if you try it.
I have copd and smoking mj is good for me
I smoke marijuana daily and consistently. I love in the Midwest where the allergen/pollen & air pollution is the highest in the country. My asthma was something that had to be controlled everyday by morning pill, steroid inhaler and emergency inhaler (which at certain times of the year I would use daily). Ever since I began smoking again, I do not have as many problems and complications as I did before. It was almost daily that I needed to use my rescue inhaler and now, smoking every day, I use it once in a blue moon and I have stopped taking my daily meds. I HIGHLY recommend it! Plus you just love life and are happy about everything. The paranoia goes away as the taboo of MJ is becoming minimal for places like this.
Laura, I am so happy that you shared your good results =) ! Your comment is very encouraging.
I have long felt that the healing effects from my experience with cannabis 4 decades ago was remarkable. I have not yet been able to convince, even loved ones who would most likely benefit greatly from treatment.
So thankful that more and more people are benefitting, and are sharing their positive experiences. C Martin
So cannabis can help people with Asthma ? So it isn’t bad to smoke cannabis when having asthma ? Just wondering because I have Asthma and would love to know
Make sure you use a vaporizer rather than smoking it
marijuana vaporizer ? name of that please..
What vape is the best to smoke out of
I did notice when I did smoke recreationally years ago, I never picked up my puffer/inhaler once. When I quit, I’ve had to use my inhaler quit a few time, and I hate the side-effects I get when I use it.
I AGREE with you, also having heavy asthma, since i smoke weed recreationally i never used inhalers again, if i stop for 1-2months i need it sometimes but it isn’t as bad as it was before i smoke, so i think it helped alot.
Same here. I’ve been using my inhaler more and more lately, and noticed when I did smoke recreationally years ago, I didn’t use mine either. Same like you I HATE the side-effects.
This is so true I stopped smoking cannabis one year nw back then if I’m going to schl I’ll buy packs of drugs incase of an attack ,I’ll end up being them back home unopened, some even expires …Now that hav quit cannabis have had back to backs series of attack like in a week I have like 2 attacks minimum.
I have bad asthma and I cough a lot and have a hard time taking a deep break at times. Sometimes my albuterol works but not all the time. I was having bad asthma from a bad cold one day, so decided to smoke some weed to see if it worked. Within 30 min, I noticed a huge difference with being able to take a deep breath and my cough all but went away. It definitively improved my asthma signifintely. Not saying it works for everyone but it helps me a great deal.
I have both asthma and a auto amune called Chung Strauss . I am testing now some eatables to see the effects of the THC . ON MY symtoms. I have also had the response you had on smoking, my tightness definally went away. I will stay in communication on the effect of the eatibles. Mike
“Smoking” cannabis is not good for anyone and can damage the lungs. So ‘vaping’ it might be a better method of delivery. I’d like to know if the cannabis must be inhaled to help the lungs or if other MOD’s might help help the lungs too (although edibles are hard to dose). Do the cannabinoids end up in the lungs even if they’re not inhaled?
Ok folks ive had asthma for 45 years and have been useing salbutamol for 45 years ,.I have found that when my sprays are not working and i may take to much ,then i would have smoke of pot i found my asthma would clear but i would be come shakey but only to over use of of the sprays ,after awhile when the sprays would wear of i felt good and had no need to use sprays .pot most deffently help my asthma a lot but after smoking pot and and a25 cigeretes a day it was killing me of course ,Iam now 52 and recently come down with BRONCHOPNEUMONIA not fun right ,Ihave since stopped smoking the cigs and and stopped my pot smoking ,,Now for the good news i had some left over pot which i made some canni butter my asthma tottaly cleared up ,i had the shakes a bit untill the salbutamol worn off i can honestly say that my asthma felt like it was gone ,my wife says i should make some more canni butter ,i hate over useing sprays ,if i could i would like try pot in tablet or use the mister thing ,but i can tell you that eatting pot in a home made butter which i put on a sweet bun was the best tratment i ever had and it lasted for 24 hours ,its not good to smoke any thing for a long time ,and now waitting for pot to grow so i can make some more canni butter its the best thing ever just have to be carefull not to eat to much ,as i dont like being to stonned ,
Smoking weed helps me. I smoke it in pipes.. avoid rizzlers. I need advice on getting oil tho i hear it can cure.
