Endometriosis is a chronic and disabling disease unlike any other that only affects women. Ironically, even though it afflicts millions of women, it is known as the ‘silent disease’. Let’s take a closer look at this major, but little-known condition and find out what research suggests about the potential therapeutic benefits of cannabis in its treatment.
Despite being referred to as the “silent disease”, the number of women worldwide suffering from endometriosis is more than 176 million. According to data available today, one in 10 women has endometriosis, and young women aged 25-35 are the group with the highest incidence.
Sadly, as a result of ignorance and the silence that surrounds this condition, many of these women see their lives tied to illness, pain, suffering and incomprehension. Endometriosis is a chronic and disabling disease like few others. It significantly affects the quality of life of women and may have devastating consequences for their fertility.
Due to poor clinical knowledge and lack of resources for research into the causes and treatment of this disease, many women go undiagnosed for years. Many of them see several specialists and even undergo surgery before getting an accurate diagnosis, even though the number of affected women is growing considerably every year.
What is endometriosis?
Endometriosis occurs when the endometrial tissue is present on organs other than the uterus inside the female body. Endometrial tissue is what makes up the uterine lining and is what women lose each month during menstruation.
While most of the time the tissue grows around the uterus, it can also spread to other parts of the body – such as the peritoneum, fallopian tubes, bowel, bladder, and other parts of the abdominal cavity. This leads to the formation of endometriomas or endometriotic cysts. There have been some cases in which endometrial tissue has reached the lungs or even the brain.
Pain and other symptoms of endometriosis
The main symptoms of endometriosis include severe pain, irregular bleeding and reproductive problems such as the inability to become pregnant or repeated miscarriages. Pain caused by menstruation, also called dysmenorrhoea, is generally physiological pain provoked by inflammation suffered during menstruation.

In the case of endometriosis, pain also occurs at some other times: abdominal pain and cramps before and during menstruation, pain during or after sexual intercourse (dyspareunia), painful bowel movements, pelvic or low back pain. The discomfort can be so severe that some women compare it to the pain felt when having a heart attack.
In addition to all the unbearable pain brought about by this illness, many of these women also suffer from vomiting, fainting and extreme irritability. Endometriosis is a condition that severely affects both the professional and personal lives of women.
Today, the belief that it is normal for women to experience (severe) menstrual pain is no longer tenable. Some specialists argue that the normal menstrual cycle does not have to be painful, and that premenstrual pain should not even exist. Hence, when both pains occur there could be a neuroendocrine alteration in the body.
The often long-awaited diagnosis
Although the average time to diagnose endometriosis is approximately 7-8 years, some women with this condition have had to wait for almost 30 years. Even though endometriosis begins with the first menstrual cycles during adolescence, patients unavoidably endure terrible pain before and after their physician can to diagnose them correctly.
This is what endometriosis patients tell us in the revealing and very interesting documentary, Endometriosis, the tip of the iceberg, produced by Radio Televisión Española RTVE in 2010, which is available online with English subtitles.
As mentioned earlier, in some cases, the average number of specialists that a patient goes through to get an accurate diagnosis is between 5 and 6, or even more. It is estimated that 25-50% of infertile women have endometriosis and currently, it is one of the most common pathologies in gynaecology.
What causes endometriosis?
Although the scientific community continues to grapple with the exact causes of endometriosis, there are different theories regarding its origin.
Until now, possible causes of endometriosis include:
- Genetics
- Immune system disorder; some experts hypothesize that endometriosis is an auto-immune condition
- Bacterial contamination of the pelvic environment
- Chemical pollutants in the environment such as dioxin
Several factors have also been identified that put women at a higher risk of developing endometriosis:
- Starting menses at an early age
- Going through menopause at a later age
- Short menstrual cycles
- Heavy menstrual periods that last longer than 7 days
- Low BMI
- Reproductive tract abnormalities
- Higher levels of oestrogen in the body
Common treatments for endometriosis
The type of treatment that is given to patients depends on their age, the severity of their symptoms and their illness, and whether or not they want to have children in the future. Depending on each of these cases, there are a variety of treatment options.
Since one of the main symptoms of endometriosis is pain, analgesics are a common form of treatment. For mild symptoms, physicians prescribe hormonal therapies such as birth control pills, but even if they provide relief, they fail to prevent scarring and cure any damage. Progesterone pills/injections and gonadotropin are also effective treatments, but they have significant side effects.