You dont smoke cannabis you use cbd oil and its vapor. Use a vape pen. This is my first day using cbd oil in a vape pen and the tightness in my chest is gone already. I am not ruining for my inhaler. I love it I almost started cring. I hsvnt been able to breath like this for years. Docotrs kept trying to shove steroids down me. I said enough I am tr6ing
Where do I get a vapor pen and cbd oil? I have been in hospital for asthma, and struggle every day , Thanks
Hi Shirley,
Depending on where you live, you may be able to order our products. Here you can find information about CBD e-liquid, which can be used in most vape pens. Here you can find a map of places that our products can be sent to.
With best wishes,
Scarlet
What oil are you using? I am paying over $7,000 a month with no results and will be out of work for a year due to my asthma. I am looking for anything that might help.
You can medicate using Cannabidiols in a variety of methods; smoke dry herb, dabs/ shatter, oils- auroma, vape CBD, THC. More ways to smoke, I’m probably forgetting.
Other ways Cannabidiols are useful are; edibales (drinks, snacks, candy….ect), pill form, suppositories, topical creams, bath additives, tenures, crystalline. Again, more I’m probably forgetting some.
THC (I believe THCA does as well) gives you the “high” effect in any form; which depending on the strain, method and potency I can notice a difference in my asthma. Other factors include if my triggering antigens are active or if I’m experiencing a cold or if when a sinus infection develops and that exasperates my asthma and lowers my blood oxygen levels. So then I can’t breath and that sucks!
CBD, CBDV, CBDA, THCV and so many more Cannabidiols don’t give you that “high” feeling. They do have so many other bennifits; anti-cancer properties, calming/stress, sleep, fatigue, nausea, appetite, memory, mood (TCH helps with most of these too). I prefer something with a THC and CBD mix and perfer a higher THC% to CBD%. I enjoy smoking dry herb, pills, edibles and what not but vaping concentrates is my main (and most convenient for me) method right now. I’m not a fan of dabbing as it includes knives or nails or blow torches and a number of just dangerously hot and sharp objects. Lol, just my opinion but not against it either. I believe there are a number of methods to dab these days, I’m just not hip to the game that’s out there so much.
Cannabis helps me in a variety of different ways but for my asthma helps; relax muscles/ airway, reduces illnesses/ quick recovery if I get sick, sleep, alter mood (everyone has ups and down but we wouldn’t know what the ups were, if we didn’t have the downs), ect. All of which can and do effect my breathing at times. If I’m out for a hike, am medicated and something triggers an attack, it’s happning but already being medicated helps my body to relax the tightening in my chest and rapid, wheezing breathing….which for me can be worrisome/panic- even if I don’t think I necessarily “panic,” when I can’t breath it’s very scary at times.
State’s are coming closer and closer to FDA approval, state laws and federal legalization.
I believe (I have my MMJ card, so I’m not 100%) CBD oils and pills are legal to all because they don’t produce the high effect of TCH.
This is just some of the ways how cannabis has benefitted me in my life. Please research, become aware, advocate, spread knowledge and most of all have a wonderful day!
Thanks for reading, Mahalla
I have had athsma every since I moved from California to Missouri, I guess clean air made me have asthma or something but I have been smoking marijuana for years and have found that it is a great expectorant expecially when my sinuses get acting up, which usually triggers my asthma.
Granted I usually throw up a ton of mucus but after I can breath better than I do normally, it keeps my asthma under control better than my inhalers do, and when I have a attack I smoke a few hits and it instantaneously goes away, and then I have no problems at all.
Now that my inhalers cost $270 a inhaler every month, I haven’t been buying them and have been relying on marijuana because it’s cheaper, by a lot.