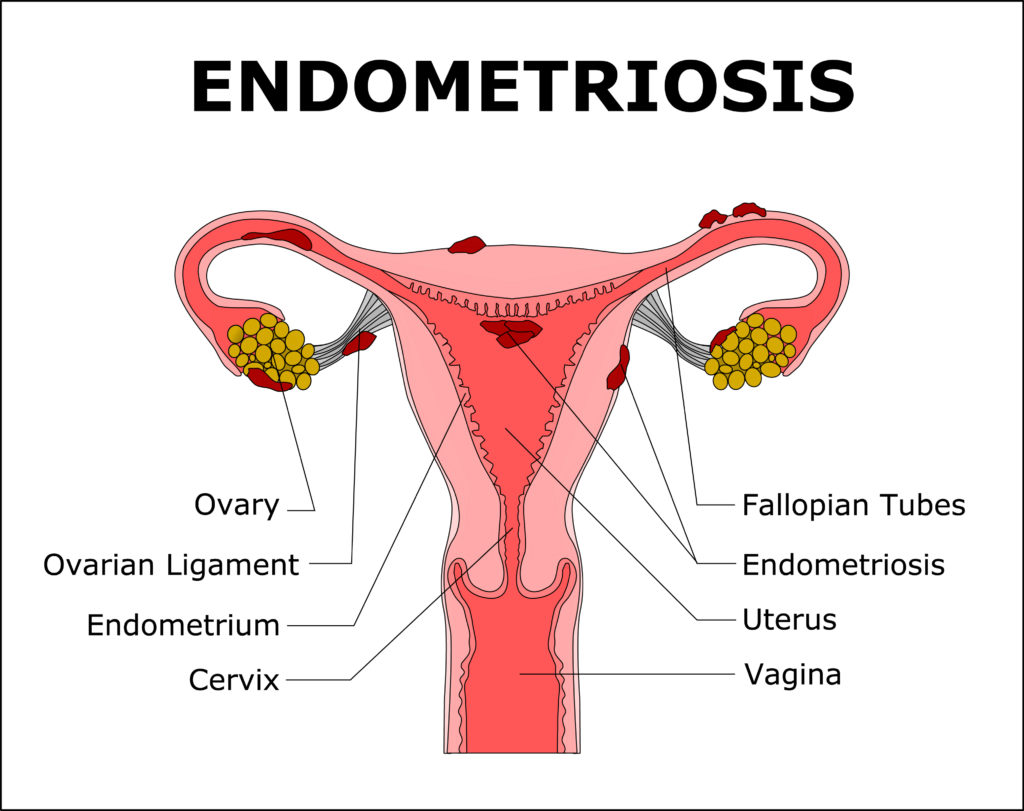
Surgical treatment is the most frequent way to treat severe symptoms that do not go away with other methods of treatment. Laparoscopies are usually carried out to help diagnose the disease once and for all and can also eliminate cysts and scar or endometrial tissue. Other techniques used are laparotomy and hysterectomy, the latter being the most aggressive surgery of all and usually the last solution.
As some of the patients in the documentary mentioned above describe, after many of these surgical operations, patients realized that not all endometriosis plaques were removed by the surgeon.
Endometriosis cells reproduce quickly forming a plaque of tissue as hard as marble, which is why the disease often relapses. This is why it would be fundamental to remove all the endometriosis nodules in a single optimal surgery.
It is clear, therefore, that there needs to be a consensus in the medical community regarding the treatment of endometriosis so that new, less aggressive methods of treating this condition can be developed. There is a great deal of scientific evidence currently available showing that the use of medical cannabis has excellent potential to help women suffering from this illness.
How can medicinal cannabis help treat endometriosis?
As previously explained, endometriosis is a chronic disease that has no cure. However, women’s own experience controlling the disease and scientific research, show that cannabis may be a highly effective therapy.
Today, science has identified cannabinoids, the active substances contained in the cannabis plant, as a new type of medicine that needs to be considered and further studied. The most researched and studied are THC and CBD, but there are more than 100 known cannabinoids. In addition, cannabis contains other compounds such as flavonoids and terpenes, which are also being studied for their entourage effect.
The proven beneficial properties of cannabinoids can help alleviate many of the symptoms produced by endometriosis, such as pain, depression and anxiety, fatigue, inflammation and vomiting, to name a few.
Medical cannabis for menstrual pain, inflammation and cramps
In addition to having analgesic properties, cannabinoids also have anti-inflammatory and antispasmodic effects. They are administered orally (CBD oil or capsules) or via intravaginal routes (vaginal suppositories), to help with menstrual pains.
There are different ways to use medical cannabis, so it is recommended to take into account a number of practical considerations for proper use and dosage, and always consult a physician. Smoking is the quickest way to notice the effects of cannabis while ingesting it takes longer, but the effects last longer. A better alternative to smoking may be vaporizing your buds. Suppositories and topical creams can also be viable options, they act in a more localized way.
The anti-inflammatory properties of cannabinoids and other cannabis compounds are enhanced when administered together. They are useful in reducing pain produced by menstrual inflammation. Hence, thanks to their analgesic properties, patients suffering from pain can improve their condition, but in specific ways depending on the cannabinoid and compound used. In addition, their spasmolytic effects help reduce menstrual cramps.
At present, research indicates that cannabidiol or CBD, the main non-psychoactive component of cannabis, reduces inflammation associated with chronic inflammatory states. It also acts as an antioxidant, potentially inhibiting the development of various types of cancer.
In the case of endometriosis, the cells covering the uterus (endometrium) may bleed, releasing inflammatory mediators and causing pain locally. With the use of cannabidiol, patients can significantly improve their quality of life by reducing pain. In many cases, patients even stop taking other types of medication.
Endometriosis and the endocannabinoid system
Endocannabinoids are natural endogenous cannabinoids produced by the human body. They serve different biological functions and activate the cannabinoid receptors CB1 and CB2. Due to the importance of this system, drugs that may interfere with cannabinoid activity are now considered candidates for the treatment of various diseases, including endometriosis.
The body’s endocannabinoid system is a network of cannabinoid receptors that modulate our cerebral, immune and endocrine functions, and is essential for proper functioning of the female reproductive system. Since its discovery, research has continued to show interest in the potential of cannabinoids to treat diseases affecting the female reproductive system.
It seems that imbalances occurring in endogenous cannabinoid levels are often related to complications and diseases of the female reproductive system, including endometriosis. Proper use of cannabis products such as topical creams, oils or suppositories can help restore balance in the body.
Cannabinoids also have properties that may be used to control another significant aspect of severe endometriosis: cell multiplication. Cannabinoids regulate cell growth and cell migration due to their role in proliferation, apoptosis and angiogenesis.
Their antiproliferative effects are the result of the inhibition of growth factors and the deregulation of signalling pathways. Since endometrial cells have a hyperproliferative phenotype and proangiogenic properties, the use of medical cannabis may help prevent the disease from reappearing.
What else does science say?
In the case of women who have deep infiltrating endometriosis (DIE), an even more painful form of this disease, it is believed that the lesions found in deeper regions contain a much higher density of nerves than others.
Research suggests that endocannabinoids regulate nerve growth and that CB1 receptors are found in the nerves that supply endometriotic lesions. According to the results of a study, “the inhibitions of CB1R and its downstream ERK and JNK signalling pathways may alleviate the sprouted innervation that has been involved in ENDO-associated pain”. This “may provide a new therapeutic target for patients with endometriosis”.
Many of the endocannabinoid receptors, particularly CB1 and CB2, are found in endometrial tissue. Studies on rodents with the disease show that these levels are regulated by the menstrual cycle. Furthermore, the highest concentration of endocannabinoid anandamide (AEA) in the reproductive system is found in the uterus.
Researchers have discovered that CB1 cannabinoid receptors are present on both the somata and in the fibres of sensory and sympathetic neurons that innervate endometriosis’ abnormal growths. CB1 receptor agonists appear to decrease the hyperalgesia associated with endometriosis, while CB1 receptor antagonists increase it.
These findings suggest that the endocannabinoid system (ECS) contributes to the mechanisms underlying the peripheral innervation of abnormal growths and the pain associated with endometriosis. Thus, it seems clear that endometriosis may be related to clinical endocannabinoid deficiency (CECD).
It has been shown that reduced ECS function causes endometriosis to spread throughout the body and increases pain. In fact, women with this condition have lower levels of CB1 receptors in endometrial tissue, and since this receptor regulates pain, patients suffer more.
There is evidence that human endometrial cells increased, except when stimulated with a synthetic cannabinoid known as WIN 55212-2. Endometriosis studies in rodents have revealed that the animals had more pain when treated with AM251, a drug that inhibits cannabinoid receptors, and less pain when treated with WIN 55212-2.
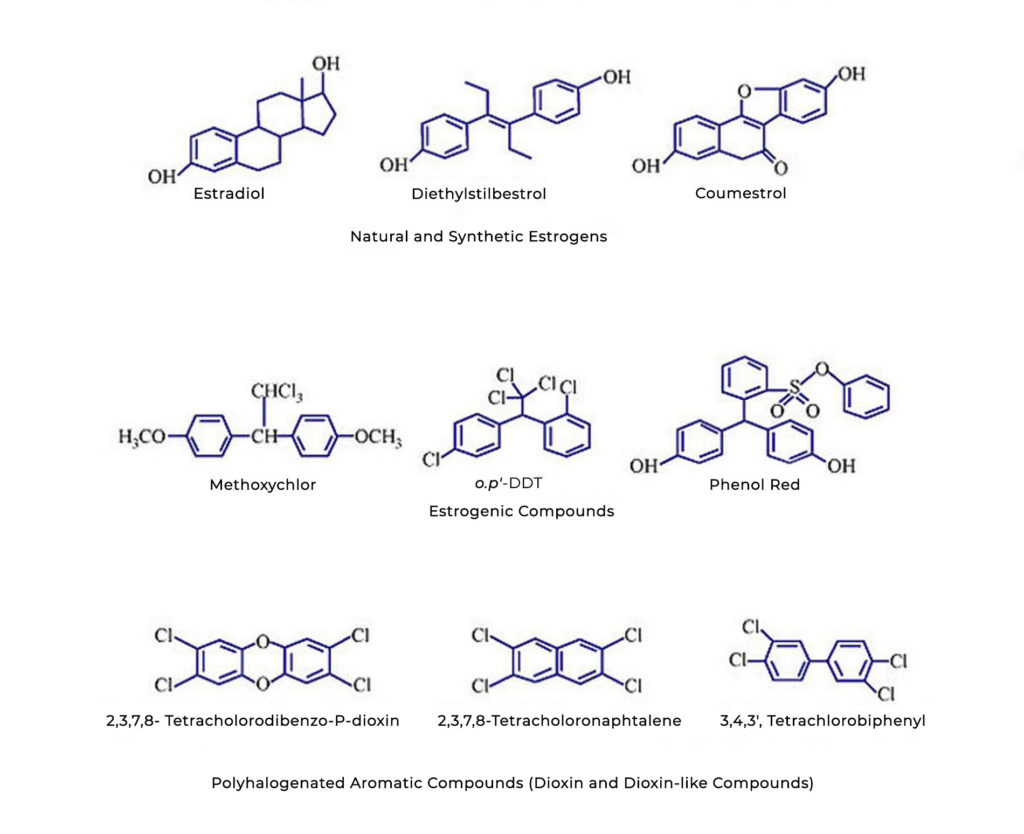
Environmental toxins, such as dioxin, have also been linked to endometriosis and CECD. Dioxin is an unintentional by-product of many industrial processes, especially those involving chlorine, such as waste incineration. Dioxin decreases CB1 levels in endometrial tissue. As we are exposed to air, water, and food pollution, it is not surprising that so many women in developed countries today suffer some form of endometriosis.