But now I don’t smoke anymore for about 2 years and haven’t had a episode yet, I have my inhalers just in case but haven’t used them, and I honestly think it’s because all my marijuana smoking has reversed everything.
I just wish it was legal everywhere because it’s dumb seeing that cigarettes which are Uber harmful are legal but marijuana which is benefitial isn’t in most states, makes no sense at all.
I’ve had asthma as a kid and can honestly say that since I’ve started smoking weed (over 15 years ago) I’ve never had an asthma attack… Ever! They say you grow out of it but some don’t, can’t say that I did, all I can say is that it worked for me
Depends…I have asthma and can be really sensitive to smoke so it really starts my asthma so if I was to do cannabis I’d probably do the oil. You might be different, it might not affect you the same way!
cbd can be taken orally, no smoking necessary
I want this badly
I can benefit from this
I have been using CBD oil to help with my asthma and found that it helps a lot. I have Lao found that there is some expectorant properties that have helped too. I would love to be in a research group for this if it helped other asthmatics!
Kim,
Which brand cbd did u use??
I have asthma and want to use cbd VG based… I’ve read up medical journal on the
positive properties of cbd on the bronchioles ad it’s anti inflammatory
I have asthma and copd
When I smoke and I smoke all the time.cannabis actually helps me to get the mucus up to where when I don’t smoke it tends to fill my chest with mucus and I can’t get it up.cannabis makes you cough and when you do it often brings up the mucus fluids that has settled in my chest.when I go without it the mucus builds up in my chest which causes me not to breathe rite.it also helps with the pain that it causes in my chest due to the asthma and cold.
I am asthmatic and experience attacks whenever i have flu or when i encounter smoke, perfumes, dust etc…how can i use cannabis seeds at home or where in South Africa can i buy them prepared to be used.
How do i noe wen my baby is aving an a tack
i’m not a doctor,and you should research all avinues about jnfant asthma…i was diagnosed at age 3….first ,,,there might be irratibillity,maybe accompanied with some wheezing ,,,then lathargic and shallow breathing,,,,baby may turn red faced,,or even pail from lack of oxigen ,,,,extreme cases the baby goes blue,,,,,you should have your baby at an “”er”” long before this happens ……i almost died many times from asthma,…literally suffucating,,,,,months in intensive care under o2 tents..they new very little about it in the 60’s and 70’s…………used to have to take addrinolin shots when having an attack……hope this helps…..research google also..talk to clinics…and your baby’s doctor…..know your baby’s triggers….good luck…….jeff a.
How long did you use it before you felt a difference?
The improved breathing was almost immediate to some extent, but the substantial and sustained effect resulted from regular use. I’m a lifelong asthma sufferer & my condition had escalated to a “mild copd” diagnosis as breathing problems became chronic. After trying vaping medical grade oil for anxiety, insomnia- I noticed my breathing was greatly improved.
I’ve subsequently determined that there’s a direct immediate effect,
not unlike using a puffer, but more so a lasting effect from regularly vaping or ingesting med-mar. Before med-mar I could barely climb stairs without reaching for a rescue puffer. Now I’m hiking, exercising and rarely in distress.
One thing, I’ve found is that a 85/15 thc/cbd ratio work better for me, which I take at night, and ingest a 50/50 blend during day. And specific brands (which will have its own distinct blend of the myriad cannabinoid compounds) work best for me.
This n similar blogs so helpful as when I convey my experience with med-mar to doctors they generally respond with surprise & dismiss it as a curiosity. More research and educating of physicians of this treatment should be explored.
Med-mar has literally has changed my life, but finding consistency with product and effect has been a challenge.
What is the name of the cannibis product you are using for Lund/ bronchial issues?
Is it true that allergy to cannabis is affected by THC and is not protected by using a vaporizer?
Interesting, well-researched article. Perhaps needless to point out, but imo a vaporizer is still the safest method to consume (medicinal) cannabis, especially so for asthmatic cannabis users.