Can CBD oil be used to treat endometriosis or ovarian cysts?
There are multiple mechanisms by which CBD oil may help treat the symptoms related with endometriosis:
- CBD has antiproliferative effects, and therefore may stop the proliferation of uterine tissues in places where it should not grow. In addition, this kind of medical intervention may prevent relapse after treatment or surgery.
- CBD has analgesic properties, and therefore may simply be an effective treatment for the management of pain related with endometriosis.
- Ingestion of cannabinoids may address the imbalance in endocannabinoid and cannabinoid receptor expression that is observed in women with endometriosis. However, this is yet to be confirmed by scientific research.

Some women with endometriosis also have ovarian cysts. While the endocannabinoid system plays a role in the human ovary, there is no scientific literature that suggests that cannabinoid treatment for ovarian cysts is effective.
Research to develop new cannabis treatments
There is no doubt that the data available suggest the need for further investigation into the levels of endocannabinoids in women. It is necessary to determine whether they are lower in the plasma or endometrial cells. With this information, we will be able to know if endocannabinoid levels change throughout a woman’s menstrual cycle, as is the case with rodents.
Thus, we could determine whether women treated with cannabinoids experience less pain and reduced endometrial growth, or whether women using cannabis are less likely to develop endometriosis, as some of the studies to date seem to indicate.
As explained earlier, at the moment it is very difficult to diagnose this disease. A simple biomarker, such as a reduced level of endocannabinoids in the blood or endometrial tissues, could save millions in healthcare worldwide. Plus, it may save years of unnecessary pain for the millions of women who suffer from this disease.
While further research is needed to determine exactly how cannabis may benefit patients with endometriosis, evidence from research shows very promising results, as does data obtained from medical cannabis patients. The potential for cannabis to help women manage the symptoms of this disease and improve their quality of life is now rather obvious.
Are you one of many women who have endometriosis? Have you ever used cannabis, cannabis oil or any other cannabis product to treat the symptoms of endometriosis? Tell us in the comments below!
- Disclaimer:This article is not a substitute for professional medical advice, diagnosis, or treatment. Always consult with your doctor or other licensed medical professional. Do not delay seeking medical advice or disregard medical advice due to something you have read on this website.














This blog article provides a thorough examination of the potential of cannabis to alleviate endometriosis-related pain and symptoms, offering valuable insights for those seeking alternative therapies. As someone who has researched medical cannabis for pain management, I find the information presented here to be both informative and insightful. The comprehensive overview aligns with my own experiences and understanding of the potential benefits of cannabis in managing chronic pain conditions like endometriosis.
Thanks for the info about CBD. My wife is trying to get more information about CBD suppositories.
Good morning Max,
Thanks for your question!
I’m glad you found the article interesting,
Fortunately, we have an article on ecreational Rectal Use of Cannabis (Or, What I Did for Science)
Hope this answers your questions.
With the best wishes,
Mark
I am intrigued with the Cannnabis possibility of helping relieve pain, inflammation, etc. I was diagnosed over 17yrs ago, had a partial hysterectomy and my Dr. hoped it would give me 10years before it was back. Well, 17years later it is here with a vengeance at times as I lie on the couch in pain, have little to no energy and am overly tired. My normal chipper self is lacking. I was re-diagnosed a month ago and best option is surgery once again….. However, I would prefer to avoid it if at all possible and have been researching and changing lifestyle a little more than I had already in hopes to do this naturally with eating habits, exercise & supplements (vitamins, minerals and oils I am lacking) per my research. I have really implemented this once verified I wasn’t losing my mind this past year with symptoms and I haven’t had a period for over 17yrs so hard to know if associated with that time of the month or not but I do have both ovaries. My left ovary looked good but my right has a very visible 4cm mass and likely more in and around the normal areas. Pain sometimes comes and goes but can usually feel it if I position myself incorrectly, sex hurts (very hard for me as I don’t say much to my husband of 24yrs as I don’t want him to feel bad and just try to reposition myself)…. pain has increased and sometimes makes normal day to day hard as it’s in my low back, front ovary area as well as hurts and aches more often than not inside my right vaginal area (sorry to be so descriptive). Does anyone know if you can just use the Oil topically? Will it help as I know it has helped some of my friends from other ailments from arthritis to broken ankle hurting when walk too much to do the damage but when using the oil/lotion can walk miles and swelling stays down. I am NOT a smoker, I am a lightweight the couple of times I have tried it and would feel better doing it topical if I can find out if it has helped others this way before wasting my money….. Please, if you have tried it or no someone whom has please let me know as I want my normal quality of life back, hubby has been on the road luckily everytime I have a really bad few days so he doesn’t know how bad it really is affecting me.
Hi Robin,
Thank you for your comment. I’m really sorry to hear about your situation. Don’t apologise for giving details – there is no shame in what you are going through and we’re all adults here. I’m obliged to give you the answer below, but hopefully someone with direct experience can let you know if it worked for them. My personal opinion is that using oil topically would offer some relief; I have not tried it vaginally but I have tried rectal suppositories and they definitely had an effect. You can read my report on that experience here. If you read the comments on that article you will see that suppositories have been used with success by other people too.
You may also wish to investigate a product called ‘Foria Relief’, a pessary formulated to give relief from menstrual pain. Another option could be the products from ‘Whoopi and Maya’ which are developed for the same reason. Although what you’re suffering is much worse than menstrual pain, these products might alleviate it slightly.
As Sensi Seeds is not a medical agency or practitioner, we cannot give any kind of medical advice other than to consult our registered healthcare professional. This article about the potential benefits of medicinal cannabis might be useful for you to show your healthcare provider if they are not familiar with it.
You may also find it helpful to contact a support group for medicinal cannabis patients. In the UK there is the United Patients Alliance, and throughout much of the rest of the world there is NORML, who should be able to put you in touch with a group in your area (search United Patients Alliance or NORML followed by your area name).
These are our pages on medicinal cannabis and medicinal cannabis strains, which you might also find interesting.
With best wishes,
Scarlet
I have an endometrioma on my right ovary. I’ve know about since 2016, after my endocrinologist found one on my left side which was about 1cm and the one on my right was almost 3cm. (Within a few weeks my left one burst, I felt no pain and since then it hasn’t come back).
We tried to find a treatment plan so she decided to put me on spironolactone at first because I have a family history of high blood pressure and strokes. (My grandpa had 5 strokes before he passed away and my mum has had 2 micro strokes. She now takes beta blockers and blood thinners everyday now).
I had started using the spironolactone, I was about 3 months in when the endometrioma on my right side started rupturing, a few months after it was discovered.
I was 26 at the time and had never experienced any sort of pain like that in my life!
My periods were very casual. No migraines. No cramps. No major bloating. No PMS. No back pain…. ZERO! Aunt flow would come, and just like that she was gone. So, when I felt this endometrioma rupture for the first time I literally thought I was in hell. I couldn’t sleep all night from sharp pains. I had a fever and chills, my back hurt so bad there was no position in which I could sit or lie down. I began to throw up, violently. I was in so much pain I could barely communicate with anyone.
Anyways, after being rushed to the hospital and having a bunch of tests performed, (blood tests, CT scans, ultrasounds, pelvic exams) and a lot of drugs were administered I was able to go home. Needless to say I missed a lot of work from not being able to move around without pain for a few days.
Fast forward… I happened once more… and then again. Every time it happened I was baffled. I could not believe this was my life now! I thought to myself… am I going to have to spend my nights at emergency once every month? How could this have happened? I went from never feeling a thing…. to the most excruciating pain I have ever felt! It was unbelievable.
Well, at that point I was already seeing a bunch of specialists: a gynocologist, an endocrinologist, a dermatologist, a haematologist and a neurologist.
To which they all came to the conclusion that it was time to put me on birth control. They were all hesitant at first because of my family history. I was a smoker as well before hand. Many factors…
I had always been a person who did not like to rely on medicine very much, I would rarely ever have to need to take anything. However, the pain I was enduring and the symptoms I was being left with from all the hormonal imbalances, the amount of work I was missing made me panic and so I said okay to trying the birth control.
Over time there was a bunch of trial and error until I found the right one I felt comfortable taking that didn’t make me feel depressed, anger, crazy or that didn’t make my skin react or make my hair fall out.
It’s been about a year and a half of no ruptures. The endometrioma is the same size, 3 cm. Once in a while I can feel it twisting, I’ll feel some mad pokes on my lower side, but it goes away.
My only problem now is the side effects I have with the pill I’m on. I get some serious bouts of nausea and some very unforgiving migraines.. sometimes they’re quick. Sometimes they last for days. And yes, I could never compared these annoyances to rupturing cysts, I am grateful we found a temporary solution. But I have heard that the CBD oil has the ability to shrink down lesions and help with auto immune issues, inflammation and so on, all very much associated with endometriosis, PCOS, and fibroids.
My fear really is me ending up in the hospital with a rupture again. I really do not like being on hormones, you always here about all the way it can affect your health. It’s truly scary.
Finally, my question is how can I transition to using CBD oil? I’m curious if I could take them together or if I go cold turkey and stopped the Birth Control and only use the CBD oil how long before I could see some positive effects? I’ve heard of women treating themselves with CBD oils, do they have to take any other vitamins to go along with it?
Does anyone have a successful transitioning story from birth control to CBD oils?
Great article. I was diagnosed after I had a tubal ligation at 26. My mother had a hysterectomy and they left one ovary in her. She died of ovarian cancer at 54 yrs old. I noticed almost right away the positive effects cannabis had on managing pain. All other treatment options were either barbaric or came with too many side effects, and unfortunately I’m allergic to ibuprofen and nsaids. My pain comes with ovulation and I can go from pale, sweating and in so much pain I can barely breathe (let alone move) to sore but fine in ten minutes.
This article is so well written and educational. As an Stage 4 Endometriosis fighter, I have been thru several major surgeries, including a total hysterectomy. To alleviate pain, I made this decision to undergo a fourth surgery because I had Endo glued to all my reproductive, disgestive, and urinary organs. My surgery left my right arm with severe nerve damage due to laying how I had to lay for 8 hours during surgery. All to alleviate pain. I have been prescribed every treatment possible. Hormone therapy, Lupron cycles, etc…
Point of my story is this. I have been fighting this disease for over 15 years. 10 of which I had an actual diagnosis from a laprascopic procedure turned badly into a laparatomy when they realized the extent of the damage that had already been done by the sticky lesions and 30 day cycles. BLAH.
I WISH THERE WAS A WAY TO PROVIDE THIS RELIEF AND TREATMENT LEGALLY TO WOMEN WHO SUFFER SILENTLY WITH AN INVISIBLE DISEASE.
It hides and grows. The only thing you can do to survive is minimize the growth, the inflammation, the depression from medical expenses and loss of way of life.
Much love to the author of this article and it’s intelligent and educated analysis of this treatment.
Hi I have started to take the 10mg cbd oil 3 days ago started off with 3 drops no relief not at 7 drops still in so much pain with this endometriosis does it take long to get into the system I’ve heard really good things about the oil I’m on a serious amount of medication and would love nothing better to get off them thanks again
Dear Martina,
Thank you for your comment. We are sorry to hear about your situation. Unfortunately, as Sensi Seeds is not a medical practice, we are not able to provide any advice relating to medical situations other than to consult your doctor or other licensed medical professional. This article, written specifically for healthcare providers who may not be aware of the many properties of cannabis, may be useful to you in talking with your doctor. You could also try to contact local medicinal cannabis support groups, if you have not already done so. In the UK, there is the United Patients Alliance (you can find them on Facebook) and in the US and EU there are many branches of NORML (google NORML followed by your area name). We hope this is helpful.
With best wishes,
Scarlet
I am beginning to think that as with Cancer, Endometriosis could be cured with extreme concentrations of CBD or a THC/CBD mix? There are quite a few examples of people going into remission through taking a product called Phoenix Tears, or better known as Honey Oil, in large concentrations at once. The procedure is not cheap, though not as expensive as a Chemo treatment. For instance, you would require 60 grams in 90 days for Cancer, and the average cost ranges in the $40-$70 range per gram, vs $14,000 for one month’s worth of Chemo. If you transfer this approach to Endo, you might have a great deal of relief, if not a movement towards remission of these symptoms?
One thing to point out; When it comes to taking CBD or Cannabis, the only time you will encounter the healing aspects of the plant, vs a short state of ease, is through ingestion. You can smoke until you are blue in the face, and you will not experience the true healing powers of this plant. Once you start to ingest it, you will then be introduced to its true purpose. I would love to see a trial conducted on a group of women where they took Suppositories vaginally of the concentrated Cannabis to facilitate movement towards finding a cure for this? This is a miraculous plant, that has been stripped from us for almost a century due to dubious means. With the resurgence of this product, I would really like to see more “out of the box” attempts regarding ailments such as this.
On a side note, my niece and a friend suffer from this, and we are experimenting with different applications of CBD and Cannabis to facilitate a potential fix for them. They are both young women, and they as well as all others deserve a quality of life.
So, I’m still confused. Is CBD good or bad for those with Endometriosis?
Kay,
In my personal experience, I began using a pure CBD vape pen and have felt a miraculous improvement. I wish I had tried it sooner!! I suffer from chronic back pain among many other endometriosis symptoms, and the day I began using the CBD, I actually shed some tears because I hadn’t felt “normal” or pain free in SO LONG. My mood improved so much, I actually felt like myself again! The CBD when inhaled in this vape form worked almost instantly.
If you use any vape cartridges you must make sure it’s only 100% CBD oil and NOT mixed with anything else. Some brands are mixed with MCT oil (basically coconut oil, which shouldn’t be inhaled!!), propelyne glycol, glycerine, etc.)
I hope this helped you!
well… If it could just get damn legalized, then me and my mom wouldn’t be suffering much longer, ive tried soo many ways to get rid of the pain of my period and tried to stop it by starving myself, but it will not work, then the day came when I did it. I felt better then I have ever before! I could focus in school the day after and was not in the nurse’s office or had to take pain killer! Now I cannot do anything in school and the bleeding keeps going and keeps going! I’m only 13 and need to go see a doctor for a never ending period! I get a break but when I do I’m so pail I can see half of my veins! and tomorrow I have a mile test and I am gonna die
IT’S NEVER ENOUGH!
I was diagnosed with this disease and I was told my whole body was riddled with the cysts associated with endometriosis! I suffer with a great deal of pain and problems and would like more information about it. I was originally put on birth control to help alleviate some of the pain, but was cut off when insurance didn’t want to cover birth control for a 52 year old woman! Plus it was causing other issues for me being on the pill. Also I was told that they would “disappear” after menopause, don’t know if I believe that, but I refuse to have surgery, for one the cysts are EVERYWHERE throughout my body and surgery could not possibly remove it all, plus I don’t want any doctors “practicing” on me! What are the alternatives? Pain killers do nothing for the pain and I hate taking them because of the other side effects they cause, but I can’t bear the pain most days either! I am sick of “experts” that can’t get their facts straight or even have a clue about what they are talking about! I don’t want to break the law for relief but feel the issue really falls on deaf ears, nobody wants to hear about it or cares that I am suffering every day with such pain! What can I do?? I am desperate!
Hello Marcia,
I have endometriosis cysts in both ovaries, and, long to tell… but I am not on birth control pills, and I will not have any surgery (so far). I was in pain almost every month with my menstruation but acupuntcture help me a lot with that; althought it seems to do not work for shrinking the cysts, it is beneficial to reduce inflamation and pain.
What it was very stressfull for me is that the cyst bothered me during my sex relationships. It did not hurt, but it was quite unconfortable. I also use to have unconfortable feelings in my left side, where I have the biggest endometrioma.
In my life I have smoked marihuana… But not all the marihuana strains have the same beneficts. Anyway, during my last holidays my friends gave me to smoke a very good one marihuana that was magic to me… Inflamation dissappeared and I did not felt any disconfort, it was like the cyst dissapeared (although I know it is still there). Due to this experience, I am starting having Organic CBD Oil, it is an oil which is stracted from the marihuana, and it is said it has medical beneficts. It is legal, because there are no high THC concentrations in such oil and you reduces the side effects of smoking… Look for information and give it a try. My firts bottle arrived today, so I can not tell if it works on me or not …
Hello Virginia,
I know it’s been some time since you write your comment above. Can you please tell me if Organic CBD Oil helped you? Did you tried this form of treatment everyday? How many bottles per month? Can you please leave a reply if it happens to come over this message?
Thank you,
Very informative, one of the most inciting articles I have read on this topic. Thank you!
Hope others may find hope from the link below.
https://endometriosisanaturalcure.wordpress.com/2014/10/18/the-silent-female-epidemic-endometriosis-my-story/
This was very helpful:) Thank you for sharing!
Very interesting…I have this disease, took birth control for awhile, but stopped being effective…wished I could legally take a natural treatment for the severe pain and swelling I experience!
The ailment where the endometrial tissue is found on the outer part of the uterus or womb is termed as endometriosis. This stays between the lower part of the stomach or abdomen and the pelvic area. This disease does not spread on other parts of the body. This disease mainly occurs in the endometrial tissue that is accountable for lining the walls of womb. It is completely a feminine disease and has very mild indications. It is observed only when the symptoms get severe or painful. The causes of this disease include surgical implantation and weak immune organization of the body
First off you claim “It is completely a feminine disease and has very mild indications. It is observed only when the symptoms get severe or painful” – from what I understand Indication in medical terms means: a condition which makes a particular treatment or procedure advisable. So “very mild” indication means it is advisable to not treat Endometriosis. I have no words…I am left speechless. That is such awful and dangerous advice. Its actually quite sad.
You also claim: “This stays between the lower part of the stomach or abdomen and the pelvic area. This disease does not spread on other parts of the body.” Why do I, and so many others have Endometriosis on our lungs, and if you’re saying it’s completely Feminine, you are intimating it’s only seen on Female organs. Strangely so many women with Endometriosis have the disease infiltrating their bowel, intestines, bladder, etc. I think men have those organs as well?
Further you claim: “The causes of this disease include surgical implantation and weak immune organization of the body.” So you have discovered the cause of Endometriosis when science clearly says states the causes are unknown (they do give possibilities).
I take high offense to anyone, especially a Dr. misinforming people about a disease that already is for the most part unknown and has a horrible stigma attached to it. I will not have children, I missed 6 years of work due to pain and symptoms, I have pain every day. If you can say a disease that destroys about 35% of the women who have it’s chance to have a family, a disease that is explained in the way it acts, the pain and the exhaustion as a “cancer that doesn’t kill you”, a disease that you need excision surgery for every few years as a bandaid or harsh hormones, a disease MANY cannot control even through life changes, ETC. – a disease which has “very mild indications”, you sound like you don’t know what you’re talking about. I don’t know what kind of Dr. you are, but if you said that to me, I would laugh at you, say some choice words and leave the room. Thank you for being another medical “expert” to misinform the public on a very difficult and excruciating disease – a disease that is on many top 10 lists of most painful diseases.
Whoever reads this suffering from Endometriosis, please do not listen to Dr.’s like this – they will undermine the disease because they truly do not understand it. Find a Dr. that does.
Thank you for your support. I am so appalled at what that person said. I as well have this disease everywhere.
Thank you Elena for representing for your Endosisters, I could not have said it better. You are awesome! Best wishes and healing to you!
-your Endosister
Thank you Elena Maria. My sentiments exactly. I hope no one takes this man’s word as fact. He is clearly uneducated in this area.
I agree with Elena 100%. We who suffer from this disease are forced to equip ourselves with so much knowledge as the doctors don’t really know what to do. I have it everywhere My spine,bowel,rib cage. My heart has become weak because of the severity of my pain. I walk with this 24/7 everyday of my life. I feel some doctors are ignorant when it come to ENDOMETRIOSIS. You need to do research before misinforming patients like myself about the disease we suffer from.
Yes absolutely! thank you for standing up for us. xo
Thank you very much for such an articulate and personal reply to that “Dr.’s” comment! I can’t help but wonder if the comment was an intentional effort to infuriate sufferers of the disease, but either way, your reply was right on point and needed.
Elena Maria if their was a like button on your comit I would have hit liked just wanted to say I feel the same way
Thank you Elena. That person sounded like a fool. I also like you have endometriosis on organs and I’m in pain everyday. I can’t work, it hurts to do anything. It has seriously taken over my life. No surgeries have helped either.
well spoken Elena I to have endometriosis and I have had 2 surgeries already and after surgeries I have had nerve damage to my left side from Endometriosis ! Also in my right eye Endometriosis is detatching my iris… who ever said endo doesn’t spread needs a fact check it goes all the way to your brain!!
Your wring. It does spread. I have it everywhere. Not only do I need a hysterectomy, I also need a bowel reconstruction due to my endometriosis
“This disease does not spread to other parts of the body”. With all due respect this statement is incorrect. endometriosis implants have been found on the diaphragm, lungs and even on the brain. It is documented to have been found in the knee of a MAN!
You’re assertion that one of the causes is surgical implantation is interesting I would like for you to expand on this.
There is growing evidence to show that immune regulation plays a part but whether it’s the cause is not yet known.
If you actually did research you would know that endometriosis has been found in the brain, lungs, and eyes, in women with rare severe cases of endometriosis.
Tara yes finally someone knows what im dealing with!! I have had 2 surgeries from endometriosis, now have nerve damage on left side from nerve damage, its detaching my iris in my right eye its headed to my brain!
I have abdominal wall endometriosis, which was caused from my C-section
it is in my c-section and six pack muscles. very painful and had to have surgery and mesh replacement to replace missing muscles. doctors need to be aware of spreading this during c-section surgeries. and they need to learn to treat iatrogenic (doctor made) endometriosis,
” Very mild indications…” “Stays between the lower part of the stomach…” Endometriosis being an entirely feminine condition does not make it an insignificant one. It can and is often a debilitating condition for those who have to live with it. Its implications affect not only the sufferer, but her family as a whole. Think infertility, depression, chronic pain,repeated surgeries for intestinal obstruction secondary to adhesions. The implants can be found way beyond the boundaries of the”stomach”, as they can be the cause of pleuritic chest pain from pleural space implants, hemoptysis, even headaches and seizures if implants are on the brain, meninges or in the ventricles. Please inform yourself before minimizing other people’s burden. This shows a certain lack of empathy.
What kind of doctor are you Vikram do you have any specific areas of study where did you get your information from ?
I agree with Elena Maria. Please find a doctor that is knowledgeable in endometriosis. Do not let a doctor tell you that something is not wrong with your body when you know it is not right. Perseverance is often required in these situations. Also, it has been documented in autopsies that endometrial tissue had been doing in the lungs & even brain tissue of women (I believe this is documented in Women’s Body Women’s Health, a very inclusive women’s health book by Christina N??????). Remember, it is called “practising” medicine. Be your own health care advocate.
You sir are clearly an uneducated idiot and I pity your patients!
I know for a fact that the endometriosis does spread and attach to other parts of the body, ive had it on bowels, uterus, liver, ovaries, old scar tissue. And yes some women do expierence more milder symptoms, but most have sever pain, and deal with constant side effects do to the disease and medications, and not to mention some women can not have children or have complications at birth, with not being able to carry to term. Im not sure what kind of doctor you are, but i hope not one for womens health. I suggest you do some more research!!
no way dude. This disease is similar to cancer and can spread. I’m not even a doctor bt I can tell you that it can spread to the brain. My wife has stage 4 endometriosis and she’s been taking pain killers for as long as I know her. I am so afraid of all the pills she takes because of all the toxins it might build up in her body. I am now doing research on cannabis oils and how effective it could be for her disease. If anyone can please shed more light around the cannabis treatment. I am from South Africa.
Thank you
I am living proof that endometriosis reaches other organs. I am scarred on my entire intestines all the way down to my anus. My left ovary was removed with my tube. She knew she needed to remove the rest but she didn’t because she wanted to help me conceive. As a woman suffering from endometriosis I wish my state would allow medical marijuana so I can try it. Doctors should be taught fully about endometriosis. It has been around long enough there is No excuse. Women should be educated about it as well. It is a life threatening painful dangerous disease and it should be treated seriously. If I didn’t go for my first ultrasound for my pregnancy which I lost along with every pregnancy I lost I would probably be dead because I was bleeding internally from my ovary. When u go to the hospital for this they treat u like your overreacting about the pain and send u home. So, I’m not surprised to read more about how medically educated people have no real idea about this disease or why they want to assume that they just might not really know what they are talking about. This article and many others should be brought to every doctors attention and taught in schools everywhere.
Come to Maryland and DC. It’s legal here. I’m using marijuana as a treatment and it is actually working. If it can reduce my endometriosis then it’s good enough for me. Also it has helped my depression too.
I had excision surgery with a specialist widely known in the endometriosis community. He found endometrial tissue embedded in my hip, thus why I experienced excruciating pain twice month. Your ignorance as a doctor is shocking.
Doctor? Doctor of what? Quackery? There was a famous case where a MAN in Japan being treated for prostate cancer developed endometriosis. This has happened in SEVERAL men and there is readily available peer-reviewed medical articles on this. If you ARE a doctor, you have no excuse for your ignorance and should be ashamed. I bet you think Sampson’s theory of re-flux menstruation is true, as well, or that uteri wander inside of women and make them irrational.
Mr. Vikram (I won’t call you a doctor) are seriously mistaken and you sound like a quack.
interesante el articulo
Very well written article,thankyou so much.